ACA Subsidies Expired: What Alternatives are Available

Jason Stolz CLTC, CRPC
ACA subsidies expired: what alternatives are available is a question that shows up when the monthly premium jumps and the math suddenly stops working. For many households, that shift feels immediate: the plan may be the same plan, the deductible may still be high, and the network may still feel narrow, but the price becomes dramatically less forgiving. For many employers, the same pressure shows up in a different way. Employees begin asking for help. Owners begin questioning whether it still makes sense for the company to rely on individual coverage strategies. And leadership starts looking for a path that is more stable, more controllable, and easier to plan around than year-to-year marketplace volatility.
While headlines often focus on the individual market, the most practical alternatives after subsidies end are frequently group health alternatives. That does not mean abandoning compliant coverage. It means shifting into an employer-sponsored structure that gives the company more control over plan design, more predictability in budgeting, and—depending on the strategy—more transparency into what is driving costs. In other words, when the subsidy goes away, many employers and business owners stop thinking in terms of “shopping for a plan” and start thinking in terms of “building a sustainable benefits strategy.”
At Diversified Insurance Brokers, we help employers nationwide evaluate group health options that can replace or outperform unsubsidized ACA coverage once subsidies are no longer available. For some companies, the best move is a traditional fully insured group plan. For others, the best move is a level-funded or partially self-funded model that preserves the group structure while improving cost visibility. The goal is not complexity for the sake of complexity. The goal is giving the employer a framework that can hold up over time—especially when the company is tired of surprise increases and limited plan flexibility.
This page breaks down the real alternatives that exist when ACA subsidies expire, why group health becomes more attractive in many situations, how self-funded and level-funded plans work as employer strategies, how eligibility and participation requirements typically function, and how to plan a transition that employees understand and value.
Explore Group Health Alternatives After ACA Subsidies Expire
If premiums increased after subsidies ended, compare unsubsidized ACA costs against group health options built for stability.
Why ACA Subsidy Expiration Changes the Math
ACA subsidies were designed to soften the cost of individual marketplace coverage. When those subsidies are no longer applied, the premium that a household sees each month can snap back to the plan’s full unsubsidized cost. Many people assume that if a plan is “standardized,” the price should feel predictable. In reality, the individual market can be extremely sensitive to rating changes, regional competition, carrier participation, and year-to-year pricing adjustments. When the subsidy support disappears, those changes become much harder to absorb because there is no longer a meaningful cushion between the sticker price and what the household pays.
Another frustration is that subsidy expiration often does not bring better benefits. Deductibles can remain high. Coinsurance can remain high. Out-of-pocket maximums can still feel heavy. Network rules can still be restrictive. So the experience becomes emotionally discouraging: the price rises, but the plan still feels like a plan designed for cost containment rather than employee or family convenience.
For employers and business owners, the equation changes in a different way. Leadership begins to notice that individual coverage is not a stable foundation for a workforce benefit strategy. When employees rely on the individual market, the company’s ability to plan is limited. The company cannot easily influence plan design. The company cannot easily create consistent benefit value across the team. And the company cannot easily turn healthcare into a predictable compensation component. That is why, in many cases, subsidy expiration triggers a move toward group coverage—not because group coverage is trendy, but because group coverage can be structured as a long-term business decision rather than a yearly household shopping exercise.
What “Alternatives” Really Means After Subsidies End
When someone asks, ACA subsidies expired: what alternatives are available, it can sound like they are searching for a completely different kind of coverage. In practice, the best alternatives are often not “replacement” products. They are different structures for delivering legitimate healthcare coverage in a way that is more stable and more controllable.
For many working families, the strongest alternative is becoming eligible for employer-sponsored group coverage or joining a company plan where the employer contributes to premiums. For business owners, the alternative may be creating a group plan where none existed before. For growing companies, the alternative may be changing the way the current group plan is funded and managed so renewals become less punishing and more understandable.
This is where group health becomes the center of the conversation. Group health can be structured traditionally, or it can be structured with modern funding models. The important point is that these are still group health strategies. They are not a downgrade. They are a different way to fund and manage healthcare costs with an emphasis on sustainability.
Why Group Health Insurance Becomes More Attractive After Subsidies Expire
Group health insurance is not priced the same way as individual marketplace coverage. The group market focuses on the employer’s census, participation rules, plan design, and—depending on the structure—claims trends. In a fully insured model, the employer pays a premium to the carrier and the carrier assumes claim risk. In more advanced models, the employer can participate differently in risk sharing while still using professional administration and risk protection layers.
Once subsidies expire and individuals face full marketplace pricing, a group plan can become more competitive for two reasons. First, the employer can contribute. That alone can change affordability immediately. Second, the group plan may provide better value: broader networks, more consistent benefit structures, and plan designs that are not as constrained by marketplace plan menus.
For employers, group health also becomes a strategic tool. If the company can provide a benefit that helps employees stabilize a major household expense at the same time subsidies disappear, the benefit feels more valuable than ever. That can support retention, recruiting, and company culture. It also gives leadership a more predictable framework for budgeting benefits and adjusting compensation in a measured way.
If you want a broader overview of employer plan structures, you can start with Group Medical Insurance and how group strategies differ from individual coverage models.
Traditional Group Health vs ACA Marketplace Coverage
ACA marketplace coverage is designed to be accessible. It also tends to be standardized in ways that limit customization. That standardization can be helpful, but it also means many households feel like they are selecting from a narrow set of options that do not match their preferences. When premiums are subsidized, those limitations can be tolerable. When premiums are no longer subsidized, those limitations often feel unacceptable.
Group health, by contrast, can give the employer more influence over plan design. The employer can select networks that match the workforce’s location and provider preferences. The employer can decide how much premium contribution to provide. The employer can choose between plan designs that balance deductible levels, copays, and out-of-pocket exposure. The employer can build a benefit structure that aligns with the company’s compensation philosophy rather than forcing employees to solve healthcare on their own.
Another difference is how employers can manage renewals. In the individual market, the household is mostly reactive. In group health, the employer can evaluate funding models, implement cost-management strategies, and adjust plan design intentionally. That does not remove medical inflation, but it does give the company more tools to plan and respond.
When an Employer Should Re-Evaluate Group Health
Subsidy expiration is often the trigger, but companies usually make the shift when the company starts to feel “big enough” that relying on the individual market no longer makes sense. That threshold can be lower than many owners expect. Some employers begin evaluating group options with only a handful of eligible employees, depending on state rules, carrier guidelines, and company structure.
A helpful reference point is eligibility requirements. Reviewing Minimum Employees for Group Health Insurance can clarify when group options typically become realistic and what participation and contribution requirements often look like.
Compare Unsubsidized ACA Costs vs Group Health
We’ll compare the real monthly cost of coverage after subsidies ended with group health options designed for predictability.
Self-Funded and Level-Funded Group Health as Practical Alternatives
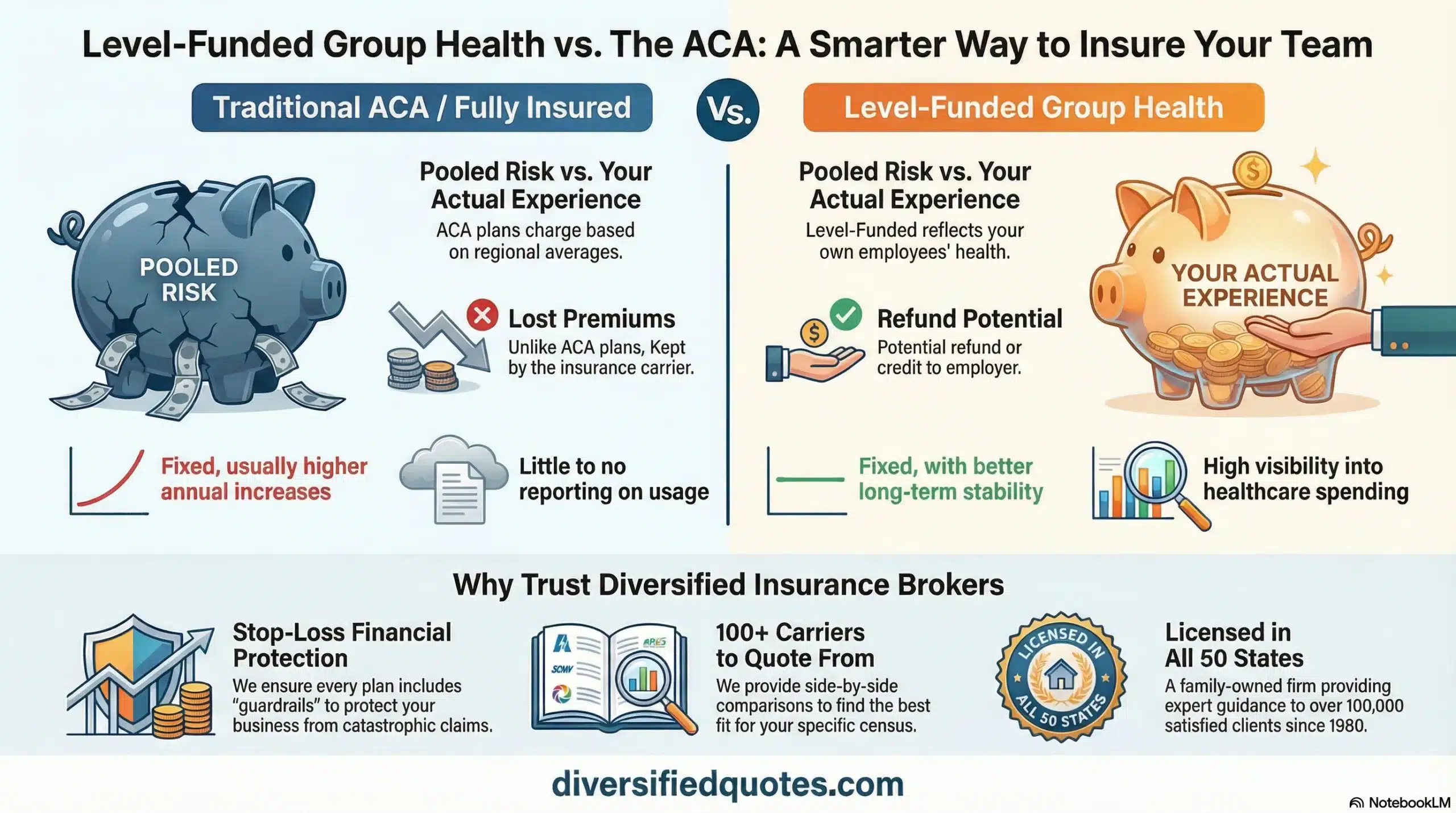
Once employers decide that a group plan makes sense, the next question becomes how to structure it. Many employers assume the only option is a traditional fully insured group plan. Fully insured plans can absolutely be the right solution, particularly for employers who want maximum simplicity. But for many businesses, the biggest frustration is that fully insured renewals can still feel opaque and unpredictable. That is why many employers explore self-funded and level-funded strategies as an alternative to traditional fully insured ACA group plans.
Self-funded and level-funded group plans are still group health plans. They are not a way to avoid legitimate coverage. The difference is how the plan is funded and how claims risk is managed. Instead of paying a single bundled premium that includes claims risk pricing, administration, and carrier margin, the employer funds claims more directly while layering in professional administration and risk protection. Over time, this structure can provide more transparency and a more strategic framework for managing cost trends.
If you want the foundational explanation of self-funding, start with What Is Self-Funded Group Health Insurance?. That breakdown helps employers understand the core difference between paying a carrier premium and funding claims with protection layers.
How Level-Funded Plans Fit Employers Who Want Predictability
Many companies want the strategic advantages of self-funding but prefer predictable monthly payments. Level-funded plans are often built for that. In a level-funded structure, the employer pays a fixed monthly amount, but the amount is typically allocated into administrative cost, stop-loss cost, and a claims funding component. Claims are paid out of a designated claims account. If claims run below projections, the employer may receive a refund or a credit depending on plan design and contract provisions.
This structure can feel like a middle ground: the employer gains improved transparency and potential upside, while the employer still has guardrails that limit volatility. That is why level funding is frequently one of the most practical alternatives after subsidies expire, particularly for employers that are large enough to meet participation requirements but still small enough to want stability.
Many employers also want to understand risk protection before they move forward. Stop-loss is a major component of level funding. It is the layer that caps exposure so the employer is not taking unlimited risk.
How Stop-Loss Insurance Protects Employers in Alternative Funding Models
Stop-loss protection is what makes self-funded and level-funded plans feasible for most employers. It limits exposure from high-cost claims and caps aggregate claim risk. While stop-loss terms vary, the goal is consistent: build a funding structure that allows the employer to benefit from favorable claims experience while not being financially derailed by catastrophic events.
Stop-loss should not be treated as an afterthought. Contract definitions, attachment points, renewal provisions, and coverage structures matter. Employers transitioning out of a fully insured plan should understand stop-loss mechanics clearly before making a decision. For a deeper explanation, review Pros and Cons of Self-Funded Group Health, which frames the decision around transparency, risk control, and long-term plan management.
Why Employers Often Prefer Group Strategies After Subsidies End
Subsidy expiration creates a psychological shift. When employees are paying full marketplace prices, they often feel exposed. They may skip care. They may delay treatment. They may feel frustrated about healthcare as a household budget line item. When an employer introduces a structured group plan, the benefit can feel like relief. Even when employees contribute, the plan is often perceived as more stable and more valuable because it is part of a broader compensation strategy rather than an individual shopping task.
Employers also often find that group strategies make budgeting easier. Instead of reacting to marketplace pricing changes that employees face individually, the employer can build a consistent approach: decide contribution levels, choose plan structures, and communicate changes clearly once per year on the company’s terms.
Cost Control vs Cost Shifting
When premiums rise after subsidies expire, it is easy for employers to assume that “the solution” is simply to push costs somewhere else. That approach usually backfires. Employees feel the change immediately, morale drops, and turnover risk increases. The stronger approach is cost control. Cost control is about building a plan structure that reduces unnecessary friction, improves transparency, and gives the employer tools to influence long-term trends.
In a group environment, cost control can come from smarter plan design, better vendor alignment, and more consistent employee education about how to use benefits effectively. The point is not to make healthcare harder to access. The point is to make the plan sustainable so the employer can keep offering it year after year without constant crisis.
How to Plan a Transition from Individual Coverage to Group Coverage
One of the biggest mistakes employers make is treating a transition as a last-minute scramble. A strong transition plan starts with understanding timing, eligibility, and employee expectations. Employers need to align effective dates, coordinate enrollment windows, and decide how much the company will contribute. Employees need a clear explanation of what is changing and why. Employees also need reassurance that the new plan is not a downgrade, and they need time to evaluate networks and plan design.
When done properly, the transition can improve satisfaction. Employees often value the stability and structure of group benefits, especially after experiencing premium shock in the individual market. The employer benefits by building a benefit framework that is easier to manage and more aligned with recruiting and retention goals.
If your company is focused on controlling spend and building a long-term approach, it can be helpful to review group health insurance cost strategies and how employers typically approach long-term budgeting decisions in a group environment.
How Diversified Insurance Brokers Helps Employers Navigate the Shift
Our role is to help employers evaluate alternatives with clarity rather than hype. That means comparing the real cost of unsubsidized individual coverage against group options and showing the employer what changes in plan design, funding model, and cost stability when a business moves into an employer-sponsored strategy.
We help employers confirm eligibility and participation requirements, compare plan structures, and evaluate whether a fully insured option or a level-funded strategy fits better. We also help employers understand what “predictability” actually means in different models, because predictability can come from a fixed premium in a fully insured plan or from a structured funding approach with stop-loss protection in a partially self-funded plan.
Most importantly, we help employers build a plan that employees can understand and value. When employees understand why the plan exists and how it supports them, the plan becomes an asset for retention and recruiting rather than a constant source of confusion.
Build a Long-Term Strategy After ACA Subsidies Expire
If your household or workforce was impacted by subsidy expiration, we’ll map the most practical group health options forward.
Related Group Health Pages
Continue exploring employer coverage strategies and funding models that may improve stability after subsidy changes.
Financial Protection Essentials
Chronic condition underwriting guidance, dental and vision options, financial firm reviews, and state-level consumer protections.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
FAQ for ACA Subsidies Expired: What Alternatives Are Available
What does it mean that ACA subsidies expired?
It means premium tax credits are no longer reducing the cost of ACA marketplace plans, exposing enrollees to full, unsubsidized premiums. Many consumers begin exploring alternatives like small employer group health insurance when subsidy support ends.
Why are ACA premiums increasing after subsidies expire?
Without subsidies, consumers must pay the full cost of coverage, which reflects rising healthcare expenses and insurer pricing. Some individuals compare these increases against short-term health insurance options to evaluate cost differences.
Is group health insurance an alternative to ACA plans?
Yes. Group health insurance is often a strong alternative, particularly for employers and businesses with eligible employees. Employers may evaluate self-funded group health structures as a way to control costs while maintaining coverage.
Can small businesses qualify for group health insurance?
Yes. Many small businesses qualify depending on employee count, participation, and contribution requirements. Even very small companies can explore options such as 2-person group health insurance if eligibility criteria are met.
Does group health insurance cost less than unsubsidized ACA plans?
In many cases, yes. Group health insurance can be more cost-effective once ACA subsidies expire, especially when compared against fully rated individual plans. Reviewing structural differences in fully insured vs. self-funded health plans can clarify long-term cost expectations.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers, is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient.
