Guaranteed Issue Group Disability Insurance
Guaranteed Issue Group Disability Insurance

Jason Stolz CLTC, CRPC, DIA, CAA
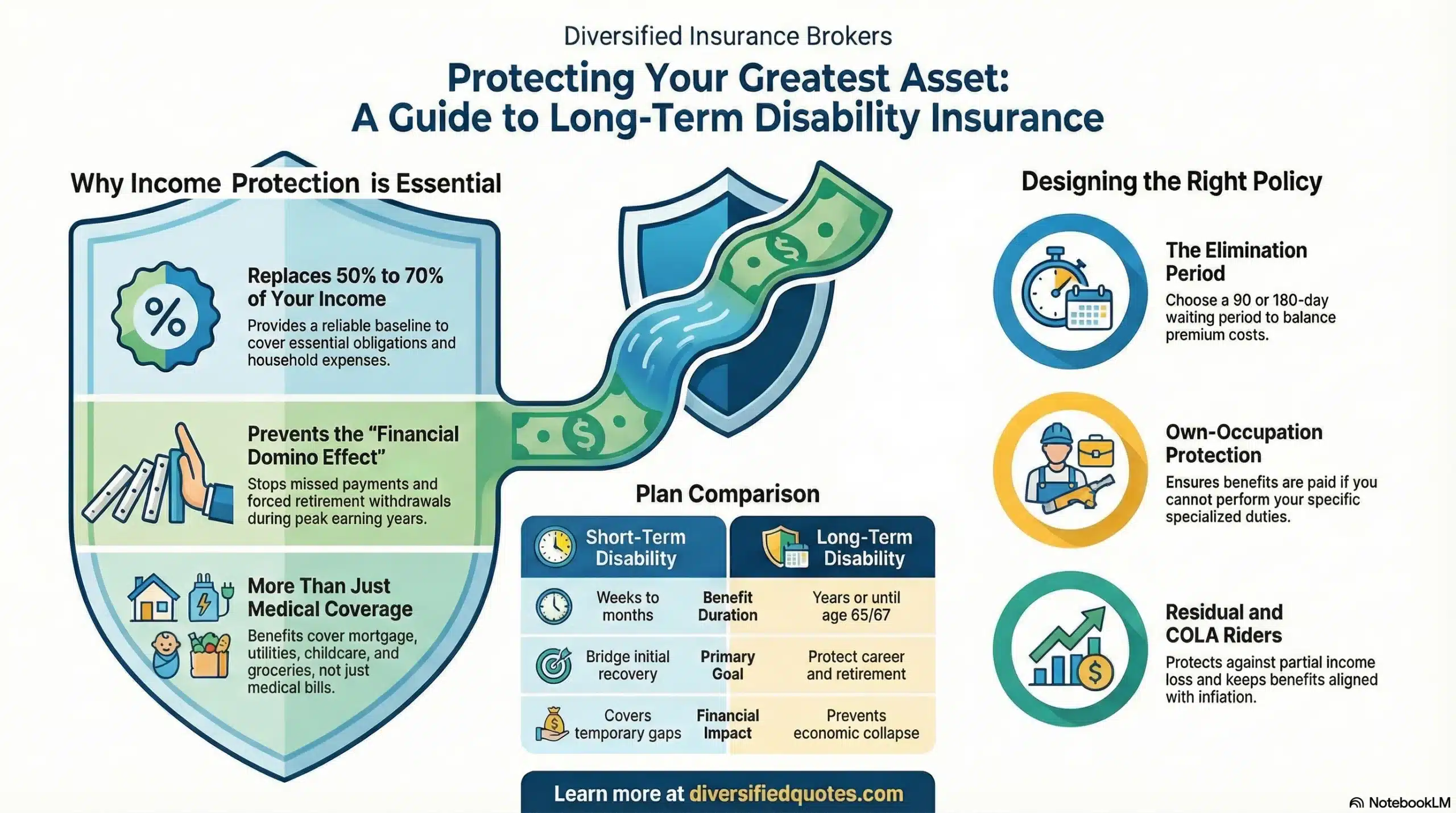
Guaranteed issue group disability insurance is the most accessible and fastest-to-implement form of employer-sponsored income protection available, allowing employers to offer meaningful disability coverage to their workforce without requiring each employee to go through individual medical underwriting. The “guaranteed issue” provision — which allows eligible employees to enroll for a defined benefit amount with no health questions or only minimal questions during an approved enrollment window — eliminates the most common participation barrier in disability insurance: the fear that a prior health history will prevent coverage or result in exclusions that render the policy useless. For employers who want to extend income protection broadly across the workforce rather than selectively to the healthiest employees, guaranteed issue group disability insurance is the structure that makes broad, equitable, and efficient enrollment possible.
The practical business case for guaranteed issue group disability insurance begins with a simple observation: disability risk is a payroll risk. When an employee becomes disabled and cannot work, the income disruption does not affect only the employee’s household — it affects team productivity, coverage obligations, morale, and retention as the organization absorbs the disruption and manages the workflow gap. A well-designed guaranteed issue group disability insurance plan provides the financial framework that allows disabled employees to focus on recovery rather than financial survival, which typically produces shorter claim durations, better recovery outcomes, and more successful returns to work. Employers who understand this connection treat group disability insurance not as a fringe benefit but as an investment in workforce stability. At Diversified Insurance Brokers, we help employers design guaranteed issue group disability insurance plans that are appropriately priced, participation-optimized, and built around the specific income distribution of the workforce rather than generic templates. Our resource on disability insurance services covers the full landscape of employer-sponsored and individual income protection, and our resource on why people buy disability insurance provides the risk context that makes guaranteed issue group disability insurance planning compelling for both employers and employees.
Compare guaranteed issue group disability insurance plans built for your industry, payroll, and workforce profile.
We’ll structure the benefit design, participation rules, and supplemental layers that make the plan work for your entire team.
What “Guaranteed Issue” Means in a Group Disability Context
Guaranteed issue in group disability insurance refers specifically to the underwriting approach used for employee enrollment, not to the contract’s claims provisions, definitions, or exclusions. Understanding this distinction is essential for setting accurate expectations about what guaranteed issue group disability insurance provides — and what it does not eliminate.
In traditional individual disability insurance underwriting, each applicant is evaluated independently based on their medical history, prescription records, attending physician statements, cognitive and functional assessments, and occupational risk profile. This thorough evaluation allows the carrier to price individual risk accurately, but it also creates barriers to coverage for employees with complex health histories, pre-existing conditions, or prior claims experience. The individual underwriting process can produce declines, benefit reductions, exclusion riders for specific body parts or conditions, and premium ratings that make coverage unaffordable for many employees who need it most.
Guaranteed issue group disability insurance shifts the underwriting from the individual level to the group level. Instead of evaluating each employee as a standalone risk, the carrier evaluates the group collectively — its size, industry, occupational composition, income distribution, and the plan design parameters — and agrees to insure eligible employees up to a defined guaranteed issue amount without requiring individual health evidence during the designated enrollment window. This collective risk assessment is what makes the guaranteed issue feature possible: the carrier is underwriting the group’s aggregate risk rather than each individual’s specific risk.
The guaranteed issue amount is not unlimited. Carriers set a maximum benefit level — often expressed as a monthly dollar amount — up to which enrollment is guaranteed for eligible employees during the enrollment window. Employees who need or want coverage above the guaranteed issue maximum may be required to provide evidence of insurability to access the additional coverage. The guaranteed issue threshold is one of the most important plan design decisions, because it determines how much of the workforce can enroll without medical scrutiny and where individual underwriting re-enters the picture for higher earners who need larger benefits.
Why Guaranteed Issue Group Disability Insurance Solves a Real Employer Problem
Employers who have tried to implement voluntary individual disability insurance programs without a guaranteed issue provision frequently encounter the same frustrating outcome: the employees who most need coverage — those with complex health histories, prior conditions, or higher-risk lifestyles — are precisely the ones who struggle to enroll, while the healthiest employees either obtain coverage easily or decline because they believe they do not need it. This adverse selection dynamic is not hypothetical; it is the natural result of voluntary enrollment without a guaranteed issue framework, and it produces a workforce protection gap that is both inequitable and inefficient.
Guaranteed issue group disability insurance resolves this adverse selection problem by making enrollment accessible to all eligible employees regardless of health history during the designated window. When the same enrollment opportunity is available to every eligible employee — not selectively to the healthy ones — the risk pool that forms the plan’s actuarial foundation is broader and more representative of the workforce, which is precisely the pool composition that supports competitive pricing and sustainable plan performance. Carriers can offer more favorable terms on a guaranteed issue basis for a well-composed group than they would offer on an individually underwritten basis for the same employees, because the group risk pooling mechanism distributes the potential impact of higher-risk individuals across the entire enrolled population.
From an equity and culture standpoint, guaranteed issue group disability insurance communicates something important about the employer’s benefit philosophy: income protection is a benefit extended to every eligible member of the workforce, not a privilege available only to those who happen to be in excellent health. This equitable access can be a meaningful differentiator in recruitment and retention conversations, particularly in industries where workforce demographics include a range of ages and health profiles and where the workforce values benefits that feel genuinely accessible rather than technically available but practically unattainable.
How Guaranteed Issue Group Disability Insurance Works: The Core Structure
The operational structure of a guaranteed issue group disability insurance plan involves several interconnected components that together determine how employees enroll, what coverage they receive, and how the plan functions during active claims. Understanding each component helps employers and plan advisors build programs that perform as expected and communicate clearly to employees.
| Plan Component | What It Determines | Typical Range | Planning Consideration |
|---|---|---|---|
| Guaranteed Issue Amount | Maximum benefit accessible without health evidence | Varies by carrier and group size | Should be benchmarked against workforce income distribution |
| Benefit Percentage | Portion of pre-disability income replaced | Usually 50%–70% of covered earnings | Higher percentages increase cost; 60% is common baseline |
| Elimination Period | Days of disability before benefits begin | Short-term: 0–14 days; Long-term: 60–180 days | Shorter periods cost more; should reflect PTO and savings profile |
| Benefit Period | Maximum duration of benefit payments | Short-term: weeks to months; Long-term: 2 years to age 65 | Longer periods provide stronger protection at higher premium |
| Definition of Disability | Standard for qualifying and staying on claim | Own-occupation, modified own-occ, any-occupation | Most important contract provision; drives claim experience |
| Pre-Existing Condition Limitation | Restriction on benefits for prior conditions during initial period | Commonly 3/12, 6/12, or 12/24 look-back/limit windows | Applies even in guaranteed issue; commonly misunderstood |
| Benefit Offsets | Income sources that reduce the plan benefit | SSDI, workers’ comp, other group DI | Integration limits total disability income; manages plan cost |
Each component in this table can be adjusted within the parameters established by the carrier and the plan’s overall design, and the combination of all components determines both the premium cost and the real-world protection experience for enrolled employees. Our resource on disability insurance elimination periods explained covers how the waiting period dimension specifically affects both cost and practical utility for employees at different savings levels.
Short-Term vs Long-Term Guaranteed Issue Group Disability Insurance
Guaranteed issue group disability insurance is available in both short-term and long-term structures, and the two serve fundamentally different phases of income protection need. Understanding how they differ — and how they can work together as a coordinated pair — is one of the most important concepts in employer-sponsored disability planning.
Short-term guaranteed issue group disability insurance is designed to address the immediate phase of an income interruption. Benefits typically begin after a short elimination period — ranging from zero days to 14 days depending on the plan design — and continue for a maximum benefit period of several weeks to a few months. Short-term disability coverage is the financial bridge between the onset of disability and either recovery or the activation of long-term disability benefits. It is particularly valuable for surgeries, acute injuries, childbirth complications, and medical events with relatively defined and predictable recovery trajectories. Our resource on how to buy short-term disability insurance covers the individual policy equivalent for employees who need coverage outside what an employer plan provides.
Long-term guaranteed issue group disability insurance addresses the extended phase of income interruption — cases where recovery takes months or years rather than weeks, or where a condition proves chronic or permanently limiting. The elimination period for long-term disability typically ranges from 60 to 180 days, which is why coordination with a short-term disability plan is so important: the short-term plan covers the period before long-term benefits activate. Long-term guaranteed issue group disability insurance is the product that provides meaningful protection against the most financially catastrophic disability scenarios — those where a person cannot return to their occupation for an extended period — and it is the coverage that most directly affects long-term household financial stability, retirement savings trajectory, and financial independence.
The most effective employer group disability programs coordinate short-term and long-term coverage like a relay: short-term benefits provide immediate income support at disability onset, and long-term benefits take over seamlessly when the short-term maximum benefit period expires. When the plans are designed with matched benefit periods and elimination periods that eliminate gaps, the employee experiences continuous income replacement rather than a coverage interruption between the two structures. Our resource on short-term versus long-term disability insurance covers this coordination strategy in detail.
Eligibility Rules and Enrollment Windows in Guaranteed Issue Group Disability Insurance
The guaranteed issue feature in a group disability plan is not permanently and unconditionally available — it is tied to specific eligibility criteria and enrollment windows that govern when employees can access coverage without individual health evidence. Understanding these timing and eligibility rules is critical for both employers designing the plan and employees making enrollment decisions.
Eligibility for guaranteed issue group disability insurance is typically based on employment classification — full-time employees meeting a minimum hours requirement (commonly 30 or more hours per week) and having completed a waiting period (commonly 30 to 90 days from date of hire). Employees who do not meet these thresholds during the plan’s enrollment window are not eligible for guaranteed issue enrollment and would need to apply with evidence of insurability if they later achieve eligibility.
The enrollment window is the defined period during which guaranteed issue enrollment is available without health evidence. The most important enrollment windows are: the initial plan enrollment when the group disability plan is first implemented, during which all currently eligible employees can enroll without evidence of insurability; the new employee enrollment window, during which newly hired employees can enroll when they first become eligible; and the annual or special open enrollment periods, which may provide some opportunity for employees who previously declined to enroll with evidence of insurability requirements.
Employees who decline coverage during their guaranteed issue enrollment window and later want to enroll typically must provide evidence of insurability — completing a full health questionnaire and potentially providing medical records — to access coverage. This late enrollment requirement is one of the most important reasons to communicate the guaranteed issue opportunity clearly at implementation: employees who understand that they can enroll now without health questions are more likely to enroll than employees who do not understand that declining and re-enrolling later will require underwriting.
Participation Requirements: Why They Matter for Guaranteed Issue Terms
One of the most consequential factors in the terms a carrier will offer for guaranteed issue group disability insurance is the plan’s participation rate — the percentage of eligible employees who enroll. Carriers underwriting group disability plans are managing a risk pool, and a key variable in that pool’s actuarial performance is how broadly representative the enrolled population is of the full eligible workforce.
When participation is high — typically above 60% to 75% of eligible employees — the risk pool is broad enough that individual health variations are diversified across many participants, and the carrier can offer favorable guaranteed issue terms: higher guaranteed issue amounts, more protective disability definitions, and competitive premiums. When participation is low, the risk pool skews toward adverse selection — the participants who enrolled despite lower participation rates may disproportionately represent higher-risk individuals who had stronger motivation to secure coverage — and the carrier’s guaranteed issue terms become more restrictive in response.
This participation dynamic is one of the strongest actuarial arguments for employer-paid or employer-contributory guaranteed issue group disability insurance plans rather than fully voluntary plans. When the employer pays the full premium, participation is typically 100% (or close to it) because all eligible employees are automatically enrolled. This maximum participation produces the most favorable guaranteed issue terms from the carrier’s perspective and often results in better premium pricing per participant than a voluntary plan with incomplete participation. When the employer contributes toward the premium but does not pay the full cost, participation is typically higher than a purely voluntary plan but lower than a fully employer-paid plan, and the guaranteed issue terms reflect the intermediate participation level.
The Definition of Disability: The Most Important Contractual Provision
The definition of disability in a guaranteed issue group disability insurance policy determines more than any other provision whether a specific employee’s real-world situation will produce a benefit payment when a claim is filed. Guaranteed issue enrollment eliminates the underwriting barrier at the front end, but it does not change how the policy evaluates claims at the back end — and the disability definition is the standard against which every claim is measured.
The most protective definition available in disability insurance is own-occupation, which requires only that the claimant be unable to perform the material duties of their own specific occupation. Under an own-occupation definition, a nurse whose back injury prevents the physical demands of patient care — lifting, repositioning, extended standing — may qualify for benefits even if she could theoretically perform a clerical job, because her disability prevents her from performing her own occupation. A surgeon whose hand tremor prevents surgical practice qualifies under own-occupation disability even if he could teach or consult, because he cannot perform the duties of his own surgical specialty. Our resource on own-occupation disability insurance covers how this definition specifically protects specialized professional income.
Many group long-term disability plans use a modified approach: an own-occupation definition during the first 24 months of disability, transitioning to an any-occupation definition thereafter. Under the any-occupation standard applied after the 24-month transition, the claimant must demonstrate that they cannot perform any occupation for which they are reasonably suited by education, training, and experience — a significantly harder standard to meet. This definition transition is one of the most important features for employers and employees to understand before plan enrollment, because it determines how the plan treats longer-term disability situations where the employee cannot return to their specific occupation but might be able to work in a different capacity.
Partial or residual disability provisions add another dimension to the definition structure. Plans that include a residual disability benefit pay a proportionate benefit when a claimant returns to work with reduced capacity — working part-time or performing only some occupational duties due to medical restrictions — rather than terminating benefits abruptly when any level of return to work begins. Residual provisions create an important incentive structure: employees can attempt a graduated return to work without risking a complete loss of benefits if they cannot yet perform at full capacity. This flexibility typically produces better claim outcomes for both the employee and the employer by supporting partial recovery rather than creating financial pressure to either remain fully disabled or return fully before recovery warrants it.
Pre-Existing Condition Limitations: What Guaranteed Issue Does Not Eliminate
The most common misconception about guaranteed issue group disability insurance is that guaranteed issue enrollment means guaranteed claim payment for any disability, including those arising from pre-existing conditions. Guaranteed issue refers to enrollment eligibility — the ability to enroll without health evidence — not to unlimited claim liability. The plan’s pre-existing condition limitation (PECL) is a separate contractual provision that governs how claims are handled for conditions that were treated or diagnosed before coverage became effective.
A typical pre-existing condition limitation in a guaranteed issue group disability insurance policy uses a “look-back and limitation” formula expressed in abbreviated form such as 3/12, 6/12, or 12/24. The first number represents the look-back period — the number of months before the coverage effective date during which treatment, consultation, prescription, or medical advice related to a condition is evaluated. The second number represents the limitation period — the number of months after the coverage effective date during which disabilities arising from conditions that were treated during the look-back period may not be payable (or may be payable only under specific circumstances).
Under a 3/12 pre-existing condition limitation: if an employee received treatment for a back condition in the 3 months before the coverage effective date, and if a disability arises from that back condition within the 12 months following the effective date, the claim may be denied or limited under the PECL. After the 12-month limitation period expires, the PECL no longer applies to that condition — future claims arising from the same condition after the limitation period are evaluated on their merits without the PECL restriction.
For employees who are enrolling in guaranteed issue group disability insurance with ongoing health conditions, this pre-existing condition limitation timeline is an important planning consideration. Employees with stable chronic conditions who are not currently disabled should still enroll during the guaranteed issue window — even if their condition is subject to the PECL — because the limitation period is finite, and coverage after the PECL expires is both guaranteed and fully effective.
Benefit Offsets and Coordination With Other Income Sources
Group long-term disability policies routinely include benefit offset provisions that coordinate the plan’s monthly benefit with other disability-related income the claimant receives from outside sources. These offsets are a standard actuarial tool for managing plan costs while ensuring that the total disability income from all sources remains below a reasonable ceiling relative to pre-disability earnings — typically in the 70% to 80% range of covered compensation.
The most common offset sources in guaranteed issue group disability insurance include Social Security Disability Insurance (SSDI) benefits, workers’ compensation payments for disabilities that are occupationally caused, state disability plan benefits in states with mandated programs, and benefits from other group disability policies. When SSDI benefits are awarded to a long-term disability claimant, the LTD plan typically reduces its monthly benefit by the SSDI amount — so the total income from both sources equals the LTD plan’s original benefit amount rather than stacking on top of it.
The offset mechanics have a practical implication for plan cost: carriers can offer competitive premiums on group long-term disability plans partly because the offset provisions limit the carrier’s maximum liability when claimants successfully obtain benefits from other offset sources. For employees, the offset provisions mean that successfully obtaining SSDI benefits during a long-term disability claim does not increase total disability income — it transfers a portion of the income obligation from the group carrier to the Social Security system, which is one reason why carriers often encourage or assist claimants in applying for SSDI.
The High-Earner Gap in Guaranteed Issue Group Disability Insurance
The most structurally significant limitation in standard guaranteed issue group disability insurance plans is the income replacement gap that affects higher-earning employees when the plan’s maximum monthly benefit cap produces an effective replacement rate meaningfully below the plan’s stated percentage. This gap is not a design flaw — it reflects the actuarial and financial reality that unlimited benefit amounts in a guaranteed issue structure would create unsustainable carrier risk — but it is a planning gap that employers with higher-income workforces must address proactively.
Consider a group long-term disability plan that replaces 60% of pre-disability monthly earnings with a maximum monthly benefit of $10,000. For an employee earning $120,000 annually — $10,000 per month — the plan replaces 60% of income at exactly the maximum ($6,000 per month). For an employee earning $200,000 annually — $16,667 per month — the plan’s 60% formula would produce $10,000 per month, which represents only 60% of monthly earnings… but the cap means the benefit is actually $10,000 regardless, which is 60% of $16,667. In this case, the cap coincidentally is exactly 60%. But for a higher earner at $300,000 annually — $25,000 per month — the 60% formula would produce $15,000, but the plan caps at $10,000, making the effective replacement rate only 40% of their monthly income rather than the plan’s stated 60%. This gap widens as income increases above the cap threshold.
Our resource on high-income disability insurance covers the supplemental strategies specifically designed to fill this gap for executives, owners, and high-producing employees. The most common approach is to add a supplemental individual disability policy — underwritten at the individual level for the higher earner — that covers the gap between the group plan’s maximum benefit and the income protection target for the specific individual. Our resources on disability insurance for dentists, disability insurance for doctors and physicians, and disability insurance for physicians cover occupation-specific high-income supplemental strategies in depth.
Key Person and Business Continuity Disability Planning
For closely held businesses and professional practices, guaranteed issue group disability insurance for the employee workforce is often complemented by separate disability insurance structures designed to protect the business itself rather than just the individual employee-owner’s income. These business-focused disability products address scenarios that the standard group disability plan — even a well-designed one — is not intended to cover.
Key person disability insurance protects the business against the financial loss of a specific producer, rainmaker, or irreplaceable operational contributor. When a key person becomes disabled, the business may experience revenue loss, client relationship disruption, productivity decline, and recruitment costs to source a replacement — none of which the disabled key person’s individual income replacement benefit addresses. Key person disability insurance pays the benefit to the business rather than to the disabled individual, providing capital to manage the operational and financial disruption. Our resource on key person disability insurance covers the specific design and underwriting considerations for business-level disability protection.
Buy-sell disability insurance addresses the ownership transition risk that arises when a business owner or partner becomes disabled. In a multi-owner business without a funded disability buy-sell arrangement, a partner’s disability can create an ownership crisis: the disabled partner needs income and may want to exit, but the remaining partners may not have capital available to buy out the disabled partner’s interest without business disruption. Disability buy-sell insurance provides the funding mechanism — paying a benefit that enables the remaining owners to purchase the disabled owner’s interest under the terms of a pre-agreed buy-sell agreement. Our resource on buy-sell disability insurance covers the funding and design mechanics for this critical business continuity tool.
Cost Structure and Employer Funding Models for Group Disability Insurance
The funding model for a guaranteed issue group disability insurance plan — who pays the premium, how much each party contributes, and how premium costs affect the tax treatment of benefits — has meaningful implications for both the plan’s participation profile and the after-tax value of benefits to employees who make claims.
When the employer pays 100% of the premium for a group long-term disability plan, several consequences follow. Participation is typically highest because enrollment is automatic or essentially frictionless for employees. Premium tax treatment for the employer is generally favorable — group disability premiums are typically deductible as an ordinary business expense. However, when the employer pays 100% of the premium, benefit payments received by disabled employees are generally taxable as ordinary income to the employee — because the premium payments that funded the coverage were not included in the employee’s taxable income.
When the employee pays 100% of the premium — a fully voluntary arrangement — benefit payments received during a disability are generally tax-free to the employee because they funded the coverage with after-tax dollars. This tax-free benefit treatment can meaningfully increase the effective value of the benefit to the claimant. The trade-off is that fully voluntary plans typically require evidence of insurability unless structured with specific guaranteed issue provisions, and participation is lower than employer-paid plans — which can affect both guaranteed issue terms and premium pricing.
Many employers use a cost-sharing model — contributing a defined portion of the premium and requiring employees to pay the remaining portion — that balances the tax treatment considerations, participation goals, and budget constraints. The specific split depends on the employer’s compensation strategy, benefits philosophy, and the income levels of the workforce the plan is designed to serve.
What Actually Happens When an Employee Files a Disability Claim
The claim process in a guaranteed issue group disability insurance plan follows a defined sequence that the employer and employee should understand before a claim is needed, not after. Unexpected confusion about claim procedures during an already stressful disability event creates unnecessary delays and frustration that a well-communicated plan design can prevent.
The claim process typically begins with notification — the disabled employee or their representative contacts the group carrier or its designated third-party administrator to report the disability and initiate the claim. The carrier provides the required claim forms, which typically include an employee statement, an attending physician’s statement, and an employer statement confirming the claimant’s pre-disability earnings and employment status. The attending physician’s statement is often the most time-sensitive document because it requires the treating physician’s time and attention at a moment when clinical care is the priority — which is one reason why carriers typically allow several weeks for claim form submission after the initial notification.
The carrier’s claims team reviews all submitted documentation against the plan’s disability definition, pre-existing condition limitations, and eligibility requirements to make an initial claim decision. For straightforward claims with clear medical documentation and an unambiguous disability definition, decisions may come within a few weeks. For complex medical presentations or cases where the disability definition requires more nuanced evaluation of functional limitations versus occupational demands, the review process may take longer and may involve independent medical examinations or consultation with vocational experts.
During an approved long-term disability claim, ongoing case management is a significant feature of most group LTD plans. Carriers assign case managers who monitor the claimant’s progress, coordinate return-to-work planning, facilitate appropriate medical care, and manage the claim duration. Proactive case management that supports gradual return to work — including residual disability provisions that allow partial benefits during a phased return — typically produces better outcomes for claimants and lower long-run claim costs for the plan.
Related Disability Insurance Planning Pages
Explore disability income resources for employers, owners, high earners, and specialized occupations.
Financial Protection Essentials
Coordinate group disability planning with group health, high-risk life insurance, and long-term care resources.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
Frequently Asked Questions: Guaranteed Issue Group Disability Insurance
What does “guaranteed issue” mean in a group disability insurance plan?
Guaranteed issue in group disability insurance refers specifically to the enrollment underwriting approach: eligible employees can enroll for a defined maximum benefit amount without completing individual medical underwriting — no health questionnaire, no medical exam, no physician records review — during an approved enrollment window. The carrier accepts the employee’s enrollment based on the group’s collective risk profile rather than evaluating the individual’s specific health history. Guaranteed issue applies to the enrollment process only — the policy’s claims provisions, disability definition, pre-existing condition limitations, and other contract terms still apply after coverage is in force.
Does guaranteed issue mean there are no exclusions or pre-existing condition limitations?
No. Guaranteed issue refers to enrollment eligibility, not unlimited claim payment. Most guaranteed issue group disability insurance policies include a pre-existing condition limitation that restricts benefits for disabilities arising from conditions that were treated during a look-back period before the coverage effective date, typically for an initial period after the coverage begins. Common PECL formulas use notation like 3/12 or 12/24, where the first number is the pre-coverage look-back window in months and the second is the post-effective-date limitation period in months. After the limitation period expires, the PECL no longer applies to that condition and future claims are evaluated without it.
Why do participation rates affect guaranteed issue terms?
Carriers underwriting group disability plans manage a risk pool, and the composition of that pool is directly affected by who enrolls. When participation is high — most eligible employees enroll — the risk pool is broadly representative and the carrier can offer favorable guaranteed issue terms: higher benefit amounts without medical evidence, more protective disability definitions, and competitive premiums. When participation is low, the pool skews toward adverse selection (higher-risk individuals with stronger motivation to enroll) and the carrier’s terms become more restrictive. Higher participation, typically achieved through employer-paid or employer-contributory plans rather than purely voluntary structures, produces the most favorable guaranteed issue terms and premium pricing.
How does guaranteed issue group disability insurance handle high-earning employees?
Most guaranteed issue group disability insurance plans have a maximum monthly benefit cap. As employee income rises above the threshold where the benefit percentage times the monthly income would exceed the cap, the effective income replacement rate declines. For example, a plan replacing 60% of income with a $10,000 monthly cap effectively replaces only 40% of income for an employee earning $25,000 per month. This high-earner gap is addressed through supplemental individual disability insurance that fills the difference between the group plan’s maximum and the income protection target — underwritten individually for each higher-earning employee and layered over the group foundation. Our resource on high-income disability insurance covers supplemental strategies in detail.
What is the difference between short-term and long-term group disability insurance?
Short-term group disability insurance covers the immediate phase of income interruption — typically beginning within days of disability onset and paying benefits for several weeks to a few months. Long-term group disability insurance covers extended disabilities, typically activating after a 60-to-180-day elimination period and paying benefits for periods ranging from a defined number of years to the claimant’s age 65 or Social Security normal retirement age. The two products work most effectively as a coordinated pair: short-term benefits bridge the period from disability onset through the long-term plan’s elimination period, and long-term benefits take over for extended cases. Our resource on short-term versus long-term disability insurance covers the coordination strategy in detail.
Can business owners and partners be included in a guaranteed issue group disability plan?
In many cases, yes, depending on the business structure, how the owner is compensated, and the specific carrier’s eligibility guidelines. S corporation shareholders-employees, for example, may be eligible for group disability plans based on their W-2 compensation, while partnership draws or sole proprietor income may require different plan structures. Beyond personal income replacement, business owners with ownership interests often need additional disability coverage structures — key person disability insurance and disability buy-sell insurance — that address the business-level financial consequences of the owner’s disability rather than just the personal income replacement need. Our resources on key person disability insurance and buy-sell disability insurance cover these business continuity structures.
Are benefits from employer-paid group disability plans taxable to the employee?
Generally yes. When an employer pays 100% of the group disability insurance premium, benefit payments received by disabled employees are typically taxable as ordinary income to the employee — because the premiums were paid with pre-tax employer dollars and were deducted as a business expense, the benefits received are treated as taxable compensation. When employees pay 100% of the premium with after-tax dollars (fully voluntary arrangement), the benefits they receive are generally tax-free. Cost-sharing arrangements produce proportionate tax treatment: the portion of the benefit attributable to employer-paid premium is taxable, and the portion attributable to employee-paid premium is tax-free. Tax treatment has a direct effect on the after-tax value of disability benefits and is an important consideration in plan design and cost-sharing decisions.
About the Author:
Jason Stolz, CLTC, CRPC, DIA, CAA and Chief Underwriter at Diversified Insurance Brokers (NPN 20471358), is a senior insurance and retirement professional with more than 25 years of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, Group Health, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient. Visitors who want to explore current annuity rates and compare options across multiple insurers can also use this annuity quote and comparison tool.
Explore More Disability Insurance Options: Browse our complete guide to Disability Insurance for Physicians — covering own occupation, no exam, riders, elimination periods & coverage details from 100+ carriers.
