ER & Urgent Care: When Hospital Indemnity Pays

Jason Stolz CLTC, CRPC
Cash Benefits for ER & Urgent Care Bills
Add a hospital indemnity ER benefit so short, unexpected visits don’t become big out-of-pocket surprises.
ER and urgent care visits are among the most common “small events” that can turn into big out-of-pocket costs. One visit can produce a copay, coinsurance, a facility charge, imaging charges, physician charges, and sometimes follow-up services—especially when an urgent care visit becomes an ER referral or an ER visit turns into observation. A hospital indemnity ER benefit is designed to bring cash directly to you when a qualifying visit happens, so you can cover the parts your medical plan doesn’t fully absorb and keep your monthly budget from getting blindsided.
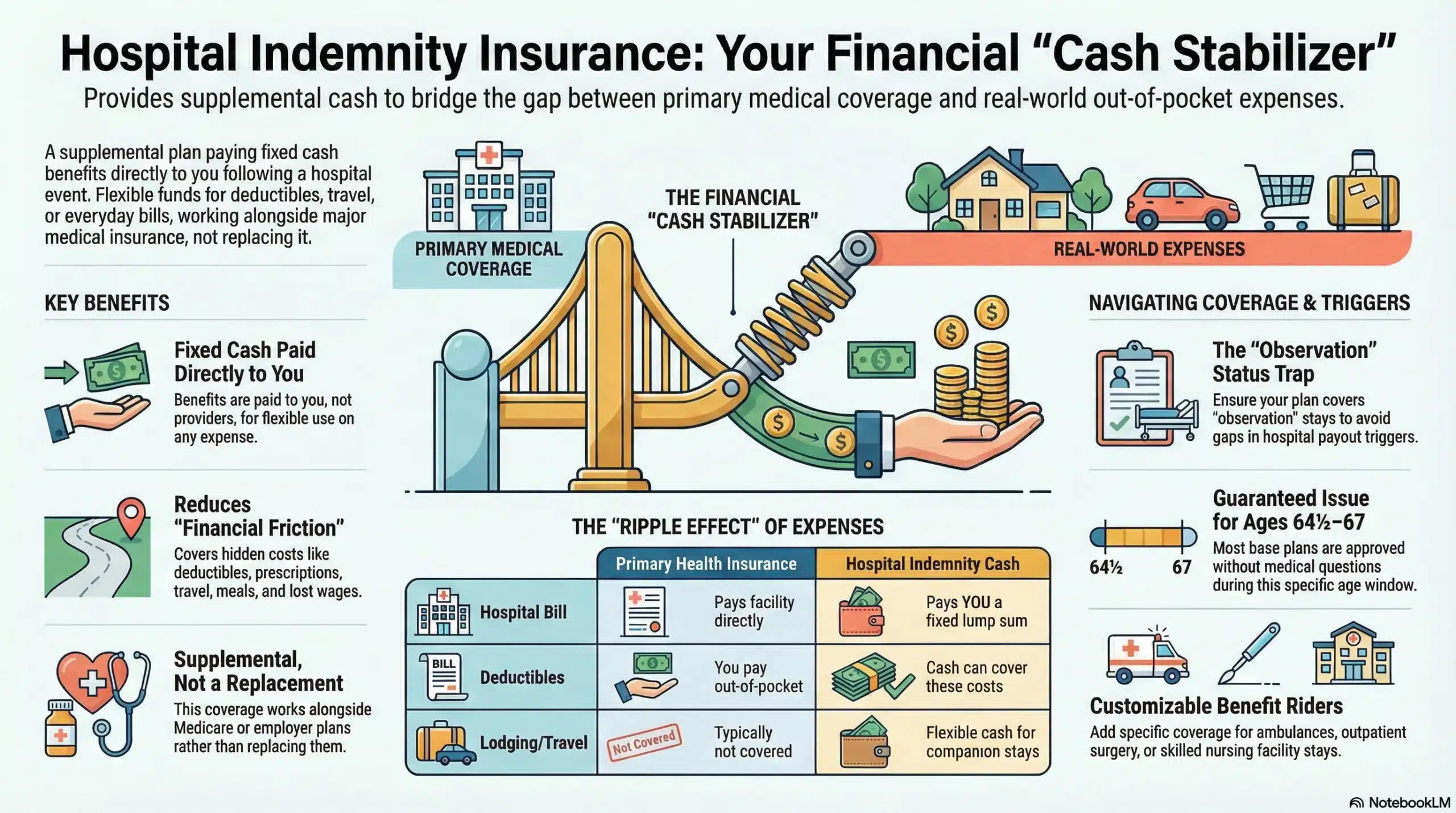
Hospital indemnity coverage is different from major medical insurance. It doesn’t try to negotiate or reprice a bill. Instead, it pays a defined amount when policy triggers are met, and then you decide how to use it—copays, coinsurance, prescriptions, transportation, meals, childcare, or everyday bills while you recover. That flexibility is exactly why many people like adding a hospital indemnity ER benefit even if they already have Medicare, Medicare Advantage, or employer coverage. The point is not “double coverage.” The point is predictable cash support when the ER happens at the worst possible time.
At Diversified Insurance Brokers, we help you design ER and urgent care benefits so they align with your real cost-sharing. That includes confirming whether the plan pays per ER visit, per urgent care visit, only when you are admitted, or in multiple layers depending on the pathway your episode of care follows. If you’re building a short-visit safety net, we also look at how ER benefits pair with observation coverage and ambulance coverage, because real-world episodes often follow a predictable sequence: transport, ER, observation, and sometimes admission.
When Hospital Indemnity Pays for ER and Urgent Care
A hospital indemnity ER benefit typically pays when you are treated in the emergency department and the visit meets the policy’s definition of a qualifying encounter. Some designs pay a fixed amount per ER visit. Others pay only when the ER visit results in observation or admission. Some plans include both types of structures, meaning you can receive a per-visit amount and then additional cash if your ER visit progresses into a longer stay.
Urgent care benefits are often structured separately from ER benefits. A plan may pay a smaller per-visit benefit for urgent care than it pays for the emergency department. That can be useful because urgent care visits are frequent, and even a “smaller” bill can be disruptive if you have several visits in a year. When both benefits are included, the design can help cover a wider range of common scenarios—minor injuries, infections, after-hours care, imaging referrals, and conditions that require rapid evaluation but do not always become admissions.
The admission pathway matters. If your ER visit leads to observation or inpatient admission, the policy may pay additional benefits based on duration, classification, or admission status. That is why ER coverage should not be evaluated in isolation. A plan that pays a small ER amount but pays strongly for observation can perform very well for people who are frequently held for monitoring. The reverse can also be true for people whose ER events rarely become observation but still create meaningful bills.
If you want a deeper, simple explanation of how hospital indemnity plans can handle observation classifications, start here: Hospital Indemnity for Observation Stays: Avoid Surprise Bills. If you want the “definitions and why they matter” breakdown, this companion page is the best reference: Observation vs. Inpatient: How Cash Benefits Pay.
Why ER and Urgent Care Create Surprise Costs
Many people assume an ER visit is a single copay. In reality, ER episodes often create multiple layers of cost-sharing. You may see a facility charge and a separate professional charge. You may have coinsurance on imaging or certain outpatient services. You may have follow-up costs that appear days later when claims finalize. Even with good coverage, the timing of these costs can be frustrating because they arrive after the medical event has already disrupted your schedule and household.
Urgent care can also be unpredictable. A visit that starts as “simple” can turn into lab work, imaging, prescriptions, or a referral. If the urgent care center directs you to an ER, you can end up with two sets of cost-sharing for one health episode. This is where a hospital indemnity ER benefit and urgent care benefit can help: they pay defined cash based on the visit trigger, giving you a consistent way to offset these costs without having to guess what the final billing will look like.
For many households, the objective is not to eliminate medical costs entirely. The objective is to reduce the surprise and protect savings from being drained by repeated short visits. ER and urgent care riders are built for exactly that pattern—short, common episodes that happen more often than major hospital stays.
Pairing ER Benefits With Observation and Ambulance
Real ER episodes rarely stop at the ER visit itself. Many begin with transport, continue with evaluation in the emergency department, and then move into observation—sometimes for 10 to 20 hours, sometimes overnight, and sometimes longer. A strong design is one where benefits work together across that chain rather than leaving you with a gap at the exact point cost-sharing is highest.
A common “short-visit safety net” design includes three layers: an ER benefit (cash per visit), an observation benefit (cash for short stays under observation rules), and an ambulance rider (cash for transport costs). This trio mirrors how many episodes actually occur: transport → ER → short observation. If the stay becomes a formal admission, the hospital daily benefit becomes the next layer that can support inpatient copays and extended disruptions.
If you are building coverage around Medicare Advantage exposures, this is especially relevant because many MA plans have defined ER copays and may have separate cost-sharing for observation and short inpatient stays. A hospital indemnity plan can be designed to align with those copay structures so the policy feels “purpose-built” for your plan rather than generic. For context on Medicare Advantage pairing, review: Hospital Indemnity for Medicare Advantage Members.
Build an ER-to-Observation Safety Net
We’ll price ER, urgent care, observation, ambulance, and hospital daily benefits together so the plan pays across the full short-stay pathway.
Design Approach: Match Benefits to Real Copays
The best design is not the one with the biggest numbers. It’s the one that aligns to your real-world cost-sharing and your most likely visit patterns. If you rarely use urgent care but you have a meaningful ER copay, you may prioritize a stronger ER benefit and an observation benefit. If you have frequent urgent care visits and occasional ER escalation, you may want both benefits structured at levels that make repeated visits less disruptive.
It also helps to decide whether your primary goal is to reduce medical cost-sharing or to reduce household disruption costs. Medical cost-sharing includes copays and coinsurance. Household disruption costs include travel, meals, lodging, lost work time, and help at home while you recover. Because hospital indemnity pays you cash, it can support both goals, but the benefit design should reflect what you actually want the money to do.
Finally, consider the “status question.” If you are frequently held under observation rules rather than formally admitted, observation benefits become more important than inpatient-only benefits. If you want the clearest explanation of how that classification impacts cash benefits, revisit: Observation vs. Inpatient.
Design Examples (Common Scenarios)
Frequent Short Visits
If you have recurring urgent care use or periodic ER visits, a per-visit benefit can reduce the “death by a thousand cuts” effect of repeated copays and facility charges. Pairing that with observation coverage helps when visits become longer evaluations rather than admissions.
Common build: urgent care per-visit cash + ER per-visit cash + observation benefit for 7–24 hours + modest hospital daily benefit for conversion to inpatient.
Transport Exposure (Rural or Long Distance)
If you live far from a hospital or ambulance bills are a common concern, transportation coverage can be one of the most practical add-ons. An ER benefit then provides immediate cash at the facility level, and a hospital daily benefit supports longer stays.
Common build: ambulance rider (ground and/or air as available) + ER per-visit cash + moderate hospital daily benefit + observation benefit.
We’ll quote multiple carriers and show which designs deliver the best value per dollar of premium, then right-size benefits so you get meaningful protection without paying for riders that don’t match your exposure.
Who Benefits Most From ER and Urgent Care Cash Benefits
ER and urgent care riders tend to fit best for people who want budget predictability and who are more likely to experience short, repeatable episodes rather than long admissions. Medicare Advantage members often like these riders because MA plans commonly rely on fixed copays for ER visits and structured cost-sharing that can feel manageable until multiple services stack up in one episode. People managing chronic conditions may also like per-visit cash benefits because periodic evaluations, monitoring, or flare-ups can create repeat costs in a single plan year.
Budget-conscious households also benefit because the cash helps protect savings from being used for routine medical disruption costs. Even when bills are not catastrophic, they can be stressful and inconvenient. A small, predictable cash benefit can reduce that friction and help keep your finances stable during the year.
Claim Basics: What Usually Triggers Payment and What to Keep
Most ER and urgent care benefits are triggered by evidence of a qualifying visit, such as a bill, visit summary, or documentation showing the date and location of service. Observation and inpatient benefits are typically triggered by facility documentation showing status and duration. Policies differ on limits (such as per-year maximums or per-visit rules), so the right approach is to verify the exact claim requirements for the carrier and state where you enroll.
We explain how claims are typically filed for the plan you choose, what documents are usually needed, and how to keep benefits aligned if your medical plan changes over time.
Related Hospital Indemnity Pages
Use these pages to compare benefit triggers and build a complete short-visit protection design.
Related Medicare Pages
If you’re coordinating ER benefits with Medicare decisions, these pages add helpful context.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
ER & Urgent Care Hospital Indemnity FAQs
Is urgent care paid the same as the emergency room?
Usually not. Many plans treat urgent care as a separate per-visit benefit with its own amount and limits. ER benefits are commonly higher and may have different triggers.
Will the ER benefit pay if I am treated and released?
Often yes, as long as the visit meets the policy definition of a qualifying ER encounter and any waiting periods or limitations have been satisfied. Observation and inpatient benefits are typically separate.
What if my ER visit becomes observation?
Depending on the design, you may receive an ER per-visit benefit and then a separate observation benefit if the policy includes one and the observation trigger is met. Policies vary, so we confirm how benefits transition or stack.
What if my ER visit becomes an inpatient admission?
If you are formally admitted, inpatient benefits such as a daily hospital confinement benefit may apply, subject to the policy rules. This is why ER benefits are often paired with observation and inpatient coverage.
Do I need an ambulance rider?
If ambulance costs are a meaningful exposure for you, the rider can be valuable. Limits for ground and air transport vary by plan and state, so we match the rider to your likely risk and location.
What documents are typically needed for a claim?
Commonly, a bill or visit summary showing the date, location, and type of service is sufficient for ER or urgent care benefits. Observation or inpatient benefits may require documentation showing status and duration.
Can I add ER or urgent care benefits later?
Sometimes, but health questions may apply and a new waiting period can start. If ER and urgent care cash benefits are central to your strategy, adding them upfront is often simpler.
Is hospital indemnity a replacement for major medical or Medicare?
No. Hospital indemnity is supplemental coverage that pays fixed cash benefits when covered events occur. It is designed to work alongside Medicare, Medicare Advantage, or employer coverage.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers (NPN 20471358), is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, Group Health, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient. Visitors who want to explore current annuity rates and compare options across multiple insurers can also use this annuity quote and comparison tool.
