Are Medicare and Long-Term Care Insurance the Same?

Jason Stolz CLTC, CRPC
Are Medicare and long-term care insurance the same? Not at all. They’re often mentioned in the same conversation because both relate to aging, healthcare, and retirement planning—but they solve two very different problems. Medicare is built for medical treatment and short-term recovery needs. Long-term care (LTC) insurance is built for ongoing help when someone needs assistance with daily life—especially when that help lasts for months or years.
This distinction matters because many families assume Medicare will “cover a nursing home” the way it covers a hospital stay. In reality, Medicare’s nursing facility coverage is limited to skilled care in specific circumstances and for a limited time. Long-term custodial care—help with bathing, dressing, eating, transferring, toileting, or supervision due to cognitive decline—is typically outside Medicare’s design. If you plan correctly, you can layer Medicare and long-term care coverage so each does what it’s best at and your savings are protected from unnecessary spend-down.
Compare Medicare vs. Long-Term Care Coverage
We’ll help you see what’s covered, what’s not, and how to fill the gaps with the right plan for your situation.
📞 Call 800-533-5969 or visit our Contact Page
How Medicare Works (and Why People Assume It Covers Long-Term Care)
Medicare is a federal health insurance program designed primarily to cover acute medical care. Think of doctor visits, hospital stays, medically necessary procedures, outpatient services, and short-term rehabilitation after a health event. When you are sick, injured, or recovering, Medicare is often the core payer that keeps medical bills from becoming overwhelming.
That’s also why the confusion persists. A hospital stay and a rehab stay can look similar on paper: a person is in a medical facility, receiving care, and there are nurses involved. But Medicare’s focus is on medical necessity and skilled treatment. Once a person no longer requires skilled nursing or skilled therapy to improve or maintain function, Medicare coverage typically stops—even if they still need significant help to live safely day to day.
At a high level, Medicare is often described in “parts,” and each part helps with different medical costs. Part A is usually associated with inpatient and facility-related coverage. Part B covers outpatient and physician services. Part D focuses on prescription drugs. Medicare Advantage (Part C) is an alternative way to receive Part A and Part B benefits through a private insurance plan, often bundling additional features like dental or vision, but still operating within Medicare’s medical framework.
What Medicare Does Cover in a Facility Setting
Medicare can cover a limited stay in a skilled nursing facility when specific rules are met. This is where many families believe “Medicare covers the nursing home,” but it’s important to understand what that phrase actually means in Medicare language.
In general, Medicare’s facility coverage is tied to a qualifying medical event and a medical need. A typical example is a hospitalization for surgery, stroke, severe infection, or injury. After the hospital, a person may need skilled therapy (physical, occupational, or speech therapy) and skilled nursing to recover safely. In this scenario, Medicare may help pay for a short-term skilled nursing facility stay, because the goal is recovery and rehabilitation—not long-term custodial support.
The key takeaway is that Medicare’s nursing facility coverage is structured around skilled care. It’s designed for recovery periods, not for ongoing help with dressing, bathing, meal support, medication reminders, mobility assistance, or supervision due to memory impairment.
What Medicare Generally Does Not Cover
Long-term care, as most families experience it, is not primarily medical treatment. It’s ongoing help with the tasks that keep someone functioning safely. That includes hands-on assistance, stand-by assistance, supervision, and cueing—especially when chronic conditions, frailty, or cognitive decline make independent living unsafe.
Medicare generally does not pay for custodial care as a standalone need. Custodial care is the non-medical assistance someone needs with routine daily activities. Medicare may cover limited home health services in certain cases, but the presence of a nurse does not automatically mean the care is “skilled” in the Medicare sense. If the care need is ongoing personal support rather than skilled treatment, Medicare is typically not the solution.
To understand how insurance companies define these functional limitations, it helps to review Activities of Daily Living (ADLs). ADLs are commonly used in long-term care insurance to determine when benefits can begin.
What Long-Term Care Insurance Covers
Long-term care insurance exists to pay for the kind of assistance Medicare usually excludes: extended help when someone cannot safely perform everyday tasks on their own. The trigger is often a need for help with ADLs (commonly two or more), or a qualifying cognitive impairment that requires supervision for safety.
Unlike Medicare—which is tied to medical necessity and short-term recovery—long-term care insurance is designed for ongoing support. That support can take place at home, in an assisted living community, in memory care, or in a nursing facility. The goal is to preserve choice, keep care aligned with personal preferences, and protect retirement assets from being drained by multi-year care costs.
Depending on the policy, long-term care insurance can help pay for home health aides, in-home custodial care, assisted living, memory care, nursing home care for chronic needs, respite care, and adult day care. The exact covered services depend on the plan design, but the common thread is that it addresses the long-term, personal-care side of aging that Medicare doesn’t meaningfully fund.
If you want a starting point for estimating how care costs may look for your age and situation, you can use our Long-Term Care Insurance Calculator to model coverage and budgeting scenarios.
Medicare vs. Long-Term Care Insurance: The Difference in Plain English
The simplest way to think about the difference is this: Medicare is for medical treatment and short-term recovery. Long-term care insurance is for ongoing help with daily living. Medicare is a government program with defined medical benefits. Long-term care insurance is a private policy designed to fund extended care needs and protect assets.
Medicare’s facility coverage is limited and tied to skilled needs. Long-term care insurance can pay for custodial care in multiple settings, including assisted living, which Medicare does not cover as a general benefit. Medicare may cover therapy or skilled services in the home in certain situations, but long-term care insurance can cover personal care at home—often the #1 preference for most families when care begins.
If you are weighing long-term affordability and planning, another important difference is qualification. Medicare qualification is driven by age/disability and medical necessity rules. Long-term care insurance benefits are typically triggered by functional limitations (ADLs) or cognitive impairment, and the policy must be purchased while you are still healthy enough to qualify medically.
Medicare vs. LTC Insurance: Side-by-Side Snapshot
| Feature | Medicare | Long-Term Care Insurance |
|---|---|---|
| Primary purpose | Medical treatment and short-term recovery | Ongoing custodial/personal care support |
| Nursing facility coverage | Limited skilled nursing care (short-term, rules apply) | Custodial/ongoing care as defined by the policy |
| Assisted living | Generally not covered | Often covered (policy dependent) |
| Home care | Limited skilled services in qualifying situations | Personal/custodial home care benefits (policy dependent) |
| How benefits trigger | Medical necessity and program rules | ADL assistance needs and/or cognitive impairment |
| Funding | Government program | Private insurance policy |
How Medicare and Long-Term Care Insurance Work Together
In many well-built retirement plans, Medicare and long-term care coverage are layered—not confused. Medicare covers the medical side: hospital care, physicians, diagnostics, medically necessary treatments, and short-term rehab when the goal is recovery. Long-term care insurance covers the daily-life side: ongoing assistance when the goal is safety, stability, and support.
A common sequence looks like this. A health event occurs and Medicare covers the hospital episode. Next, Medicare may cover a period of rehab or skilled services if the rules are met. If recovery reaches a plateau and the person still needs help with daily activities, the situation becomes custodial care. That is where a long-term care policy can step in, so the family is not forced into a private-pay burn rate that can quickly erode savings.
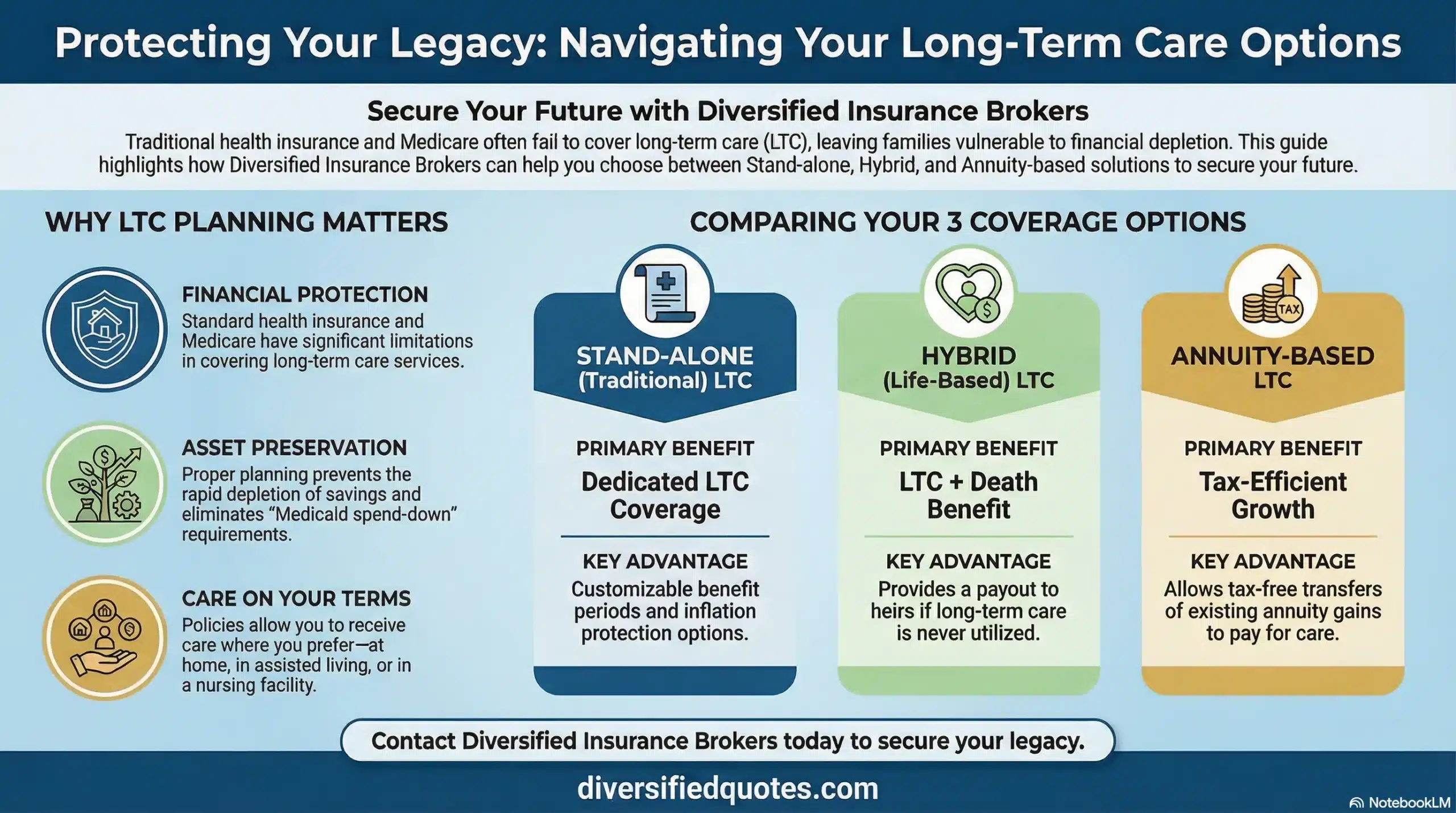
Some families also explore alternative ways to fund care risk if traditional long-term care insurance is not a fit. Depending on goals, that can include hybrid life/LTC designs or annuity-based options. If you’re evaluating how these strategies fit, reviewing different policy structures and costs with an advisor can clarify what actually solves your problem versus what simply sounds appealing in marketing.
Who Should Consider Long-Term Care Insurance?
Long-term care insurance is often most useful for people who want to protect assets and preserve options—especially households that could absorb premiums but would feel significant pressure if faced with a multi-year care bill. It can be particularly valuable for families who want the flexibility of home care and assisted living options without the financial and emotional strain of last-minute decisions.
Timing matters. Many people explore long-term care coverage in their 50s to mid-60s, when underwriting is often more favorable and policy options may be broader. Waiting until a health event occurs can limit choices or prevent approval. If you’re considering coverage, it’s also helpful to review how to qualify for long-term care insurance so you understand what carriers look for and how to position your application.
The Bottom Line
Medicare and long-term care insurance are not the same—and treating them as interchangeable is one of the costliest planning mistakes families make. Medicare is an essential foundation for medical costs, but it is not designed to pay for extended custodial care. Long-term care insurance exists to fund that gap, preserve choices about where care happens, and protect retirement savings from being drained by long-term assistance needs.
If you want to know where your current plan leaves exposure—and what it would take to close that gap—an objective review can give you clarity and a realistic action plan.
Get Help Coordinating Medicare & Long-Term Care Coverage
We’ll show how to layer coverage, reduce financial exposure, and build a plan for future care needs.
Related Pages
Explore related long-term care and Medicare planning resources.
Financial Protection Essentials
Core strategies to protect retirement income, prepare for healthcare costs, and build long-term financial stability.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
FAQs: Medicare vs. Long-Term Care Insurance
Are Medicare and long-term care insurance the same?
No. Medicare is for short-term, medically necessary care. Long-term care (LTC) insurance covers ongoing custodial or personal care when you need help with daily activities.
Does Medicare pay for assisted living?
Generally no. Medicare does not pay for room, board, or custodial care in assisted living. LTC insurance can cover assisted living if your policy includes that setting.
How long will Medicare cover a nursing home stay?
Medicare may cover skilled nursing care up to 100 days after a qualifying hospital stay. Once you no longer need skilled care, Medicare coverage ends.
What does long-term care insurance typically cover?
Home health aides, assisted living, memory care, nursing homes, adult day care, and respite—focused on help with Activities of Daily Living (ADLs).
How do I qualify to trigger LTC insurance benefits?
Most policies pay when a licensed professional certifies that you need help with at least two ADLs or you have a qualifying cognitive impairment.
Does Medicare pay for in-home custodial care?
Medicare can cover short-term skilled home health services, not ongoing custodial help like bathing or meal prep. LTC policies can cover personal care at home.
Do I still need LTC insurance if I have Medicare and a supplement?
Yes, if you want protection for custodial care costs. Medicare (and Medigap) focus on medical bills, not ongoing support with daily living needs.
What if I can’t medically qualify for traditional LTC insurance?
Consider alternative strategies such as limited-underwriting coverage, hybrid life/LTC designs, or annuities that include LTC-style benefits and enhanced withdrawal features.
How much does long-term care cost, and how do I plan for it?
Costs vary by state and setting; many areas exceed $80,000 per year. Review local estimates and build a plan that blends insurance benefits with your assets.
Can Medicare and LTC insurance work together?
Yes. Medicare handles acute/rehab phases; LTC insurance takes over if you need ongoing custodial care at home, assisted living, or in a nursing facility.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers (NPN 20471358), is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, Group Health, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient. Visitors who want to explore current annuity rates and compare options across multiple insurers can also use this annuity quote and comparison tool.
