How to Choose the Right Group Health Plan

Jason Stolz CLTC, CRPC
Choosing the right group health plan is one of the most financially significant and culturally impactful decisions a business owner can make. Health insurance is not just an employee benefit — it is a strategic lever that affects recruitment, retention, morale, productivity, tax efficiency, and long-term business stability. The wrong plan can create frustration, rising costs, and constant administrative headaches. The right plan can strengthen loyalty, reduce turnover, protect leadership, and position your company competitively in the marketplace. But selecting that plan requires more than comparing premiums. It demands a clear understanding of workforce demographics, contribution strategy, network design, deductible structures, compliance obligations, tax treatment, and long-term cost trends. Group health insurance is a moving target influenced by carrier underwriting, participation requirements, regional provider networks, and federal and state regulations. Making a smart decision requires aligning coverage design with business goals — not simply choosing the lowest quoted rate.
Before evaluating plan types, the first step is clarifying your objectives. Are you trying to control costs predictably? Compete for top talent? Reduce turnover? Improve employee satisfaction? Protect executive leadership? Support a remote workforce across multiple states? Each goal influences plan structure. For example, a company focused on recruitment may prioritize broader PPO networks and lower out-of-pocket exposure. A company focused on predictable budgeting may lean toward higher deductible plans with defined employer contributions. A fast-growing startup may need flexible participation thresholds and scalable plan options. Without defining purpose first, business owners often compare plans purely on monthly premium — which can lead to unintended long-term cost exposure.
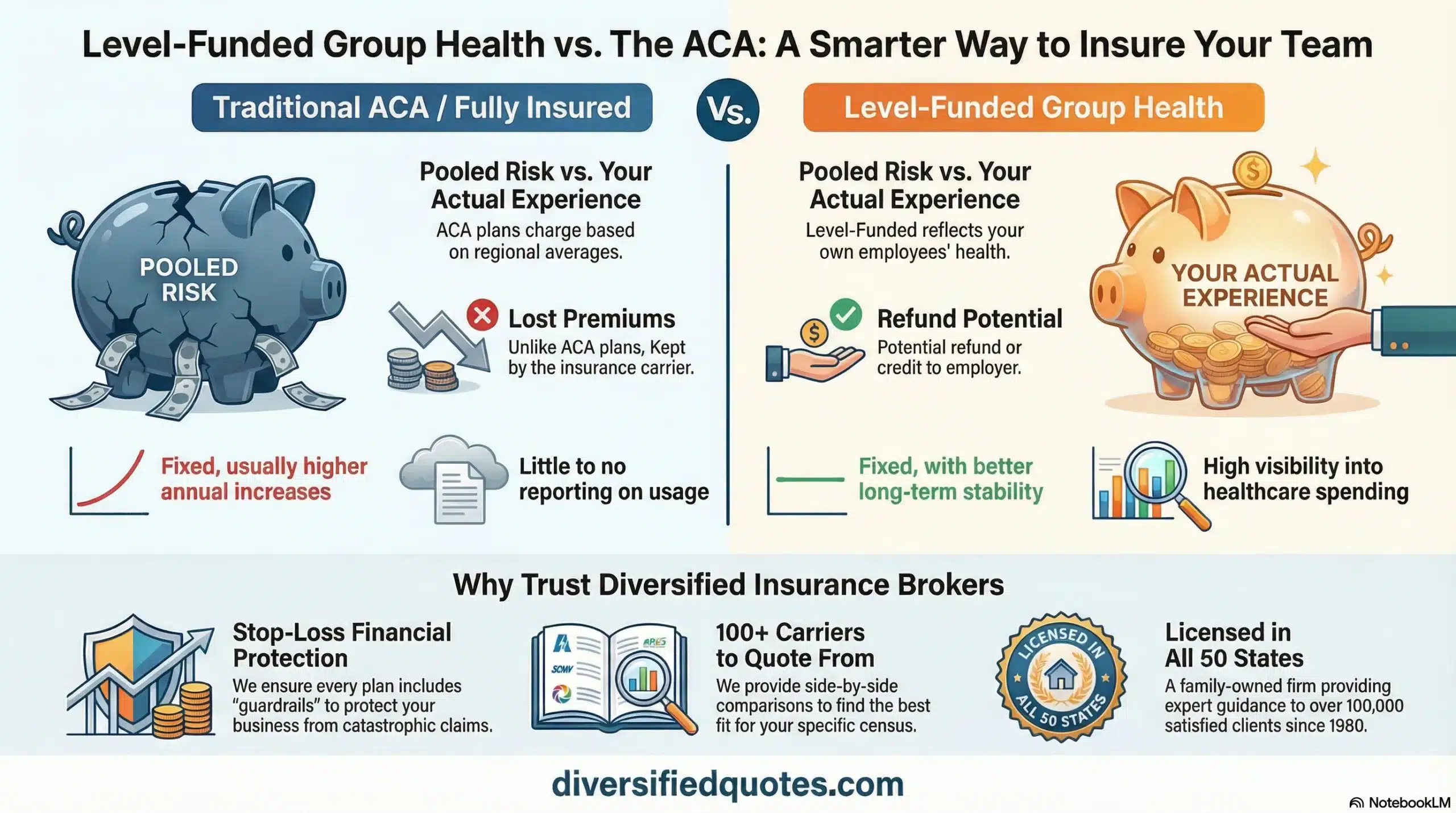
There are several primary group health structures to understand. Traditional fully insured plans shift claim risk to the carrier, with the employer paying a fixed premium. These are straightforward and predictable but subject to annual renewal increases. Level-funded and self-funded arrangements allow employers to retain some risk in exchange for potential cost savings and improved transparency. However, these structures require careful financial evaluation and may not be suitable for every company size. Small employers often begin with fully insured plans due to simplicity and lower administrative burden. As companies grow, more advanced funding structures may become viable.
Network type is another critical factor. PPO plans offer broader provider access and greater flexibility but usually come with higher premiums. HMO plans reduce costs but limit out-of-network coverage. EPO and POS structures sit somewhere in between. If your workforce includes employees with established specialists or out-of-state dependents, network design becomes even more important. Choosing a narrow network may reduce cost initially but increase dissatisfaction if employees cannot access preferred providers.
Deductibles, copays, and coinsurance structures shape how employees experience the plan. A low premium with a $7,000 deductible may look attractive on paper but feel unaffordable in practice. High-deductible health plans (HDHPs) paired with Health Savings Accounts (HSAs) can create tax-advantaged savings opportunities and empower employees to build medical reserves. For some companies, offering both a traditional PPO and an HSA-compatible option provides flexibility across income levels and health utilization patterns.
Need Help Comparing Group Health Plans?
We’ll analyze your workforce, compare multiple carriers, and design a cost-effective group health strategy tailored to your business.
Request a Group Health ConsultationEmployer contribution strategy plays a central role in both compliance and competitiveness. Many carriers require minimum employer contributions (often 50% of employee-only premium). Participation thresholds may also apply, particularly for small groups. Structuring contributions strategically can encourage enrollment while controlling employer liability. Some businesses offer tiered contribution models based on tenure or role. Others provide defined contribution allowances, allowing employees to choose between plan options.
Compliance considerations cannot be overlooked. Businesses with 50 or more full-time equivalent employees must comply with Affordable Care Act (ACA) employer mandate rules, including minimum essential coverage and affordability thresholds. COBRA administration, Section 125 cafeteria plans, ERISA documentation, and summary plan descriptions all require attention. Failure to comply can result in penalties. Working with an experienced advisor ensures documentation and reporting requirements are met.
Cost containment strategies should be proactive, not reactive. Renewal increases are common, but they are not always unavoidable. Reviewing claims data, evaluating alternative carriers, adjusting plan design, introducing wellness initiatives, and educating employees on cost transparency tools can all influence long-term trends. Transparency around pharmacy benefit management (PBM) contracts and specialty drug exposure is increasingly important as prescription costs rise.
Business owners should also consider integration with other employee benefits. Coordinating group health with Group vs. Individual Disability Insurance, voluntary life coverage through our Life Insurance Overview, and executive supplemental benefits can strengthen overall protection. A cohesive benefits strategy positions the company as stable and supportive — particularly important in competitive hiring markets.
For small businesses evaluating whether to offer coverage at all, the decision often comes down to long-term talent strategy. Even companies with fewer than 10 employees may benefit from offering group health, especially in professional industries where candidates expect it. Tax advantages may also offset part of the cost. Premium contributions are typically deductible business expenses, and certain small employers may qualify for tax credits under specific circumstances.
Large employers face different complexities. Multi-state operations must evaluate network access in each region. Remote workforces may require national PPO networks. Self-funded arrangements can provide transparency and potential savings but require stop-loss protection and cash-flow planning. Executive carve-out plans may also become part of broader compensation strategies.
Employee education plays a crucial role in maximizing plan value. Even a well-designed plan can feel inadequate if employees do not understand how to use it. Annual enrollment meetings, benefit summaries, comparison charts, and digital tools help reduce confusion and improve satisfaction. Encouraging preventive care utilization can also reduce long-term claims severity.
Planning for Renewal?
Don’t wait for your renewal increase to surprise you. Let us review your current plan and explore better alternatives.
Start Your Benefits ReviewAnother overlooked factor is leadership protection. Owners and executives often rely heavily on business income. Coordinating group health with disability income protection, such as Disability Insurance, ensures income continuity if a medical event interrupts operations. Comprehensive planning looks beyond medical claims and considers broader financial resilience.
As healthcare costs continue rising, companies that approach group health strategically — rather than reactively — maintain greater control. This includes evaluating wellness programs, telemedicine integration, mental health access, and cost-sharing structures. Culture matters. Employees who feel supported are more engaged and productive.
Ultimately, choosing the right group health plan is about balance: balancing cost and coverage, flexibility and predictability, compliance and simplicity, employee satisfaction and employer sustainability. There is no universal “best” plan — only the plan that best fits your workforce, budget, and growth trajectory. By evaluating funding structure, network design, cost-sharing levels, compliance requirements, and integration with other benefits, business owners can design a program that strengthens both financial performance and workplace culture.
Related Pages
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
A fully insured plan has fixed monthly premiums and shifts claim risk to the carrier. A self-funded (or level-funded) plan allows the employer to assume some claim risk in exchange for potential savings and greater transparency. The right structure depends on company size, cash flow stability, and risk tolerance. If you are unsure which structure fits, request a consultation through our Group Health Consultation Form.
Most carriers require employers to contribute at least 50% of the employee-only premium, though contribution strategies can vary. Structuring employer contributions carefully helps maintain compliance and encourage participation. Coordinating benefits with programs like Disability Insurance can also strengthen overall protection.
In most states, businesses with at least one eligible W-2 employee (other than the owner) can qualify for small group coverage. Participation and contribution requirements vary by carrier. Even small employers may benefit from offering coverage to remain competitive in hiring.
Yes, employer-paid premiums are generally tax-deductible as a business expense. Certain small businesses may also qualify for additional tax credits depending on size and wage levels. Consulting with a tax advisor is recommended to confirm eligibility.
Renewal increases can sometimes be mitigated by reviewing claims data, adjusting plan design, exploring alternative carriers, or considering level-funded arrangements. Regular benefit reviews and proactive planning are essential. You can also evaluate complementary protections such as Group vs. Individual Disability Insurance to strengthen your overall benefits strategy.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers, is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient.
