Does Medicare Cover Nursing Home Care?
Does Medicare Cover Nursing Home Care?

Jason Stolz CLTC, CRPC
Does Medicare Cover Nursing Home Care?
Get clarity on skilled nursing vs. custodial care, what Medicare actually pays for, and how to close the long-term care gap.
Does Medicare cover nursing home care? Yes—but only in narrow circumstances, for a limited time, and only when the care you need is classified as skilled. That’s very different from what most families mean when they say “nursing home care.” If someone needs ongoing help with bathing, dressing, eating, walking safely, or supervision due to memory loss, Medicare usually does not pay for that custodial, long-duration care.
This distinction matters because long-term care expenses don’t arrive as a one-time bill. They tend to build over months or years, and the financial impact can change a retirement plan fast. Without a strategy, families often spend down assets, depend heavily on adult children, or scramble to qualify for Medicaid under strict eligibility rules. If you want a broader overview of where Medicare ends and long-term care planning begins, review Does Medicare Cover Long-Term Care?.
What Medicare Means by “Nursing Home” Coverage
Medicare’s nursing-facility help is primarily tied to skilled nursing facility (SNF) coverage under Part A. In plain language, Medicare can help when you are recovering after an illness, injury, or surgery and need daily skilled services—such as nursing care that must be performed or supervised by licensed professionals, or therapy services like physical or occupational therapy that are part of an active rehabilitation plan.
To qualify, Medicare generally expects a specific chain of events: you have a qualifying inpatient hospital stay, your doctor documents the need for daily skilled care, and you transition into a Medicare-certified SNF within the allowed time window. When those conditions are met, Medicare may cover part of the SNF stay. But the coverage is not intended for long-term residency, and it usually ends when skilled services are no longer medically necessary.
Families often experience this as a “coverage cliff.” The person may still need help every day—but if the remaining needs are custodial (help with ADLs) rather than skilled, Medicare’s role can end even though the care need continues. That’s why it helps to understand the bigger picture of how Medicare and long-term care solutions coordinate, including resources like Are Medicare and Long-Term Care Insurance the Same?.
Skilled Nursing vs. Custodial Care (The Divider That Drives Coverage)
The simplest way to think about Medicare coverage is this: Medicare pays for medical recovery, not long-term assistance. Skilled nursing care is tied to treatment and rehabilitation that require licensed medical involvement. Custodial care is the ongoing help many people need when they cannot safely function independently—help with toileting, bathing, dressing, transferring, eating, and supervision due to cognitive decline.
This is where many people get tripped up by terminology. A “nursing home” is a place, but Medicare coverage is based on the type of care. If the primary reason for staying is custodial support, Medicare generally doesn’t pay—regardless of the setting. If you want to see how long-term care plans define functional triggers, Activities of Daily Living is a helpful starting point because ADLs are a common trigger used by long-term care insurance designs.
When Medicare Can Help After a Hospital Stay
Medicare may help pay for a short skilled nursing facility stay after hospitalization. In many cases, this happens after events like a stroke, a serious infection, or major surgery where rehabilitation is expected to restore function. During that period, Medicare’s role is to fund skilled services while the patient is actively improving or requires daily skilled oversight.
The practical issue is that the skilled component can end before the person is fully independent. When therapy is complete or the care no longer meets Medicare’s skilled criteria, the facility stay can shift from “covered skilled rehab” to “private-pay custodial care.” That moment is often when families realize Medicare is not a long-term nursing home solution and why planning ahead matters.
Medicare Comparison Tool
If you’re comparing Medicare Supplement or Medicare Advantage options to help manage medical costs around hospital and skilled nursing stays, use the comparison tool below. It won’t quote nursing home room and board for long-term custodial care, but it can help you compare plan structures that affect your out-of-pocket exposure during hospitalizations and skilled rehab periods.
Compare Plans & Estimate Costs
Use the calculator, then request guidance to confirm plan type fit for your doctors, prescriptions, and budget—especially if you want clarity around hospitalization and post-hospital rehab coverage.
The Key Answer: Medicare Does Not Cover Long-Term Custodial Nursing Home Care
This is the critical point: Medicare does not cover long-term custodial care in a nursing home when the ongoing need is help with daily activities or supervision. Once you no longer require daily skilled nursing or ongoing rehabilitation, Medicare’s role in a facility stay typically ends—even if the person still needs day-to-day support.
At that point, the “how do we pay for this?” conversation usually becomes about private pay, long-term care insurance benefits if a policy exists, or Medicaid eligibility rules if assets and income eventually fall within program guidelines. The right path depends on household finances, the healthy spouse’s needs, and how much choice the family wants in care settings and providers.
Why a Long-Term Care Plan Matters (Even If You’re Healthy Today)
Long-term care planning is not about assuming you’ll need a nursing home. It’s about acknowledging that many care journeys begin at home, then progress—sometimes slowly—into more consistent support. What starts as help with errands and transportation can turn into hands-on daily care. When that happens, costs become recurring, and the length of time matters as much as the monthly price.
Long-term care insurance is designed to fund custodial care—at home, in assisted living, in memory care, or in a nursing facility—because those services sit outside Medicare’s main purpose. For many families, having a policy is less about “getting a check” and more about protecting options: staying at home longer, reducing caregiver burden, and avoiding a rushed spend-down plan.
Where Long-Term Care Insurance Fits After Medicare’s Skilled Coverage Ends
Some families coordinate coverage intentionally: Medicare helps with short-term skilled rehab after a hospitalization, and a long-term care policy can step in later if the person transitions to custodial care for months or years. This coordination is one reason LTC solutions are often described as “filling the Medicare gap.”
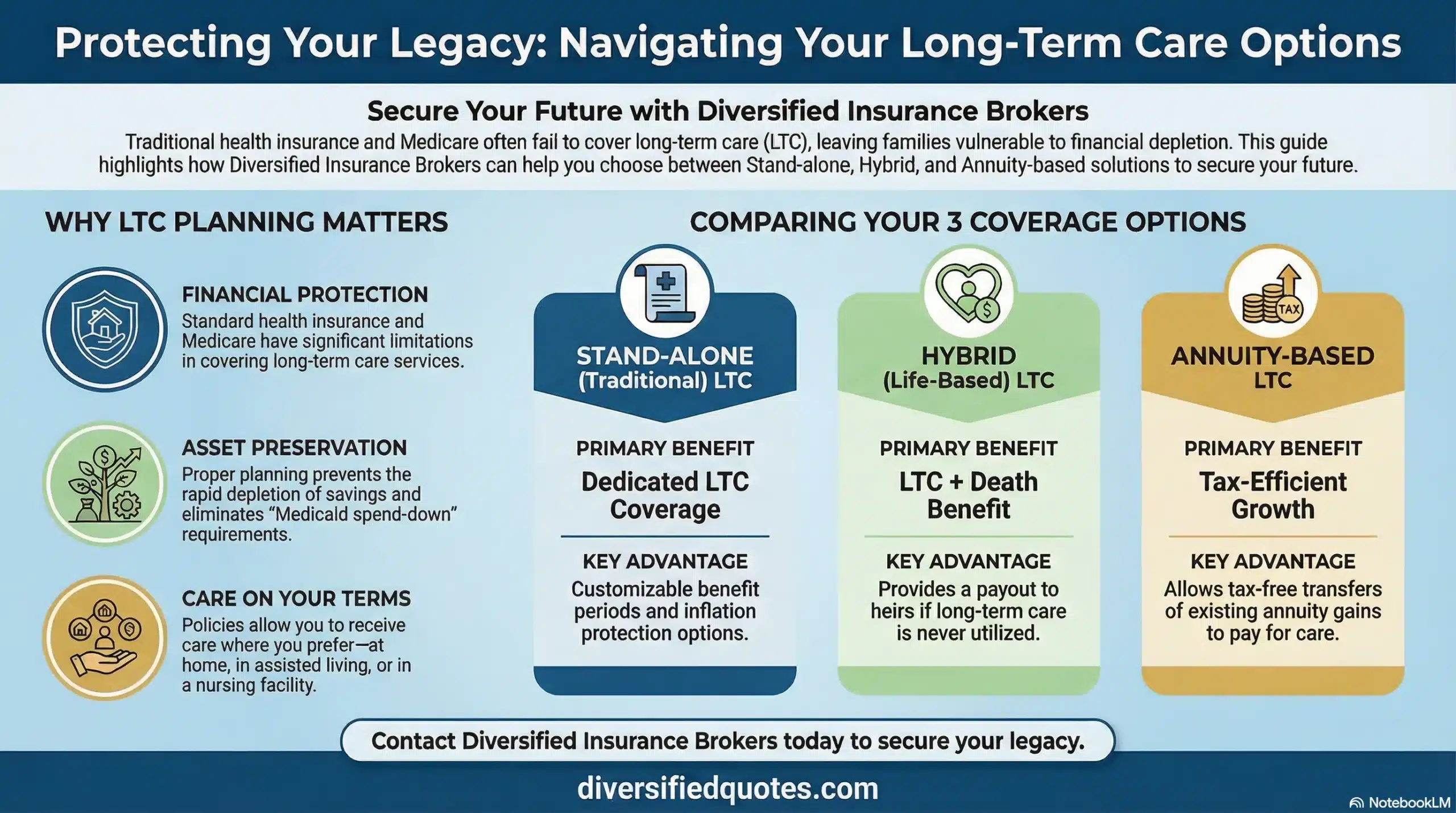
Modern designs can also be more flexible than many people expect. Couples sometimes use shared benefit pools to avoid buying two completely separate benefit stacks. Others prefer hybrid life/LTC designs that preserve a benefit for heirs if care is never needed. If you want to explore these options, we typically compare traditional LTC, hybrid life/LTC, and annuity-based LTC riders side by side so the trade-offs are clear.
Funding Care in a Tax-Smart Way
Once someone understands Medicare’s limitation, the next question is often about efficiency: “If I need long-term care, how do I pay without destroying my retirement plan?” Some people prefer traditional LTC insurance for maximum leverage per premium dollar. Others prefer hybrid designs because they dislike the idea of paying premiums without any value if care is never needed. Still others evaluate annuity-linked LTC riders because they want conservative accumulation with an expanded pool if care occurs.
Tax treatment can vary by design, by funding source, and by how benefits are paid. Educational resources like Tax Benefits of Long-Term Care Insurance help clarify why some households incorporate LTC planning as part of a broader retirement income strategy rather than treating it as a standalone purchase.
What Happens When Medicare Isn’t Enough and There’s No LTC Plan
In real life, families often move through phases: short-term rehab coverage after a hospitalization (when it qualifies), then private pay when care becomes custodial, and eventually Medicaid if assets are spent down far enough. That sequence can be financially and emotionally exhausting, especially when it happens quickly and decisions are made under stress.
Some households look for ways to create a dedicated care funding pool that does not rely on Medicare or a last-minute Medicaid strategy. For example, educational content on non-qualified long-term care annuities can show how certain annuity structures are designed to help fund extended care needs while keeping money available if care is never needed.
How This Fits Into Your Retirement Plan
Ultimately, “Does Medicare cover nursing home care?” is really a retirement-risk question. Medicare is strong for hospital and medical coverage, and it can be helpful for skilled rehab. But it is not a long-term custodial care solution. If you plan for that gap while you’re healthy, you typically have more choices and better pricing options than if you wait until after a health change.
If you want help, the next step is simple: use the Medicare comparison tool above to understand plan structure, then request guidance so we can explain how Medicare interacts with skilled nursing and how to build a long-term care plan around it.
Get a Plan for Nursing Home and Long-Term Care Costs
We’ll clarify what Medicare will pay for, explain the skilled vs. custodial divide, and map out options that can protect your savings if extended care is needed.
Related Pages
Explore these related resources on Medicare costs, long-term care planning, and retirement protection strategies.
Financial Protection Essentials
Chronic condition underwriting, burial insurance solutions, legal funding guidance, and specialized life insurance structures.
Questions now? Call 800-533-5969
FAQs: Does Medicare Cover Nursing Home Care?
Does Medicare pay for long-term nursing home care?
No. Medicare does not pay for long-term custodial care when you primarily need help with daily activities like bathing, dressing, or eating. It focuses on short-term skilled nursing after a qualifying hospital stay.
When does Medicare cover nursing home care?
Medicare may cover nursing home care when you need skilled nursing or rehabilitation services after a qualifying hospital stay, are admitted to a Medicare-certified facility, and your doctor certifies that you need daily skilled care.
What is the difference between skilled nursing and custodial care?
Skilled nursing involves medical care provided or supervised by licensed professionals, such as nurses and therapists. Custodial care focuses on non-medical help with daily activities and is not covered by Medicare long term.
Does Medicare cover assisted living or memory care?
Generally no. Medicare does not pay for room, board, or personal care in assisted living or memory care facilities. It may cover certain medical services provided there, but not the ongoing custodial care itself.
Will Medicare cover my entire nursing home bill after a hospital stay?
No. Even when requirements are met, Medicare covers only a limited number of days in a skilled nursing facility and may require copayments. After that, you are responsible for the full cost unless other coverage applies.
How can I pay for nursing home care when Medicare stops?
Options include long-term care insurance, certain annuity strategies, personal savings, and Medicaid if you meet eligibility rules. Planning early can help reduce the risk of spending down your assets unexpectedly.
Is long-term care insurance necessary if I have Medicare?
For many people, yes. Long-term care insurance is designed to cover extended custodial care in nursing homes, assisted living, or at home—services that Medicare generally does not cover on a long-term basis.
When should I start planning for nursing home and long-term care costs?
It is best to start planning in your 50s or early 60s, while you are still healthy enough to qualify for coverage and have time to integrate long-term care planning into your overall retirement strategy.
About the Author:
Tonia Pettitt, CMIP©, is a seasoned Medicare specialist with more than 40 years of hands-on experience guiding individuals and families through the complexities of Medicare planning. As a senior advisor with the nationally licensed independent agency Diversified Insurance Brokers, Tonia provides clear, dependable guidance across all areas of Medicare—including Medicare Advantage, Medicare Supplement (Medigap), and Part D prescription coverage. Leveraging active contracts with dozens of highly rated insurance carriers, she helps clients compare options objectively and secure the most suitable coverage for their health and budget.
Known for her patient, education-first approach, Tonia has built a reputation as a trusted resource for retirees seeking reliable, unbiased Medicare support. With four decades of experience across evolving Medicare laws, carrier changes, and plan structures, she brings unmatched insight to every client conversation—ensuring clients feel confident, protected, and fully prepared for each stage of their retirement healthcare journey.
Explore More Medicare Options: Browse our complete guide to How Does Medicare Work? — covering Medicare Parts A, B, C & D explained — coverage, costs & how it all fits together.
