Small Business Group Health Insurance

Jason Stolz CLTC, CRPC
Small business group health insurance helps employers with 2–50 employees offer professional-grade medical coverage while keeping costs predictable and benefits competitive. For many owners, the decision is not about “checking a box.” It’s about recruiting and retaining great employees, improving stability, and protecting your team’s financial well-being when medical needs arise. A structured group plan can also create meaningful tax advantages, and it often provides stronger network access and plan value than many individual options—especially for teams that want consistent, long-term coverage.
The challenge is that small group health plans don’t come in a single format. You can choose a traditional fully insured plan, explore hybrid approaches like level-funded arrangements, or even evaluate a self-funded path for groups that want maximum transparency and control. The best choice depends on your headcount, budget, participation strength, how stable your employee roster is, and how much renewal volatility your business can tolerate year to year.
If you’re in the earliest research stage, two foundational resources help clarify the rules quickly. Start with 2-Person Group Health Insurance if you’re an owner-and-one team (or you’re right on the edge of eligibility). Then review Minimum Employees for Group Health Insurance to understand the most common qualification standards, documentation expectations, and exceptions that can impact quoting.
Below, we walk through how small business group health insurance works, the funding models worth considering, how eligibility and participation affect pricing, and how to build a plan that employees actually use—without creating an administrative burden. Throughout the page, Diversified Insurance Brokers focuses on the practical decisions that drive real-world outcomes: true cost, renewal stability, employee satisfaction, and compliance simplicity.
Compare Small Business Health Plans
See how small group plans can improve retention, strengthen coverage, and create a predictable monthly budget for your business.
How Small Business Group Health Insurance Works
When your business offers group health insurance, you are setting up a single employer-sponsored plan that covers eligible employees and—if you choose—eligible dependents. The employer typically pays a portion of the premium, and employees contribute the rest through payroll deductions. That shared structure spreads risk across the group and can make coverage more affordable and consistent than individual policies, especially when employees value stable networks and predictable benefits.
From an employee’s perspective, group coverage often feels simpler because enrollment is tied to hiring and annual renewal cycles. From an employer’s perspective, the plan is an ongoing business decision with predictable monthly billing, renewal pricing that must be evaluated each year, and compliance responsibilities such as eligibility definitions, waiting periods, and required notices. A strong plan does not just “exist.” It is designed to be understood, used, and renewed without shock.
Most carriers define small groups as businesses with 2–50 employees, but the practical question is not just headcount. It is eligibility. Carriers typically want bona fide W-2 employees, and they often require minimum employer contributions and a minimum participation rate. If you are a micro-group, eligibility nuances matter more than anything else. For example, an owner-and-one scenario can be workable when documentation and payroll structure are clean, but it can become difficult if the group is unstable or if the plan does not meet underwriting rules. That is why micro-groups should start with group health insurance for a 2-person business if you want a direct “what works in real life” walkthrough.
Funding Models to Consider for Small Business Plans
Small business group health insurance is not one product. It is a category that includes multiple funding models. Choosing the right funding model is one of the most important decisions you will make because it affects not only your initial rate, but how renewals behave, how much transparency you get into claims, and whether you have pathways to long-term cost control. In practice, small employers typically evaluate three core approaches: fully insured, level-funded, and self-funded.
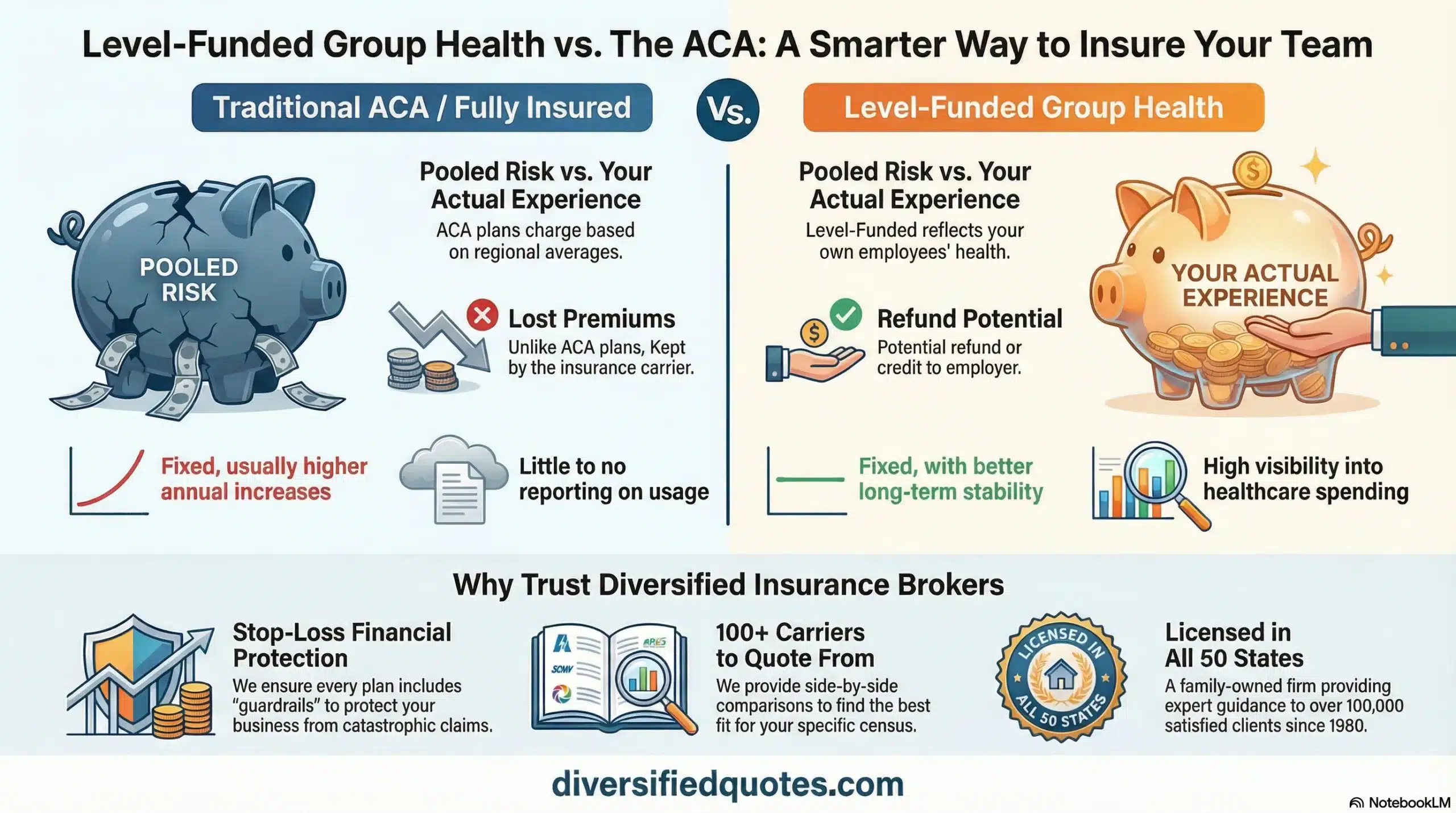
Fully insured plans are the traditional approach. You pay a fixed monthly premium, the carrier assumes the claims risk, and your cost is mostly determined by the carrier’s underwriting and renewal formula. Fully insured can be an excellent fit when simplicity is your top priority and you do not want any exposure to claim volatility. The tradeoff is that the structure typically includes carrier margin, premium taxes, and less transparency into what is driving long-term pricing.
Level-funded plans are a hybrid designed specifically to make alternative funding realistic for smaller groups. In a level-funded arrangement, you pay a predictable monthly amount that generally includes estimated claims funding, fixed administrative costs, and stop-loss protection. If claims run lower than expected, many level-funded plans can return a portion of unused claims funding based on contract terms. If claims run higher than expected, stop-loss coverage helps protect the plan from catastrophic exposure. For employers who want budget stability but still want a pathway to improved economics, level-funded is often a compelling middle lane. If you want the “why it works” overview, review why group level funding can make sense.
Self-funded plans place the employer in a more direct funding role. The employer pays claims as they occur and uses stop-loss insurance to cap major risk exposure. Self-funding can deliver strong transparency and customization, but it requires good governance, consistent cash flow, and a willingness to manage the plan as an ongoing financial system rather than a passive premium purchase. If you want the clearest foundation on this lane, start with what is self-funded group health insurance.
The “best” funding model is the one that fits your business reality. If your team is stable and your budget can handle a structured renewal process, a level-funded or self-funded option may provide better long-term control. If your group is brand new, or if participation is uncertain, a fully insured plan can provide a clean starting point while you build stability and documentation strength.
Why Stop-Loss Matters (Especially for Level-Funded and Self-Funded Plans)
Stop-loss insurance is the protection layer that makes alternative funding practical for small employers. Without stop-loss, a single high-cost claim could create unacceptable volatility for a small group. With stop-loss in place, the plan can limit exposure above defined thresholds and create a more stable financial outcome across the plan year. This is why many level-funded proposals look “simple” on the surface—fixed monthly payments—but are powered by stop-loss mechanics underneath.
For employers evaluating level-funded designs, understanding stop-loss terms helps you compare proposals correctly. Items like specific thresholds, aggregate protections, and contract basis can change the true risk profile and the total cost. If you want a plain-English breakdown of the most common terms and how they impact underwriting, see understanding stop-loss insurance in level-funded plans.
In practical terms, the goal is not to “buy the lowest stop-loss premium.” The goal is to align stop-loss structure with your risk tolerance, headcount, cash flow, and expected volatility. A well-designed stop-loss layer stabilizes your plan year and makes renewal decisions clearer because you can see which changes are driven by claims and which are driven by market pricing.
Eligibility and Participation Rules That Drive Pricing
Most small group health plans are underwritten based on eligibility and participation rules, and these rules influence both whether you can be quoted and what the final pricing looks like. Carriers typically want eligible W-2 employees, consistent payroll, and a stable definition of who is “benefits eligible.” The most common scenario is straightforward: you define full-time status (often 30 hours per week), set a waiting period if desired, and offer coverage to eligible employees.
Participation matters because carriers do not want a plan where only employees who expect high claims enroll. That is why many carriers require a minimum participation percentage among eligible employees. Employer contributions also matter because they affect participation. Many small employers choose a contribution strategy that is strong enough to encourage consistent enrollment but still predictable for budgeting.
Micro-groups require extra attention because one person’s decision can change participation dramatically. If you are very small, the most helpful step is to confirm your baseline eligibility first. Use minimum employees for group health insurance to validate the most common group definitions, and then use 2-person group health insurance if you are right at the smallest end of the market.
Workforce mix can also complicate eligibility. Contractors are a common point of confusion. In most cases, true 1099 contractors do not belong inside the group medical plan because carriers underwrite based on employee eligibility. If your workforce includes contractors and you want to stay compliant while still supporting them thoughtfully, review can 1099s get group level funding for an employer-friendly explanation of what is realistic without jeopardizing underwriting.
Plan Design: What to Compare Beyond the Monthly Premium
Many small businesses start by looking at the monthly premium. That is understandable, but it is not enough. Two plans can have similar premiums and deliver completely different employee experiences depending on network access, deductible structure, copays, coinsurance, and prescription coverage. A plan that employees can afford to use often has a bigger impact on retention and morale than a plan that simply has a lower sticker price.
Network strength is one of the biggest practical differentiators. Employees care about whether their doctors and preferred hospitals are in-network. If you have a mixed workforce across multiple ZIP codes, network decisions become even more important. A plan that looks excellent in one region can become frustrating if remote employees are pushed out-of-network for routine care. Aligning networks with where employees actually live is one of the highest-leverage improvements small employers can make.
Deductible strategy is another major driver. High-deductible health plans (HDHPs) paired with HSAs can be a strong fit for employers who want a lower premium and employees who are comfortable with more upfront cost in exchange for tax-advantaged savings. However, an HDHP can be a poor fit if your team expects frequent care and will struggle with out-of-pocket exposure. Many employers solve this by offering two plan options: one lower premium / higher deductible choice and one richer plan for employees who prefer lower point-of-care cost.
Prescription coverage and pharmacy design can quietly drive the real-world value of a plan. Formularies, tiering, specialty drug handling, and mail-order expectations can all affect employee out-of-pocket costs and satisfaction. Even in smaller groups, pharmacy utilization can influence renewals, especially if specialty medications are in play. A good plan design discussion includes pharmacy realities, not just medical deductibles.
Finally, a plan must be understandable. Employee confusion creates HR burden. Clear plan explanations, simple comparisons, and a consistent onboarding process reduce questions and improve satisfaction, especially during the first 60–90 days after implementation.
Tax Benefits and the True Cost of Coverage
Small business group health insurance often provides meaningful tax efficiency. In many cases, employer-paid premiums are deductible as a business expense, and employee contributions can often be structured pre-tax depending on the plan setup and employer approach. These factors can reduce the net cost of coverage compared to an individual plan strategy, especially when the employer is trying to balance competitiveness with budget control.
Level-funded structures can introduce additional planning considerations because the monthly amount typically combines multiple components: expected claims funding, fixed administration, and stop-loss. Understanding how these pieces work together helps employers compare proposals correctly. A practical reference for the employer side of this comparison is level-funded health insurance tax benefits explained, which is helpful when you want to evaluate the “all-in” cost rather than just the headline number.
One of the biggest mistakes small employers make is comparing two plans that are not truly comparable. For example, two proposals may have different networks, different plan designs, or different stop-loss structure. The best way to compare is to define your plan requirements first—network, plan richness, contribution approach—then compare funding options within those constraints so your decision is based on real differences rather than hidden mismatches.
How to Manage Costs and Renewals Without Destroying Benefits
Health insurance costs tend to rise over time, and renewals can feel unpredictable—especially for smaller groups where even a modest claims change can influence pricing. The goal is not to chase the cheapest option every year. The goal is to build a strategy that remains sustainable and competitive while still protecting your budget. Employers who approach renewals with a plan tend to get better results than employers who treat renewals as a last-minute emergency.
One high-impact method is to offer plan choice. When employees have two plan options—often one richer plan and one leaner plan—you can control employer contributions while giving employees flexibility. Another method is to improve how employees access care by encouraging preventive care and telehealth where appropriate. These are not “magic bullets,” but over time they can improve claims patterns and reduce disruption.
Another important lever is funding model selection at renewal. Employers who are tired of renewal spikes in fully insured plans often explore level-funded options because those models can provide more transparency and, in favorable years, surplus return potential. If your goal is to understand whether a level-funded design is realistic for your size, revisit why group level funding can make sense and then explore how stop-loss terms affect the risk profile using understanding stop-loss insurance in level-funded plans.
If your team is very small, some level-funded models include provisions that can create refunds when claims are favorable. That is not guaranteed, and it depends on contract terms, but it can be a meaningful advantage when you want predictable monthly budgeting with an upside pathway. If that concept is central to your decision, review can small groups get health insurance refunds for a clearer explanation of what employers should expect and what factors influence outcomes.
Model Fully Insured vs Level-Funded Side by Side
We’ll align networks and plan designs first, then compare funding models so you can see true cost and renewal behavior.
Request a Side-by-Side ComparisonComparison of Group Health Funding Models
This table is a quick reference, but keep in mind that real-world results depend on plan design, network, workforce stability, and stop-loss structure. Use it as a starting point to understand what you are “buying” in each lane.
| Funding Model | Predictability | Employer Risk | Refund Potential |
|---|---|---|---|
| Fully-Insured | High — fixed monthly premiums | Low | None |
| Level-Funded | High — fixed payments with guardrails | Medium (capped with stop-loss) | Possible if claims are favorable |
| Self-Funded | Variable — claims-driven | Higher (offset by stop-loss) | Yes (claims savings stay with employer) |
Implementation, Enrollment, and Ongoing Administration
Small business group health insurance is easier when implementation is structured. Most employers benefit from a clean timeline: confirm eligibility rules, finalize plan selection, schedule enrollment, and ensure employees understand what is changing and how to use their benefits. A smooth implementation reduces confusion and prevents late enrollment issues that can create administrative problems or carrier disputes.
Ongoing administration matters, too. Employers often need help with new hires, terminations, qualifying events, and renewal preparation. The right approach reduces the “constant questions” problem and helps employees feel confident using their coverage. This is also where clarity around eligibility definitions becomes important, especially if your business has variable hours, seasonal staffing, or a mix of employee classes.
If you want a straightforward “employer question” resource that mirrors what owners actually ask during quoting and implementation, review top questions employers ask about group health insurance. It complements this guide well and helps employers avoid the most common misunderstandings that delay underwriting or create confusion during onboarding.
How to Choose the Right Strategy for Your Business
The best small business group health insurance plan is not “the cheapest plan.” It is the plan that your employees can actually use, that your budget can sustain, and that renews without constant surprises. That outcome comes from making decisions in the right order: confirm eligibility and participation strategy, choose the funding lane that matches risk tolerance, compare plan design and networks inside that lane, then implement with clear communication so employees understand what they have and how to use it.
If your business is small and still stabilizing, a traditional fully insured plan can be a clean starting point. If you are frustrated with renewals and want a pathway to more transparency and potentially better economics, level-funded designs can be a strong middle lane. If you want maximum control and visibility and you have the governance and cash flow structure to manage it, a self-funded approach can be part of a longer-term benefits strategy. You do not have to guess—employers often do best when they compare two or three realistic options side by side and choose the one that matches the business reality.
Request Small Business Group Health Quotes
Share basic details and we’ll return curated options with clear explanations and clean comparisons.
Related Group Health Resources
Explore eligibility rules, funding models, stop-loss mechanics, and small-employer strategies to help you choose the right plan lane.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
FAQs: Small Business Group Health Insurance
Do small businesses have to offer health insurance?
No, businesses with fewer than 50 full-time equivalent employees are not required by federal law to offer health insurance. Many still choose to offer it for recruiting and tax reasons. See Small Business Health Care Tax Credit & SHOP.
What is the funding model difference?
You can choose fully-insured (fixed premium), level-funded (fixed premium with possible surplus refund), or self-funded (you assume claims risk and use stop-loss). Compare models under Level-Funded Health Insurance Tax Benefits Explained.
How can small employers control premiums?
Strategies include offering HDHP + HSA, wellness programs, tiered networks, adjusting employer/employee share, and moving to level-funded for refund potential. See related insights under Small Employer Group Health Insurance.
What’s the minimum number of employees?
Many carriers require at least two eligible employees (not married) to form a group. For full detail, read Minimum Employees for Group Health Insurance.
Can I subsidize premiums for employees?
Yes—employers commonly pay a portion of premiums while employees pay the rest. Subsidiation helps with tax advantages and recruiting value.
Are there tax credits available?
Yes. Eligible small employers (fewer than 25 FTEs & average wages under a threshold) who offer a qualified plan may claim the Small Business Health Care Tax Credit.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers (NPN 20471358), is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, Group Health, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient. Visitors who want to explore current annuity rates and compare options across multiple insurers can also use this annuity quote and comparison tool.
