Hospital Indemnity Insurance: What It Covers & Costs

Jason Stolz CLTC, CRPC
Get Hospital Indemnity Quotes
Compare benefits, riders, and pricing from 100+ top-rated carriers—built to work alongside Medicare or employer coverage.
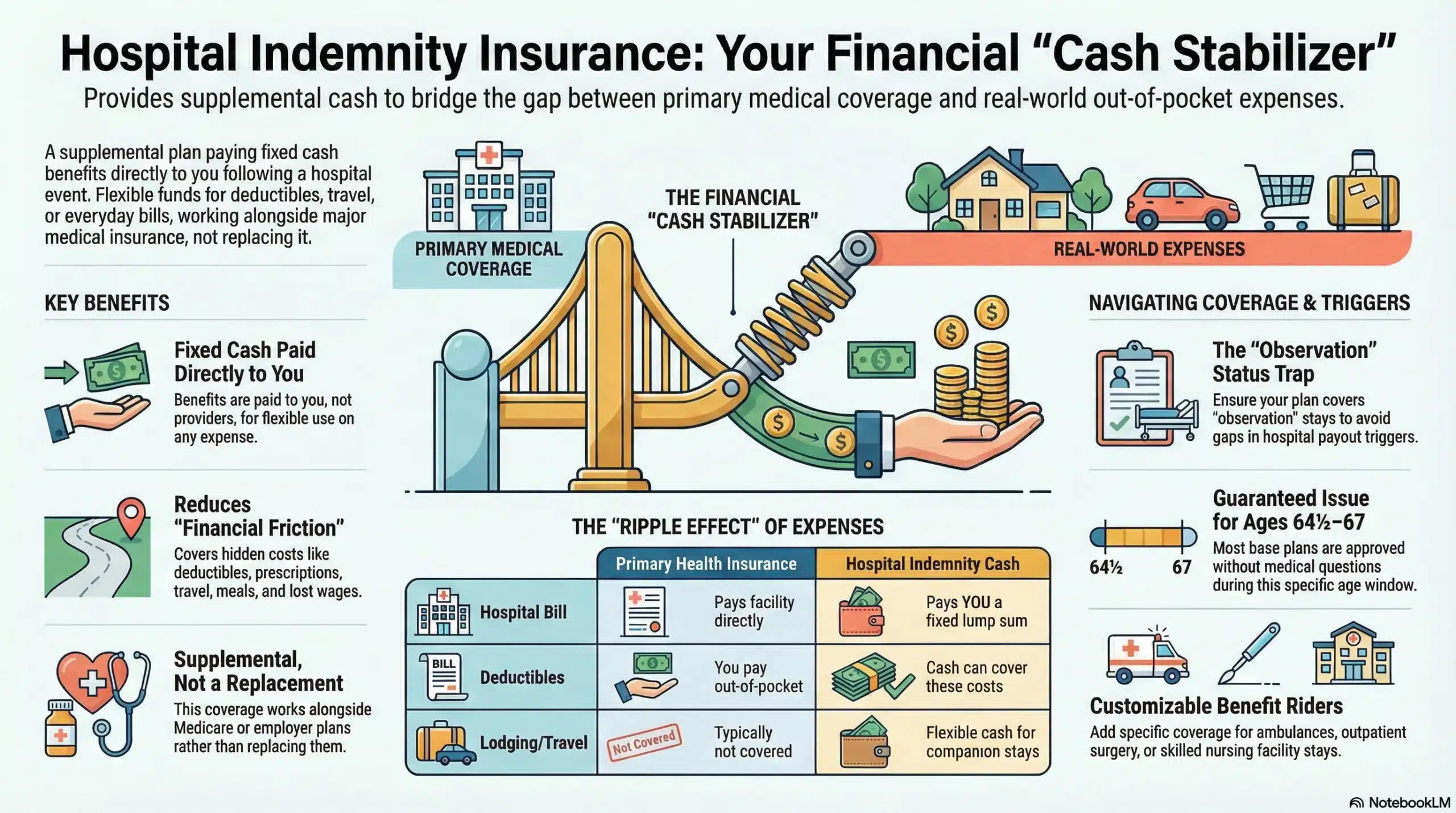
Hospital indemnity insurance is supplemental coverage that pays fixed cash benefits directly to you when a covered hospital event happens. It is not major medical insurance and it is not designed to replace Medicare, employer coverage, or an ACA plan. Instead, it’s designed to reduce the “financial friction” that shows up around hospital care—deductibles, copays, coinsurance, prescriptions, transportation, meals, lodging for a companion, and the everyday bills that don’t pause just because you’re dealing with a health event.
What makes hospital indemnity different is how it pays. Your primary coverage (Medicare, Medicare Advantage, employer coverage, or an individual health plan) generally pays providers and facilities according to its rules. A hospital indemnity plan, by contrast, pays a pre-defined benefit schedule to you after a covered event—typically using trigger rules such as inpatient admission, observation status, confinement days, or specific covered services. That cash benefit is flexible. You can use it for medical costs, but you can also use it for non-medical needs like travel, lodging, childcare, pet boarding, and household expenses.
See Your Hospital Indemnity Options
We’ll compare multiple carriers, confirm state availability, and tailor benefits and riders to the way care actually happens.
At Diversified Insurance Brokers, we help clients design hospital indemnity coverage so it matches how care actually happens. That means we don’t just pick “big numbers.” We start with the benefit triggers (what counts, what doesn’t, and why), confirm state-specific availability, then build a benefit stack that reduces surprise gaps—especially around observation versus inpatient classification, outpatient procedures, and the recovery phase after discharge. If you want a deeper explanation of the most common “why didn’t it pay?” scenario, read Observation vs. Inpatient: How Cash Benefits Pay.
What Hospital Indemnity Insurance Covers (In Plain English)
Hospital indemnity coverage generally focuses on hospital-based events and pays according to a defined schedule. The most common base benefits are a daily hospital confinement benefit and/or a lump-sum hospital confinement benefit. Some plans also include (or allow) benefits tied to emergency room/urgent care, observation stays, outpatient surgery, rehab/therapy visits, ambulance, skilled nursing facility stays, and other common “real world” add-ons that influence out-of-pocket spending around a hospital episode.
A helpful way to think about hospital indemnity is as a “cash stabilizer.” Your main coverage determines what providers charge you and what you owe. Hospital indemnity helps you absorb the out-of-pocket impact and the ripple effects that happen when life is disrupted. That ripple effect is usually the reason people like these plans. It’s not just the hospital bill. It’s the travel. It’s the prescriptions. It’s the time off work. It’s the companion lodging, meals, and the sudden need to keep household spending moving while you recover.
Because these are fixed-benefit policies, definitions matter. A plan doesn’t decide whether an event is “serious enough.” It pays when the event matches the policy definition and documentation supports that the trigger occurred. The best results happen when the plan is designed around the triggers you are most likely to experience—especially because modern hospital care frequently uses observation status for monitoring and workups before a formal inpatient admission is made.
How Benefits Pay (And Why Observation Rules Matter)
Most hospital indemnity plans pay benefits in a few common patterns. One pattern is a daily benefit—you choose a per-day cash amount and the plan pays that amount for a specified number of covered days per confinement, per year, or according to plan limits. Another pattern is a lump-sum benefit—a one-time payment for a covered confinement, sometimes with a partial benefit for short stays and a full benefit for longer stays based on the plan’s hour thresholds.
The confusion often comes from how the hospital labels a stay. You can be in a hospital bed overnight and still be classified as observation instead of inpatient. That classification affects medical billing and it can affect how a hospital indemnity plan triggers benefits. Many plans address this with observation-specific language—such as a defined benefit for a 7–24 hour stay, or a partial percentage payout for a short admission that does not meet a 24+ hour threshold. Some plans also separate “observation admission” from “inpatient admission” benefits. This is exactly why we recommend understanding classification before you buy, not after a claim surprises you. If you want the clearest breakdown, start here: Observation vs. Inpatient: How Cash Benefits Pay.
Another common payout pattern happens at the beginning of an episode. Many real-world episodes start in the emergency room or urgent care. Some plans include or offer an ER/urgent care benefit that pays cash for a qualifying visit, and some designs coordinate that benefit when the ER visit leads to observation or an inpatient admission. If you want to understand when that front-end cash can apply, this page is a helpful companion: ER & Urgent Care: When Hospital Indemnity Pays.
Who Hospital Indemnity Coverage Fits Best
Hospital indemnity coverage is most useful for people who want a predictable cash benefit to reduce hospital-related out-of-pocket exposure. Many Medicare enrollees like it because it can provide cash that helps with deductibles and cost-sharing, and because it can help stabilize spending even when plan cost-sharing changes year-to-year. People with employer coverage also use hospital indemnity as “gap support,” especially when they have higher deductibles, larger coinsurance percentages, or a family plan where hospital events can create significant out-of-pocket impact quickly.
Caregivers often like hospital indemnity for a different reason: it creates cash flexibility when life is disrupted. A hospital event can trigger travel, missed work, meals away from home, companion lodging, childcare needs, and household logistics. A supplemental cash benefit can reduce how much of that disruption turns into credit card balances or emergency fund withdrawals.
Hospital indemnity can also fit people who simply prefer a simple benefit structure. Instead of trying to predict exactly what a hospital will bill, you choose a benefit schedule that matches your risk tolerance and your budget. When an event happens, the plan pays the fixed benefit according to the contract. The most important part is making sure the triggers you choose align with the way you expect to enter and move through care—ER, observation, inpatient admission, outpatient procedures, and recovery.
Typical Costs and “Simple Math” Examples
Hospital indemnity premiums depend on your age, state, selected benefit amounts, optional riders, and the plan design available where you live. Some plans offer household discounts or multi-insured pricing, and many include a one-time policy fee depending on carrier and state. The best way to shop these plans is not to guess the “average price,” but to compare multiple designs side-by-side so you can see what your premium buys you in benefits and triggers.
Here are examples of how people often think about benefits in practical terms. A daily benefit design is often chosen when the goal is to create cash flow that matches multi-day hospital stays. A lump-sum design is often chosen when the goal is a single payment per confinement that can help with deductibles or a larger expense category. Some clients choose both because the combination can cover a wider range of real hospital patterns, especially when observation and inpatient classification varies.
Example scenario thinking can look like this: if you choose a $250/day daily hospital benefit for up to five days, a two-day covered inpatient stay could produce $500 in cash benefits—subject to the plan’s definitions and day counting rules. If your plan includes an observation benefit and you experience a 20-hour observation stay, the plan may pay an observation-level benefit rather than an inpatient daily benefit. If you choose a $1,000 lump-sum confinement benefit, a qualifying admission may trigger that one-time payment (sometimes with partial benefits for short stays). If you add outpatient surgery benefits, a same-day procedure may trigger a defined payout even without a hospital admission, depending on how the rider is structured.
The point is not that every event pays the maximum. The point is that the design should match the events you’re most likely to experience so the plan feels useful rather than random. That’s why we typically design around the “full arc” of care—how episodes start, how they are classified, where procedures occur, and what follow-up care looks like.
Design Benefits That Match Real Hospital Scenarios
We’ll compare carriers and then tailor triggers and riders around observation, inpatient, outpatient, and recovery needs.
Popular Optional Riders (And What They’re For)
Many hospital indemnity plans allow optional riders that make coverage feel more complete. The “right” riders depend on how you expect to use care and where you’ve seen out-of-pocket exposure show up in your household. Some people need stronger front-end benefits because episodes begin in the ER. Others care more about outpatient surgery and therapy copays. Others want stronger coverage for the recovery phase after discharge. The best rider strategy is the one that targets your most likely exposures rather than simply adding everything available.
Ambulance benefits are popular because transport costs can be unpredictable. Riders may pay for ground ambulance and, on some designs, air ambulance, usually subject to annual maximums. This is most useful for people who want additional cash protection for emergency transport events that can occur alongside a hospital admission.
Skilled nursing facility (SNF) daily benefits are designed for post-acute recovery when a patient transitions to a skilled nursing facility after hospitalization. If that risk matters to you, a daily SNF benefit can provide cash support for those covered days, subject to day limits and plan rules. If you want a focused explanation, see Skilled Nursing Facility Rider Explained.
Outpatient surgery benefits can pay cash for qualifying same-day procedures that occur in hospital outpatient departments or ambulatory surgery centers. These riders are often paired with the reality that modern care increasingly pushes procedures into outpatient settings. If you want to understand how outpatient and rehab riders work together, see Outpatient Surgery & Rehab Riders: What to Know.
Outpatient rehab and therapy benefits can pay per visit for PT/OT/speech therapy and sometimes limited chiropractic sessions, subject to annual caps and plan definitions. These benefits are often chosen by people who want to reduce the “death by a thousand copays” effect of repeated therapy visits after an injury or procedure.
Increasing daily hospital benefit riders (often described as 5% step-ups) are designed to keep the daily cash benefit from becoming stale over time by increasing the daily amount each policy year up to any plan cap. If you want the deeper explanation and why compounding versus simple increases matters, see Increasing Daily Benefit Rider (5% Step-Ups).
Diagnosis or condition riders may provide lump-sum benefits tied to covered first diagnoses (for example, certain cancer designs or heart attack/stroke benefit designs), sometimes with partial or recurrence benefits based on timing and plan rules. These riders are more “event-driven” and are usually chosen by people who want an additional cash layer for a specific category of major health event. For a focused overview of one common category, see Heart Attack & Stroke Cash Benefit Rider.
Practical support benefits can also exist on some plans, including travel companion lodging and pet boarding benefits, which are designed to help with the non-medical costs that show up during treatment and recovery. If that’s relevant to your planning, see Travel, Lodging & Pet Care Benefits Explained.
Guaranteed-Issue Window Near Age 65 (64½–67)
Some hospital indemnity designs offer a limited guaranteed-issue window where the base daily hospital benefit can be approved without medical questions—commonly for applicants around age 64½ to 67 based on effective date. This can be helpful for people who want coverage in place as they move into Medicare timing. It’s important to understand that guaranteed issue rules often apply to specific parts of the plan. Riders and lump-sum options may still require underwriting depending on the carrier and state. We confirm eligibility, timing, and what is included as guaranteed issue in your state before you apply.
If you are planning around Medicare decisions at the same time, it can help to view hospital indemnity as one piece of the overall strategy. Hospital indemnity pays you cash benefits, while Medicare or Medicare Advantage determines how services are covered and what cost-sharing you face. If you want a broader starting point for Medicare support, review Medicare Planning Services.
Helpful Hospital Indemnity Guides
Use these pages to understand benefit triggers and build a rider stack that pays across real care settings.
Observation vs. Inpatient: How Cash Benefits Pay ER & Urgent Care: When Hospital Indemnity Pays Outpatient Surgery & Rehab Riders: What to Know Skilled Nursing Facility Rider Explained
Related Benefit Topics
These rider explainers help you coordinate cash benefits across the full timeline of a medical event.
Increasing Daily Benefit Rider (5% Step-Ups) Heart Attack & Stroke Cash Benefit Rider Travel, Lodging & Pet Care Benefits Explained Medicare Planning Services
Financial Protection Essentials
Annuity income illustrations, international medical coverage, Medicare cost education, and disability planning resources.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
Hospital Indemnity FAQs
Is hospital indemnity insurance the same as health insurance?
No. Hospital indemnity is supplemental coverage that pays fixed cash benefits to you after covered events. It is not a substitute for major medical insurance, Medicare, or ACA-compliant coverage.
How do hospital indemnity benefits get paid?
Benefits are paid according to the policy schedule when the event matches the plan’s definitions (such as a covered confinement, admission status, or covered service). The cash is paid to you, and you decide how to use it.
Will it pay for observation stays?
Many plans include an observation benefit or observation language, often paying a partial benefit for shorter stays (for example, a 7–24 hour threshold) and different benefits for longer stays depending on plan rules. Exact hour thresholds vary by plan and state.
Can I add riders for surgery, rehab, ambulance, or skilled nursing?
Often yes. Common options include outpatient surgery benefits, rehab/therapy benefits, ambulance benefits, and skilled nursing facility daily benefits. Availability and limits vary by plan and state.
What waiting periods or pre-existing condition rules apply?
Many plans include a short waiting period (often around 30 days) and a pre-existing condition limitation period (commonly around six months), but the exact terms are plan- and state-specific. Your personalized quote will show the exact language.
Is there a guaranteed-issue option near age 65?
Some designs offer guaranteed-issue approval for the base daily hospital benefit for applicants in a limited age range around 65 (commonly described as 64½–67 based on effective date). Riders and other options may still require underwriting depending on the plan and state.
Does hospital indemnity work with Medicare or Medicare Advantage?
Yes. Hospital indemnity is supplemental and can be used alongside Medicare or Medicare Advantage because it pays you cash benefits that can help offset cost-sharing and related expenses. The plan does not replace Medicare coverage.
What’s the biggest “gotcha” to watch for?
The most common surprise is misunderstanding observation versus inpatient classification. A person can stay in the hospital overnight under observation status, which can affect how benefits trigger. Choosing a design that recognizes both statuses helps avoid gaps.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers (NPN 20471358), is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, Group Health, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient. Visitors who want to explore current annuity rates and compare options across multiple insurers can also use this annuity quote and comparison tool.
