Group Medical Insurance

Jason Stolz CLTC, CRPC
Group medical insurance is one of the most important employee benefits decisions a business can make because it touches recruiting, retention, payroll strategy, and long-term cost control all at once. Whether you run a two-person company, a small employer with 10–50 employees, or a growing organization with multiple locations, the right group medical plan can deliver broad access to care while helping you stabilize healthcare spending over time.
At Diversified Insurance Brokers, we help employers compare plan types, funding structures, networks, and contribution approaches so the end result is practical—not theoretical. The goal is simple: a plan your employees will actually use, a renewal process that isn’t a surprise every year, and a cost structure that fits the way your business runs.
If you want more detail on adjacent topics, our guides on small employer group health insurance and what is self-funded group health insurance are useful companion pages.
Compare Group Medical Insurance Options
Tell us your employee count, state, and goals. We’ll outline practical plan options and the tradeoffs that matter.
How Group Medical Insurance Works
Group medical insurance allows an employer to offer health coverage to eligible employees under a coordinated plan structure. Instead of each person shopping independently for their own policy, the employer establishes a group plan with defined eligibility rules, contribution strategy, and enrollment windows. Premiums are typically shared between employer and employee, and in many cases the group structure can produce better pricing and access than individual shopping—especially when the employer contributes meaningfully and participation is strong.
Operationally, group medical coverage is a system: employees enroll during open enrollment (or when newly eligible), premiums are handled through payroll deductions, and the plan is renewed on a yearly cycle. The “shape” of the plan—network, deductibles, copays, and out-of-pocket limits—determines how employees experience the coverage day to day.
There are three major ways the money side can be structured. A traditional fully insured plan uses a set premium where the carrier assumes the claims risk. A level-funded plan blends fixed monthly payments with a claims-based accounting structure. A self-funded plan means the employer pays claims as they occur while using stop-loss insurance to cap catastrophic exposure. Each structure can work well in the right scenario, and each has tradeoffs that should be evaluated in context.
Why Employers Use Group Medical Insurance
For most employers, group medical insurance is both a benefits decision and a business decision. It helps you compete for talent, reduce unwanted turnover, and create stability in compensation planning. Health benefits are one of the first items candidates evaluate—especially for experienced hires and employees with families—and the presence (or absence) of a credible plan can change who is willing to join your team.
Group medical insurance also supports productivity. When employees have access to routine and preventive care, they are more likely to address issues early instead of waiting until a problem becomes an emergency that turns into time off work. Over time, a plan that employees understand and use appropriately tends to reduce “avoidable waste” such as unnecessary ER utilization and high-cost out-of-network patterns.
Finally, group medical insurance is a tool for financial predictability. Even if healthcare costs rise nationally, employers that structure their plans intentionally—matching funding model, plan design, and contribution strategy—typically experience fewer surprises than employers who simply renew a generic plan every year without review.
Who Qualifies for Group Medical Coverage?
Most states and carriers require a legitimate business entity and a minimum number of eligible participants. In many cases, eligibility starts at two enrolled employees or owners, though the exact rules vary by state, carrier, and plan type. If you’re unsure what applies to your business, this guide on minimum employees for group health insurance is the best baseline.
Eligibility is not only about headcount. Carriers often look for proof of an active business operation, and they typically define eligible employees based on consistent weekly hours. Many plans define full-time eligibility around a 20–30 hour threshold, though definitions vary. Employers also typically need to meet minimum contribution expectations (often tied to employee-only premiums) and participation expectations (often tied to the percentage of eligible employees who enroll, with valid waivers allowed for employees who have other coverage).
For very small businesses, it’s also important to understand “who counts” for eligibility. Owner-only setups, spouse employees, and related individuals can be treated differently depending on state rules and carrier underwriting guidelines. The cleanest approach is to structure the plan so eligibility is clear, defensible, and easy to administer year after year.
Plan Types: PPO, HMO, HDHP/HSA, and More
Once eligibility is clear, the next decision is plan type—meaning how the network works and how employees pay for care. Most employers choose from PPO, HMO, and high-deductible plan designs (often paired with an HSA). Each can work, but each creates a different employee experience.
PPO plans are popular because they often provide broader provider access and allow employees to see specialists without strict referral requirements. In many markets, PPO designs are easiest for employees to understand because the network is straightforward and provider choice is wider. The tradeoff is typically premium cost, especially if the network is strong and the plan is richer.
HMO plans can be more cost-effective in the right region and when employees are concentrated in the same service area. Many HMOs emphasize coordinated care through a primary care provider and require referrals to specialists. When the provider ecosystem is strong, employees can have a good experience; when access is limited, HMO restrictions can become frustrating.
HDHP/HSA plans are often used when employers want to reduce premium costs while still offering meaningful coverage. The key is that an HDHP is not “cheap insurance.” It’s a different structure where employees pay more out of pocket up front, but the plan is compatible with an HSA that can be funded by employee and/or employer contributions. When implemented intentionally, an HSA strategy can improve cost predictability for the employer and create a tax-advantaged savings tool for employees.
Many employers choose a two-option approach: a value-focused plan (often HDHP/HSA) and a buy-up plan (often PPO) so employees can choose based on their preferences. This can reduce employer costs without removing choice—especially when contribution strategy is built correctly.
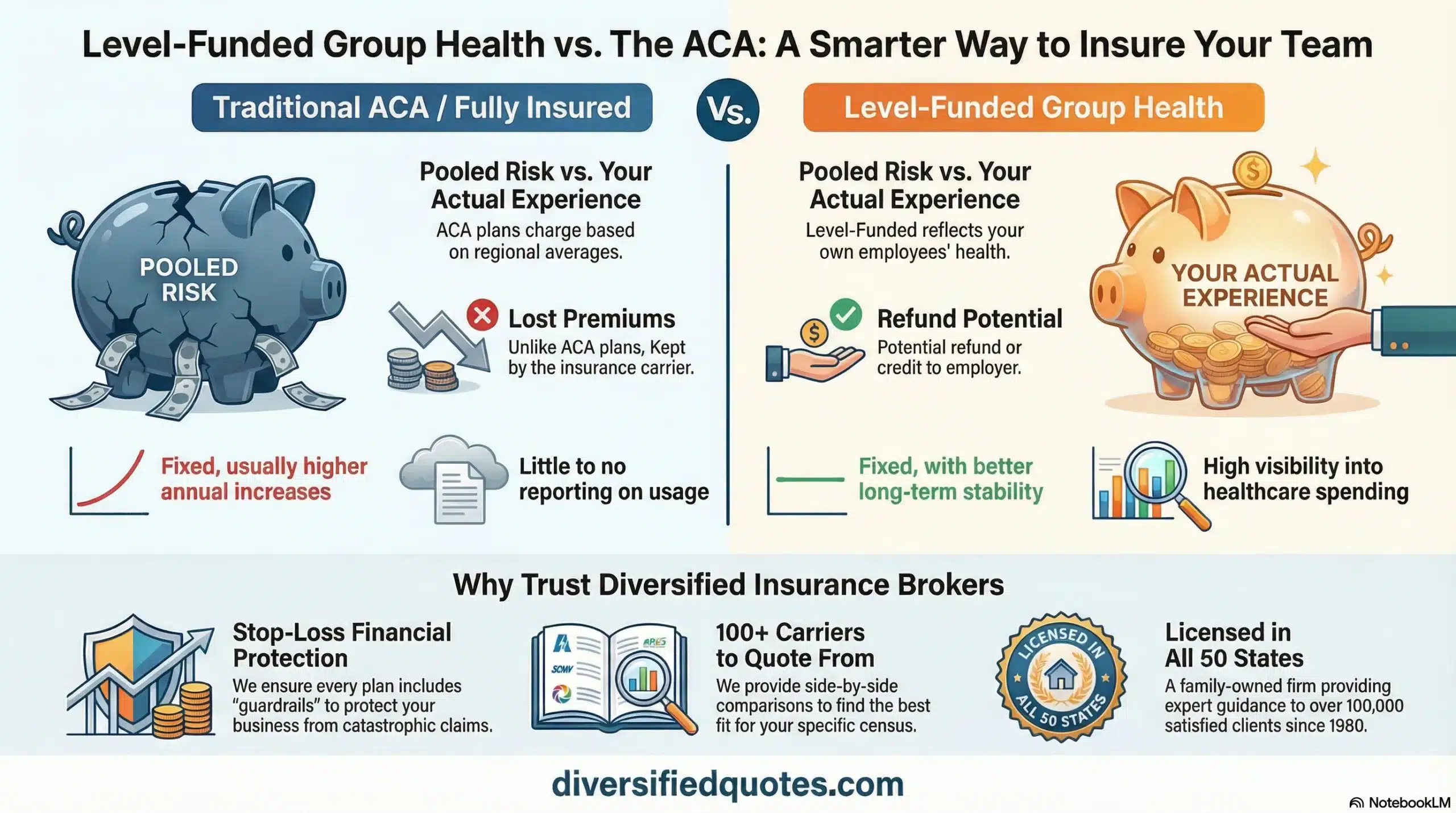
Funding Models: Fully Insured vs Level-Funded vs Self-Funded
Plan type determines the employee experience. Funding model determines how costs behave over time and what levers the employer has to manage renewals. Many employers start fully insured because it’s familiar, then evaluate level-funded or self-funded models as they grow and want more transparency.
Fully insured means you pay a set premium and the carrier assumes claims risk for the plan year. The advantages are simplicity and stable monthly premiums. The downside is that transparency into what’s driving cost is limited, and renewals may include carrier margins, trend assumptions, and risk buffers that don’t perfectly match your group’s performance.
Level-funded is designed to feel like fully insured from a cash-flow perspective (predictable monthly payment), but it’s typically built on a claims-based structure with stop-loss protection. When claims are favorable, some level-funded arrangements may return unused claim funds or provide renewal credits. It can be a strong “bridge” structure for employers that want predictability but also want a pathway to better pricing mechanics.
Self-funded means the employer pays claims as they occur, while stop-loss insurance caps catastrophic exposure. The biggest advantage is visibility and control: employers can see claims drivers, analyze pharmacy trends, and make plan adjustments with real data. The biggest requirement is discipline: the plan must be structured with appropriate stop-loss, credible administration, and a clear approach to budgeting and governance. If you want a deeper dive into this approach, your existing link to what is self-funded group health insurance is the right supporting page.
As a practical rule, the “best” funding model is the one that matches your risk tolerance, cash-flow reality, and administrative capacity. The point isn’t to chase complexity—it’s to choose a structure that makes renewals more manageable and costs more explainable.
Want a Side-by-Side Comparison Built for Your Business?
We’ll compare networks, plan designs, and funding models with clear “best case / expected / stress case” cost outcomes.
Cost Control Strategies That Don’t Break Recruiting
Most employers make the same mistake: they try to reduce costs by squeezing benefits. That approach often backfires because it increases employee dissatisfaction, reduces participation, and can lead to a higher-risk enrolling population—making the plan more expensive over time. Sustainable cost control is usually structural, not punitive.
Start with the network. A plan that looks cheaper but forces out-of-network usage can create higher claims and more employee frustration. A high-quality network can reduce waste and improve satisfaction even if premiums are slightly higher on paper.
Use plan tiering intelligently. Offering a value plan and a buy-up plan allows employees to self-select. The value plan can reduce employer costs, while the buy-up plan provides a premium option for employees who want richer benefits.
Align deductibles and copays with real utilization. Many groups end up with plan designs that don’t match employee behavior. When the plan is built around predictable usage patterns—primary care, urgent care, prescriptions—waste tends to drop and employee satisfaction improves.
Educate employees briefly and consistently. Clear education around urgent care vs ER, how prescriptions work, and how to stay in-network can reduce claims waste. This is especially important in smaller employers where a few avoidable high-cost events can impact renewals.
Review the plan early. The biggest lever in group benefits is timing. Employers that start renewal review early can compare options calmly and avoid rushed “take it or leave it” decisions.
Tax Advantages and Payroll Strategy
Group medical insurance isn’t only a benefits tool—it can also be an effective payroll strategy when structured correctly. In many cases, employer premium contributions are treated as a business expense, and employee premium shares can often be handled through pre-tax payroll mechanisms depending on plan setup and payroll configuration. This can improve take-home value for employees without requiring the employer to simply “pay more.”
HDHP/HSA strategies can also introduce additional tax advantages for employees who want to save for healthcare expenses in a dedicated, tax-advantaged account. When an employer contributes to HSAs as part of the benefits package, it can function like a targeted compensation tool that supports retention while preserving cost predictability.
For many employers, the key is to coordinate the plan with payroll operations so contributions, deductions, and eligibility are administered consistently. The better the administration, the fewer disruptions employees experience—and the less time leadership spends resolving avoidable benefits issues.
Renewals: Why Rates Change and How to Reduce Surprises
Renewals are where group medical insurance either becomes stable or becomes a yearly emergency. Rates move for a few common reasons: overall healthcare inflation, changes in the group’s claims experience, shifts in participation, network performance, and carrier underwriting changes. Employers who don’t see the “why” behind the renewal often feel like they have no control, when in reality the plan structure and strategy can make renewals far more manageable.
One of the most effective approaches is to build a repeatable renewal calendar. Start early, gather clean enrollment and eligibility data, review plan performance, and then compare alternatives. Even if you stay with the same carrier, the act of benchmarking helps keep pricing honest and prevents complacency. Over time, this process can reduce volatility and help you keep benefits consistent—something employees value highly.
If your organization is growing, it’s also important to revisit whether the original funding model still fits. Many employers outgrow their initial plan structure and simply don’t realize it until renewals become painful. A structured review is usually enough to identify whether you should stay insured, evaluate level funding, or explore a self-funded approach.
Implementation Checklist
A successful group medical rollout does not require a large HR department, but it does require a clear process. Start by confirming eligibility rules (full-time definition, waiting period, owner eligibility), then select plan options and contribution strategy. Next, prepare simple employee communication: what the plan is, what it costs, how to enroll, and how the network works.
Enrollment should be run on a clean timeline with a clear point of contact. After enrollment, do a short “first 30–60 days” check to confirm ID cards, payroll deductions, and network access are working smoothly. Administrative problems are one of the fastest ways to damage employee confidence in a benefits plan, even when coverage is strong.
Fully Insured vs Level-Funded vs Self-Funded
| Feature | Fully Insured | Level-Funded | Self-Funded |
|---|---|---|---|
| Monthly cost behavior | Fixed premium | Fixed payment with claims accounting | Variable based on claims timing |
| Risk positioning | Carrier holds claims risk | Shared risk with stop-loss | Employer pays claims with stop-loss protection |
| Transparency | Limited (varies by carrier) | Improved visibility vs fully insured | Highest visibility into claims drivers |
| Best fit | Employers prioritizing simplicity | Employers wanting predictability + upside | Employers wanting control + data-driven management |
Find the Right Group Medical Plan
We’ll help you balance cost, compliance, and employee experience with a plan structure that fits your business.
Financial Protection Essentials
Carrier reviews, retirement income planning tools, and specialized coverage resources for individuals and businesses.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
FAQs: Group Medical Insurance
What is group medical insurance?
Group medical insurance is an employer-sponsored health plan that covers multiple employees under a single policy, offering lower premiums and broader benefits compared to individual plans.
Who qualifies for group medical insurance?
Most states require at least two eligible full-time employees or owners. Married couples usually count as one entity, so two unrelated participants are typically needed.
Can small businesses with only two people qualify?
Yes, two-person businesses can often qualify for group health coverage if both are active employees and not married to each other. Learn more in our guide to 2-person group health insurance.
Are group medical insurance premiums tax-deductible?
Yes. Employer contributions to group premiums are tax-deductible, and employee contributions can be made pre-tax under Section 125 plans.
What types of group medical plans are available?
Employers can choose from fully insured, level-funded, or self-funded plans, each offering different cost structures and risk profiles.
Can I change carriers mid-year?
Yes. Group medical insurance can typically be adjusted at renewal or during a qualifying event. Employers may switch carriers to improve pricing or coverage quality.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers (NPN 20471358), is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, Group Health, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient. Visitors who want to explore current annuity rates and compare options across multiple insurers can also use this annuity quote and comparison tool.
