Group Health Insurance for Physician Practices

Jason Stolz CLTC, CRPC
Request a Group Health Insurance Review
Compare fully insured, level-funded, and self-funded plans designed for physician practices—clearly and side by side.
Group health insurance for physician practices is one of the most important—and most complex—benefit decisions a medical group will make. Whether you operate a small private practice, a multi-specialty clinic, or a growing physician-owned organization, your health plan impacts recruitment, retention, operating costs, and long-term sustainability. Unlike many businesses, physician practices also operate under reimbursement pressure, staffing volatility, and tight operating margins that make uncontrolled benefit costs especially painful.
At Diversified Insurance Brokers, we work with physician practices nationwide to design group health plans that balance cost control, provider access, regulatory compliance, and employee satisfaction. From fully insured PPO designs to level-funded and self-funded structures, we help medical groups evaluate practical options and implement a strategy that fits both today’s needs and tomorrow’s growth.
On this page, we’ll break down how physician practices typically approach group health insurance, the plan structures that tend to work best in healthcare environments, and the cost-control levers that help practices avoid disruptive renewals without reducing benefit quality.
Why Group Health Insurance Is Different for Physician Practices
Physician practices face a unique mix of pressures that most “standard small business” health plans are not designed to solve. The workforce is often highly compensated, the practice may include owners and employed clinicians, and the organization operates in a healthcare ecosystem where provider access matters more than marketing brochures. Plan decisions can also carry cultural weight inside a medical group, because clinicians tend to have strong opinions about networks, coverage design, and employee contributions.
Practices also commonly employ a mix of physicians, advanced practice providers, clinical support staff, administrative teams, and billing/operations staff. Those roles often have different utilization patterns and different expectations around plan design. A one-size-fits-all plan can lead to overspending, dissatisfaction, or both, particularly when the plan is built on conservative carrier assumptions instead of the practice’s real needs.
For this reason, physician practices often benefit from a customized group health insurance strategy rather than a generic plan that was designed to be “good enough” for a broad small-group market.
Common Challenges Physician Practices Face With Health Insurance
Most physician practices come to us after experiencing one or more predictable problems. The most common is renewal inflation that exceeds revenue growth. When a practice is on a traditional insured plan, rates can move sharply year over year with limited transparency, and leadership is often left with two bad choices: absorb the increase or shift costs to employees. Either approach can disrupt morale and recruiting.
Another common issue is the assumption that the practice is “too small” for better options. In reality, many physician practices qualify for alternatives that create better pricing mechanics, better predictability, and better reporting. Even when a group is not ready for a fully customized self-funded model, level-funded and hybrid structures can provide a middle path that improves transparency without introducing open-ended risk.
Recruitment and retention pressure is also a major factor in healthcare. Competitive benefits are no longer a “nice-to-have.” Health insurance is a core part of total compensation, and candidates compare it aggressively—especially when they are choosing between multiple offers.
Finally, practices often struggle with plan communication. When employees don’t understand how the plan works, utilization becomes inefficient and dissatisfaction rises. In healthcare environments, where staff are busy and burnout is real, confusion around benefits can become a persistent source of frustration.
Group Health Insurance Options for Physician Practices
Physician practices generally have three primary group health insurance structures to consider. The right fit depends on practice size, claims stability, cash flow, compliance needs, and how much control leadership wants over long-term costs. The best approach is usually to compare these structures side by side using the practice’s real demographics and goals.
Fully Insured Group Health Plans
Fully insured plans are the most familiar option. The practice pays a fixed monthly premium to an insurance carrier, and the carrier assumes all claims risk. These plans can be simpler to administer and predictable within the plan year, which makes them attractive for practices that want a straightforward implementation.
The tradeoff is control and transparency. Fully insured renewals often include conservative assumptions, carrier margins, and limited insight into what is driving cost. Over time, this can produce premiums that rise faster than the practice’s real utilization. Fully insured coverage can still make sense for very small practices or groups that prioritize simplicity over optimization, but it is rarely the most efficient long-term structure as the practice grows.
If you want the baseline foundation for employer plans, start with our group medical insurance overview.
Level-Funded Health Plans
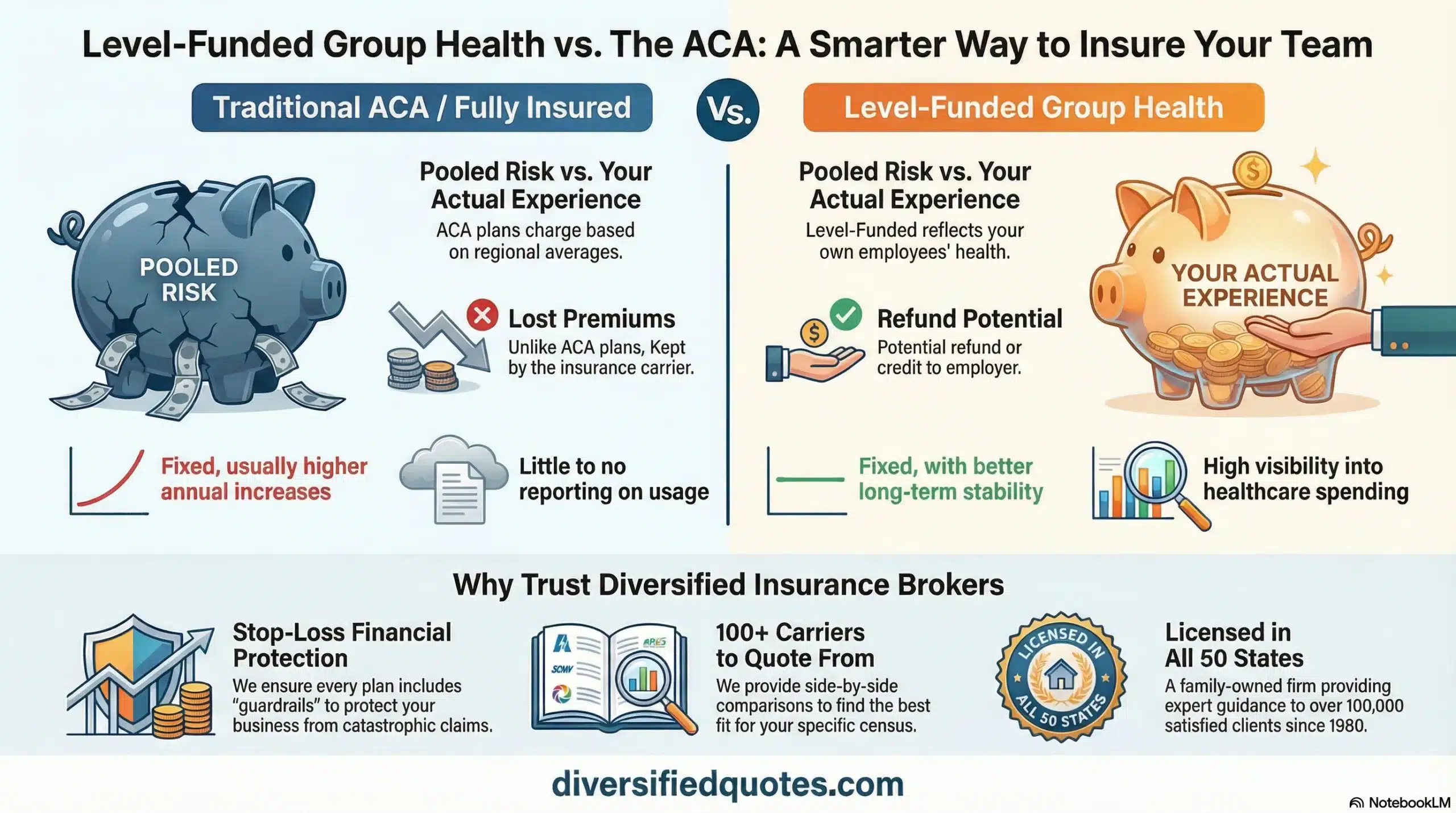
Level-funded plans combine features of insured and self-funded coverage. The practice pays a fixed monthly amount, but that payment is commonly built on expected claims rather than broad pooled averages. From a budgeting perspective, it feels like a fixed-premium plan, which is why physician practices often like it as a transition step.
The “enterprise advantage” of level-funding is that favorable claims experience can create meaningful savings. If claims are lower than expected, the practice may receive a year-end credit or refund based on the plan’s structure. If claims are higher than expected, stop-loss protection limits the downside. This creates a structure where good plan performance can benefit the practice rather than disappearing into pooled pricing.
To understand the broader mechanics, review what self-funded group health insurance is, which also helps frame why level-funded designs can create better transparency.
Self-Funded Group Health Plans
Self-funded plans allow physician practices to pay claims directly while using stop-loss insurance to protect against catastrophic losses. These plans typically offer the highest level of control, customization, and long-term savings potential because leadership can influence plan design, reporting, and vendor accountability more directly.
Self-funding can be especially attractive for physician practices that want visibility into cost drivers and prefer a structured, data-driven renewal process. It also allows practices to tailor plan features around their workforce and operating realities. The key requirement is governance: a self-funded plan should be managed intentionally, not treated like an “insured plan replacement.”
To pressure-test fit and tradeoffs, review the pros and cons of self-funded group health.
Owners, Partners, and Eligibility Considerations
Physician practices often have ownership structures that differ from typical small employers. Partners, shareholders, and physician-owners may want to participate in the plan alongside employed clinicians and staff. Eligibility depends on how the practice is organized and how individuals are classified for benefit purposes.
Getting this right is important for two reasons. First, it protects compliance. Second, it avoids avoidable plan disruption when the carrier or administrator requests documentation later. A clean eligibility structure also prevents confusion during enrollment, especially in practices where compensation and ownership vary by role and tenure.
In many practices, the goal is a plan that is simple to administer but flexible enough to reflect real roles inside the organization. That often means defining clear full-time thresholds, consistent waiting periods, and predictable employer contribution rules that leadership can repeat year after year.
How Practice Size Impacts Health Insurance Strategy
Practice size changes what “best” looks like because scale changes both pricing mechanics and risk tolerance. Solo and small group practices often assume they lack leverage, but even small groups can qualify for employer coverage that outperforms individual policies in stability and usability. The most important factor is designing eligibility and participation correctly so the plan is viable and repeatable.
Mid-sized practices often benefit from level-funded or partially self-funded structures because claims stability and cash flow can support better pricing mechanics while still keeping monthly costs predictable. These models often reduce the “renewal shock” problem that insured plans can create.
Larger physician groups and multi-location practices often move toward fully customized self-funded arrangements. At that point, leadership typically wants more control over vendor performance, pharmacy strategy, reporting cadence, and plan customization. The goal becomes long-term trend management rather than annual premium shopping.
If you’re unsure where the practical threshold begins for different plan types, reviewing minimum employees for group health insurance can help frame options realistically.
Cost Controls That Don’t Undermine Recruiting
For physician practices, cost control cannot come at the expense of recruiting. Clinicians and experienced staff have options, and benefits are a visible signal of stability. The best cost strategies usually focus on removing waste and improving plan efficiency—not simply shifting cost to employees.
One effective lever is offering multiple plan options rather than forcing one design on the entire workforce. A “value” plan can steer toward efficient in-network utilization, while a “buy-up” option can appeal to employees who prefer lower out-of-pocket costs. When designed correctly, this improves employee choice while controlling employer spend.
Contribution strategy is also critical. If contributions are too low, participation becomes fragile and morale suffers. If contributions are too high, payroll becomes inflexible and renewals become painful. The goal is a contribution approach that is competitive, sustainable, and simple enough to administer without constant exceptions.
Finally, communication matters. Clear benefits education reduces confusion and can meaningfully influence utilization patterns, especially around urgent care vs. ER usage, in-network navigation, and prescription basics.
Network Strategy and Provider Access Realities
Provider access is often more important in physician practices than in many other industries because employees are highly aware of provider quality and network limitations. A plan that looks cheaper on paper can become expensive if it drives out-of-network utilization or creates dissatisfaction due to restricted access.
Practices with multi-location footprints also need to ensure the network matches where employees live and work. When teams are distributed, network design becomes a strategic decision, not a default selection. The best outcomes usually come from starting with a strong network and then optimizing plan design and contributions within that network rather than choosing a narrow network purely to reduce premiums.
Pharmacy and Specialty Medications
Pharmacy spend is a common driver of rising costs, especially when specialty medications are involved. Many plans drift upward because pharmacy management is treated as a fixed component rather than an area that can be structured and governed. Even when medical claims appear stable, pharmacy trend can move quickly.
Better reporting, clear plan rules, and thoughtful vendor management often make a meaningful difference in pharmacy outcomes. The goal is to support appropriate access to needed medications while reducing waste, avoiding avoidable pricing inefficiencies, and improving predictability for renewals.
For practices comparing employer benefits against other forms of coverage, it can also help employees understand how employer plans fit into broader protection decisions. When appropriate, some organizations reference group vs individual insurance to help frame how employer benefits differ from personal coverage responsibilities.
Renewal Strategy and Long-Term Sustainability
Renewals are where physician practice plans either become stable or become a yearly disruption. A sustainable renewal strategy usually has three components. First, get the baseline right: network, plan structure, eligibility rules, and contributions. Second, implement modest, consistent adjustments rather than major swings every year. Third, start early enough to gather clean data and avoid rushed decisions.
Practices that rely on insured renewals often feel stuck because transparency is limited. Practices that use level-funded or self-funded structures often have more insight into what is driving cost, which makes renewals more manageable. The point is not that one structure is always superior—it’s that better information creates better decisions.
When the plan becomes a managed system instead of an annual shopping event, the practice usually experiences fewer employee disruptions and more predictable budgeting.
Why Physician Practices Work With Diversified Insurance Brokers
Diversified Insurance Brokers is an independent, fiduciary insurance agency licensed in all 50 states. We work with physician practices nationwide to design group health strategies that evolve with the practice as it grows. Because we’re independent, our recommendations are based on fit—not carrier incentives.
Our process is built to be practical. We compare plan structures side by side, clarify tradeoffs in plain language, and help practices implement coverage with clean eligibility rules and clear employee communication. The goal is a plan your team can understand, a cost you can predict, and a renewal process that stops being a yearly emergency.
If your practice is also building out a broader benefit strategy that includes elective benefits, you may find it helpful to review related options through our services page as you map out a long-term benefits stack.
Want a Side-by-Side Proposal for Your Practice?
Tell us your practice size and goals, and we’ll model practical plan options with clear tradeoffs.
Explore Group Health Insurance Options for Your Practice
Get a side-by-side comparison of group health plans designed for physician practices.
Related Group Health Insurance Resources
Explore additional pages that support plan comparison and eligibility decisions.
Financial Protection Essentials
Carrier reviews, retirement income planning tools, and specialized coverage resources for individuals and businesses.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
FAQs: Group Health Insurance for Physician Practices
Can small physician practices qualify for group health insurance?
Yes. Many physician practices with as few as two employees can qualify for group health insurance, including level-funded and self-funded options.
Are level-funded plans appropriate for medical groups?
Often, yes. Level-funded plans provide predictable costs with potential savings and are especially effective for physician practices with stable claims patterns.
Is self-funded health insurance risky for physician practices?
With proper stop-loss coverage, self-funded plans can limit risk while offering greater transparency and long-term savings.
Can physician owners be covered under the same group plan?
Yes. Physician owners and partners are commonly included in the group health plan alongside employees.
How often should a practice review its group health plan?
Annually at minimum. Practices with rapid growth or rising costs may benefit from more frequent reviews.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers, is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient.
