What is Self Funded Group Health Insurance

Jason Stolz CLTC, CRPC
Self-funded group health insurance is a healthcare funding structure where an employer pays employee medical claims directly instead of paying fixed monthly premiums to an insurance carrier. While the definition sounds simple, modern self-funded group health insurance has evolved into a highly engineered financial strategy combining actuarial science, predictive modeling, pharmacy cost management, stop-loss risk transfer, and population health analytics. For many employers, moving toward self-funded group health insurance represents a shift away from passive premium purchasing and toward actively managing healthcare costs as a controllable business expense.
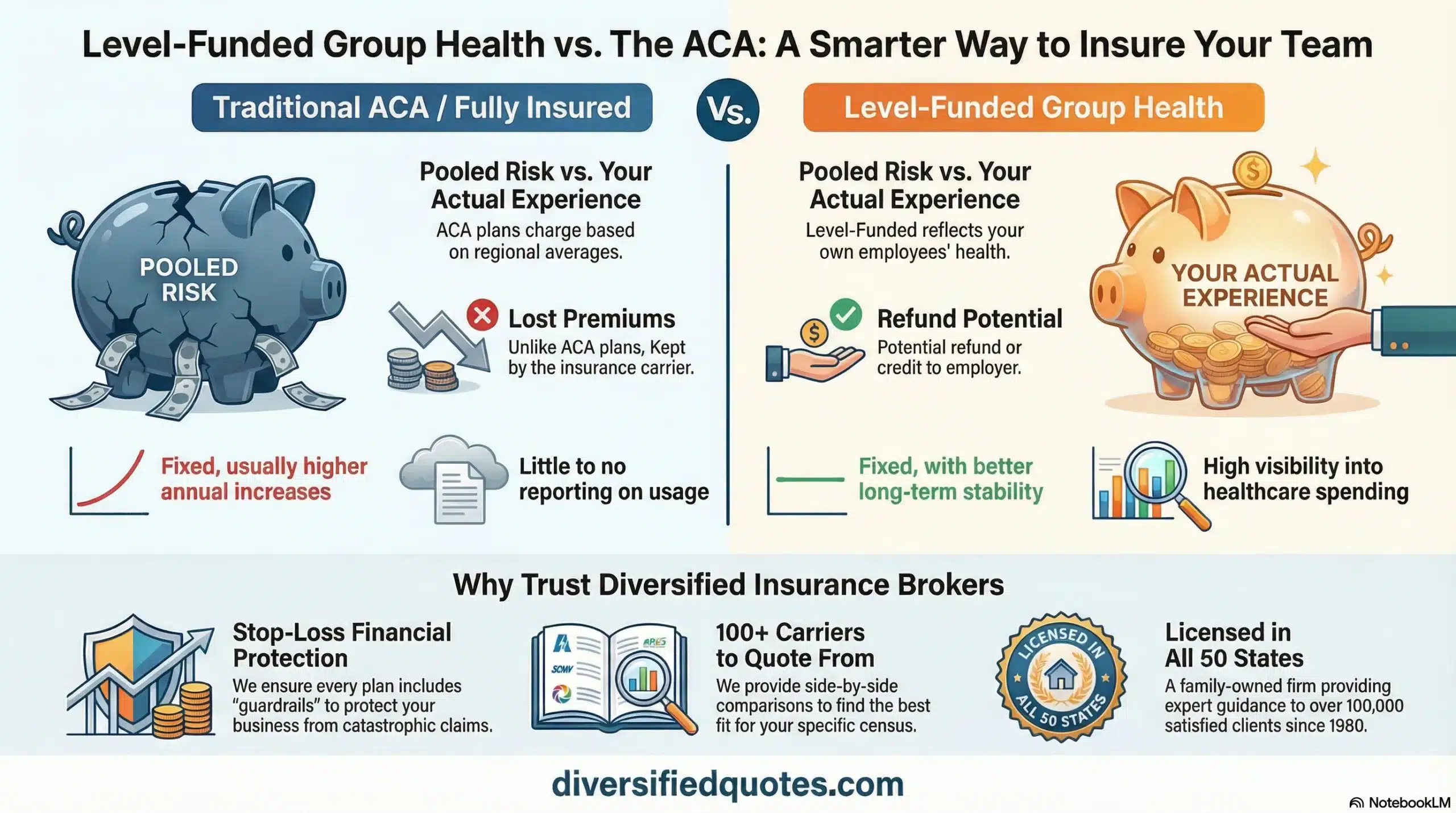
In traditional fully insured health plans, employers pay predictable premiums and transfer claims risk to an insurance carrier. Over time, those premiums are influenced by pooled regional performance, carrier risk margins, and trend assumptions that may not reflect the specific employer’s workforce. Self-funded group health insurance changes this relationship. Employers retain claims dollars, gain visibility into utilization patterns, and can deploy targeted cost control strategies that simply are not possible under traditional insurance models.
Employers evaluating self-funded group health insurance typically compare it to traditional group health insurance and hybrid funding approaches like level-funded employer health plans. Each model exists on a spectrum balancing risk transfer and financial control. Self-funded group health insurance sits at the highest level of employer control, customization flexibility, and claims transparency.
For organizations willing to invest in data-driven healthcare strategy, self-funded group health insurance can transform healthcare from a fixed cost line item into a controllable, optimizable financial system that improves over time as employers gain more insight into claims drivers and employee health patterns.
Evaluate If Self-Funded Group Health Insurance Lowers Long-Term Costs
See multi-year employer cost projections using real claims modeling, stop-loss scenarios, and pharmacy trend forecasting.
Request Employer Cost StudyThe Financial Architecture Behind Self-Funded Group Health Insurance
Modern self-funded group health insurance programs are built around multiple financial protection and cost management layers working together. At the foundation is actuarial claims forecasting, which estimates expected claims based on workforce demographics, historical claims experience when available, geographic healthcare costs, and industry utilization trends. Employers fund expected claims through structured funding accounts or claim payment reserves.
Above expected claims funding sits stop-loss insurance. Stop-loss coverage protects employers from catastrophic individual claims and high aggregate claim years. Specific stop-loss protects against large claims from a single individual, while aggregate stop-loss protects against total plan claims exceeding expected thresholds. Together, these coverage layers create predictable maximum exposure levels while still allowing employers to benefit from low-claim years.
Third-party administrators (TPAs) manage claims processing, network access, regulatory reporting, and plan administration. Many TPAs also provide advanced analytics dashboards that allow employers to monitor claims trends in near real-time. Over time, this data becomes one of the most valuable strategic assets in a self-funded group health insurance program.
Unlike traditional insurance premiums, which include carrier margin, premium tax, and risk padding, self-funded group health insurance typically focuses on actual claim cost plus transparent administrative expense. Over multi-year time horizons, this difference in cost structure often produces meaningful employer savings.
PBM Carve-Out Strategy and Pharmacy Cost Engineering
Pharmacy costs represent one of the fastest growing healthcare expense categories. In many fully insured plans, pharmacy benefits are bundled into carrier pricing, limiting employer visibility and negotiation leverage. Self-funded group health insurance allows employers to carve out pharmacy benefit management and contract directly with pharmacy benefit managers or specialty pharmacy vendors.
PBM carve-outs allow employers to control rebate pass-through structures, specialty drug sourcing, utilization management protocols, and formulary design decisions. Because specialty drugs often represent a disproportionate share of total pharmacy spend, even small strategy improvements can create significant savings.
Employers frequently combine PBM carve-outs with specialty drug management programs, gene therapy financial protection riders, and global sourcing strategies to mitigate catastrophic pharmacy exposure. As gene therapy and biologic drug pipelines continue expanding, PBM strategy is becoming one of the most critical components of long-term self-funded group health insurance planning.
Reference-Based Pricing and Direct Provider Contracting
Reference-based pricing (RBP) has emerged as one of the most advanced cost control tools available within self-funded group health insurance. Instead of paying provider billed charges or negotiated network discounts, RBP programs tie reimbursement to Medicare-based benchmarks or predetermined cost ceilings.
Employers implementing RBP strategies often pair them with patient advocacy programs and provider navigation support to ensure employees maintain access to care while controlling cost escalation. Some employers expand further into direct provider contracting, negotiating bundled surgical pricing, direct primary care partnerships, and center-of-excellence specialty care agreements.
These direct contracting models can significantly improve price transparency while improving care quality consistency. These strategies are rarely available within fully insured health plan structures.
Group Captives and Alternative Risk Pooling Structures
Some advanced self-funded group health insurance programs include captive insurance participation. Captives allow multiple employers to pool catastrophic risk while maintaining self-funded plan design control. This structure can stabilize stop-loss pricing volatility and create potential long-term financial participation benefits for employers.
Captive structures are typically best suited for financially stable employers with predictable claims trends and long-term healthcare strategy commitments. Participation often requires multi-year engagement and strong underwriting performance metrics.
Model PBM, RBP, and Stop-Loss Cost Scenarios
Run advanced cost simulations across pharmacy, claims volatility, and catastrophic exposure layers.
Run Advanced Cost ModelTax Efficiency and Employer Cash Flow Strategy
Self-funded group health insurance can provide meaningful financial advantages through premium tax avoidance, deductible claim expense timing, and improved working capital management. Employers can align claim funding with accounting cycles, improving financial statement predictability and liquidity planning.
Employers evaluating funding structure tax efficiency often compare strategies using resources like employer health tax optimization modeling.
Renewal Modeling and Multi-Year Healthcare Cost Forecasting
Traditional fully insured renewals often fluctuate based on carrier loss ratios and regional risk pool performance. Self-funded group health insurance allows employers to build multi-year claims trend projections using real utilization data. Employers can model best-case, expected-case, and worst-case claim scenarios and structure stop-loss coverage accordingly.
Employers often compare these projections against level-funded employer renewal modeling and traditional fully insured renewal cycles to determine optimal funding structure.
ERISA Governance, Compliance, and Fiduciary Responsibility
Self-funded group health insurance plans primarily operate under federal ERISA regulation rather than state insurance mandates. Employers maintain fiduciary responsibility for plan governance, vendor selection, and participant communication. While TPAs and compliance vendors manage day-to-day operational compliance tasks, employers remain legally responsible for plan oversight.
Organizations implementing self-funded group health insurance often build formal governance structures that include HR leadership, finance leadership, and external advisory partners to ensure long-term compliance and operational consistency.
Population Health Analytics and Long-Term Cost Control Strategy
One of the most powerful advantages of self-funded group health insurance is claims data transparency. Employers can identify chronic condition prevalence, specialty drug utilization trends, and high-cost treatment patterns earlier than traditional insured models allow.
Employers can then implement targeted chronic disease management programs, preventative care incentives, and specialty care steering programs designed to reduce long-term claims trends. Over time, these programs often produce compounding cost reduction benefits while improving employee health outcomes.
Design a 3–5 Year Employer Healthcare Cost Strategy
Build a multi-year plan combining stop-loss structure, PBM optimization, and claims analytics.
Request Strategic Healthcare PlanThe Future of Employer Healthcare Funding
Healthcare cost inflation continues to outpace general economic inflation. Employers increasingly require transparency, customization, and financial control over healthcare spending. Self-funded group health insurance continues expanding as stop-loss markets mature, analytics platforms improve, and employer demand for cost transparency increases.
For many organizations, self-funded group health insurance is transitioning from an alternative strategy into a long-term standard for employer healthcare funding optimization.
Advanced Employer Healthcare Funding Education
Explore deeper employer funding strategy, risk modeling, and stop-loss design.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
FAQs: Self-Funded Group Health Insurance
Is self-funded group health insurance legal for small businesses?
Yes. Self-funding is permitted under ERISA and can work for groups as small as 10 employees when paired with stop-loss insurance or level funding.
What happens if claims exceed expectations?
Stop-loss coverage reimburses the employer for claims above specific or aggregate limits, protecting cash flow.
Do self-funded plans still use provider networks?
Yes. Most use national PPO or reference-based pricing networks administered by a TPA.
Are self-funded plans subject to state mandates?
No. They are governed by federal ERISA rules, not state insurance laws, which gives greater design flexibility.
What’s the difference between level-funded and self-funded?
Level-funded plans blend fixed monthly payments with self-funded advantages, ideal for smaller employers seeking predictable budgeting.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers (NPN 20471358), is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, Group Health, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient. Visitors who want to explore current annuity rates and compare options across multiple insurers can also use this annuity quote and comparison tool.
