What are Activities of Daily Living

Jason Stolz CLTC, CRPC
Activities of Daily Living (ADLs) are the six essential, hands-on self-care functions that determine whether someone can live independently or requires long-term care support. In the world of long-term care insurance, ADLs are not just medical terminology — they are the contractual triggers that determine when benefits begin. If you or a loved one cannot perform at least two of these activities without substantial assistance for an expected period of 90 days (or if there is a qualifying cognitive impairment), most long-term care policies will activate benefits. Understanding ADLs is critical when evaluating whether you should buy long-term care insurance, how policies pay, and how to structure benefits that align with real-world care needs. ADLs also intersect with questions many families ask, such as whether Medicare covers nursing home care, how Medicare Supplement vs. Medicare Advantage plans differ in coverage, and what happens if care is needed at home versus in a facility.
The six core ADLs used in most policies are bathing, dressing, eating, toileting, continence, and transferring. Bathing includes safely getting in and out of a shower or tub and washing without risk of falling. Dressing involves selecting appropriate clothing and managing buttons, zippers, and braces. Eating refers strictly to the act of getting nourishment into the body — not meal preparation. Toileting includes safely using the bathroom and performing related hygiene. Continence refers to control of bowel and bladder function. Transferring means moving safely from bed to chair, wheelchair, or standing position. A policy typically requires “substantial assistance,” meaning hands-on help or standby supervision to prevent injury. For individuals with Alzheimer’s disease or other forms of dementia, cognitive impairment can also trigger benefits even if physical ADLs remain intact. Families often combine LTC coverage with other financial planning tools such as retirement tax strategies, retirement sustainability planning, and guaranteed income options like guaranteed income at age 65 or guaranteed income at age 70 to ensure assets last if ADL support becomes necessary.
Compare Long-Term Care Policies Based on ADL Triggers
We’ll explain exactly how different carriers define “substantial assistance,” elimination periods, and cognitive impairment qualifications.
ADLs are often confused with Instrumental Activities of Daily Living (IADLs), which include tasks such as managing medications, preparing meals, shopping, housekeeping, transportation, and handling finances. While IADLs are important indicators of declining independence, most long-term care insurance policies do not pay benefits based solely on IADL limitations unless cognitive impairment is present. For example, someone who can physically bathe and dress independently but cannot manage bills may not qualify under the ADL trigger. This distinction is vital when families evaluate home-based care options such as adult daycare services or consider broader income protection strategies like income protection insurance or disability income insurance with COLA earlier in life.
When an ADL claim is filed, insurers typically require certification from a licensed healthcare practitioner confirming the inability to perform at least two ADLs or documenting severe cognitive impairment. They will review medical records, therapy notes, hospital discharge paperwork, medication lists, and home health assessments. Precision matters. Instead of stating “needs help transferring,” documentation should specify “requires two-person assist to transfer from bed to wheelchair.” Policies also contain an elimination period — commonly 30, 60, or 90 days — during which care must be received before reimbursement begins. Some policies count calendar days, others count service days. Understanding these mechanics before purchasing coverage is crucial, which is why working with a best independent long-term care insurance broker can make a measurable difference in claim success later.
Care needs triggered by ADLs do not automatically require nursing home placement. Many individuals begin with part-time home health aides, progress to assisted living, and eventually require memory care or skilled nursing. Benefit structure must match realistic care paths. For instance, home care hourly costs can exceed facility daily rates in some regions, and inflation protection riders may be essential to preserve purchasing power over decades. Families also weigh hybrid solutions such as hybrid life and LTC policies that provide a death benefit if care is never needed. Broader estate strategies — like Irrevocable Life Insurance Trusts (ILITs) — may also play a role in preserving assets when ADL-triggered care becomes prolonged.
Planning ahead for ADL-related care means evaluating benefit amounts, benefit periods, shared-care riders for couples, and inflation options. It also means understanding what public programs will and will not cover. Medicare is primarily short-term and medically necessary coverage; custodial care driven by ADL limitations is largely excluded outside limited skilled nursing situations. Medicaid may eventually cover long-term care but requires asset qualification. For families concerned about future insurability or complex health histories, other specialized coverage topics — such as life insurance for atrial fibrillation or life insurance for hepatitis C — highlight how early planning preserves options before health changes affect eligibility.
Protect Retirement Assets from ADL-Driven Care Costs
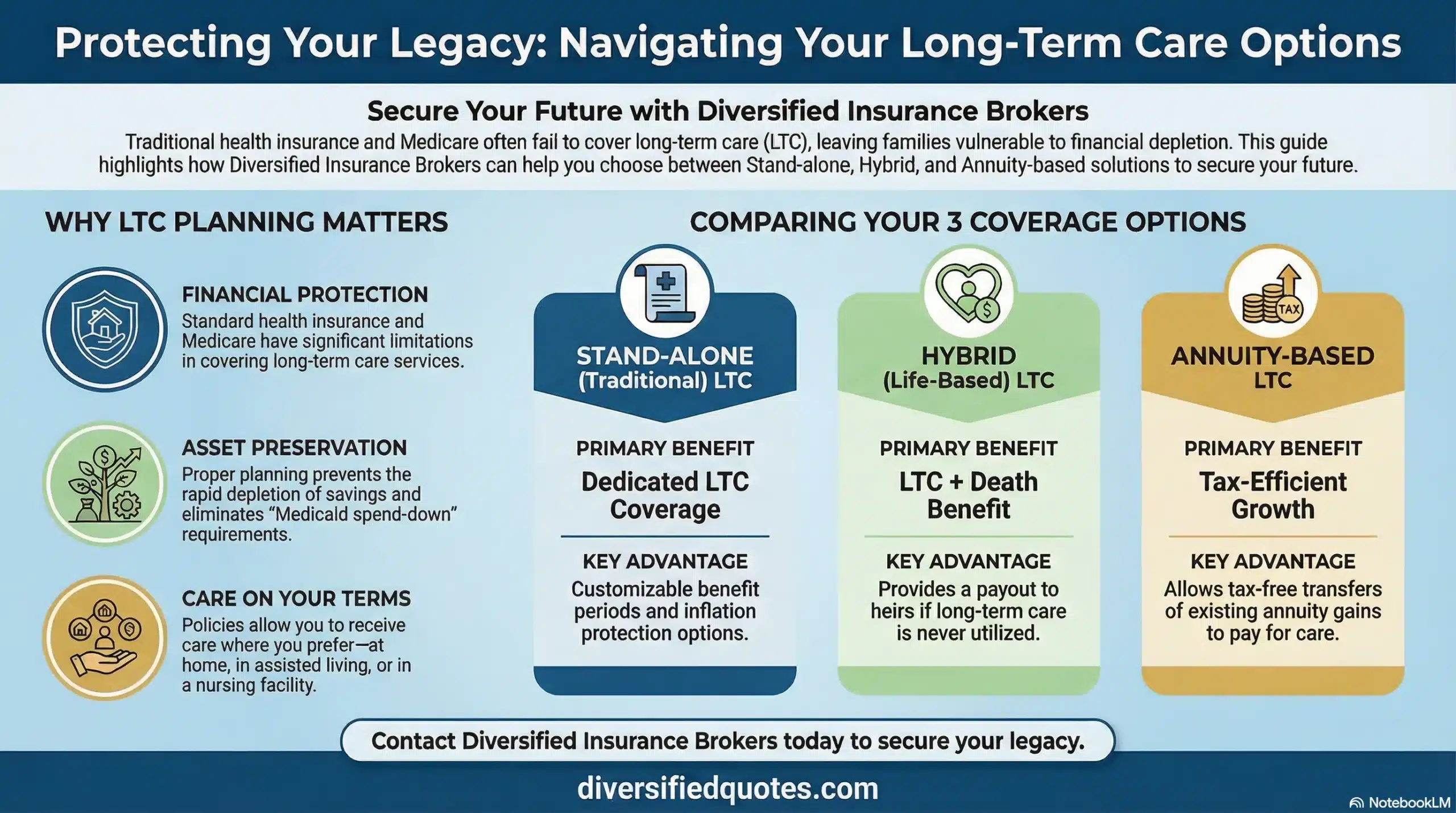
Compare traditional and hybrid LTC options and see how elimination periods and benefit pools affect long-term outcomes.
Related Long-Term Care & Planning Guides
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
FAQs: Activities of Daily Living (ADLs)
What are the six ADLs?
Bathing, dressing, eating, toileting, continence, and transferring. These hands-on self-care tasks are the industry standard for evaluating functional ability.
How many ADLs must I need help with to trigger LTC insurance benefits?
Most policies require substantial assistance with at least two ADLs, or a qualifying cognitive impairment requiring supervision, as certified by a licensed professional.
Do IADLs count toward eligibility?
Typically no. Instrumental ADLs (like shopping or housekeeping) support independent living but generally don’t trigger benefits unless cognitive impairment criteria are met or your policy explicitly allows it.
What’s the difference between standby and hands-on assistance?
Hands-on means physical help to complete the task. Standby means a helper is present to prevent falls or cue the person; many policies recognize both as “substantial assistance.”
Who decides whether I qualify for benefits?
An insurer-approved licensed health professional assesses your abilities, documents ADL limitations, and creates or reviews a plan of care.
How does cognitive impairment factor in?
Severe cognitive impairment (e.g., dementia) that requires continual supervision for safety can qualify you for benefits even if you can still perform ADLs physically.
Do I have to be in a facility to receive benefits?
Not necessarily. Many policies cover home care, assisted living, and adult day care, in addition to nursing facilities—subject to your contract terms.
What documents help with a smoother claim?
Professional assessments, physician notes, therapy reports, discharge summaries, home-health visit logs, and a written plan of care aligned with actual services.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers (NPN 20471358), is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, Group Health, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient. Visitors who want to explore current annuity rates and compare options across multiple insurers can also use this annuity quote and comparison tool.
