Does Medicare Cover Long Term Care

Does Medicare cover long-term care? It’s one of the biggest misconceptions in retirement planning—and one that often catches families off guard when health begins to decline. While Medicare provides essential hospital and medical coverage, it does not pay for most long-term care services such as assisted living, home health aides, or custodial care. Understanding where Medicare stops and where long-term care insurance begins can be the difference between protecting your retirement savings and spending them down prematurely.
Get Clarity on Medicare vs. Long-Term Care
We’ll explain what Medicare pays for, what it doesn’t, and how to protect your savings from extended care costs.
Check Your LTC Coverage Options
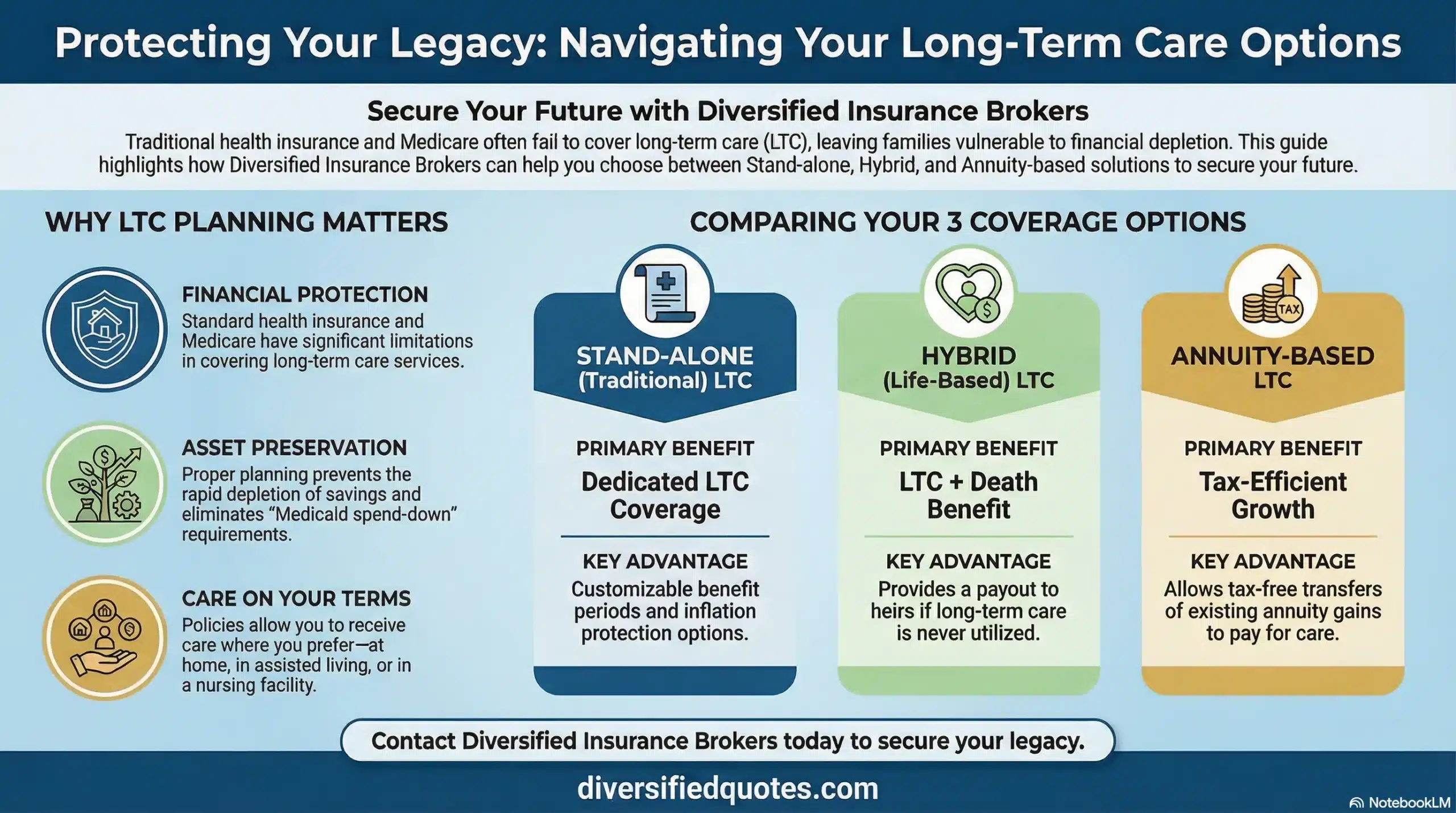
We’ll compare traditional LTC, hybrid life/LTC, and annuity-based LTC riders—and show how they coordinate with Medicare.
Prefer to talk? Call 800-533-5969
What Medicare Actually Covers—and What It Doesn’t
Medicare was designed to cover acute medical needs, not chronic, long-term assistance. Original Medicare (Parts A & B) covers hospital stays, physician visits, preventive care, skilled nursing following hospitalization, and hospice. But long-term care coverage is extremely limited. In many cases, Medicare pays up to 100 days in a skilled nursing facility—only after a qualifying three-day hospital stay and only while skilled treatment is still required. When rehab ends, coverage stops.
When a loved one needs ongoing help with everyday tasks—bathing, eating, dressing, or moving around—also known as Activities of Daily Living (ADLs), Medicare generally doesn’t pay. These non-medical needs are custodial care and fall outside Medicare’s mandate.
Why the Medicare Confusion Persists
Confusion often stems from the brief overlap between post-hospital recovery and true long-term care. After, say, hip surgery, Medicare may cover a short rehab stay. But once therapy ends and help is still needed with meals or dressing, the bills become private-pay. With nursing homes often costing $9,000–$12,000 per month and assisted living $6,000+ in many areas, families can be forced to spend down assets quickly if there’s no plan in place.
Another reason people assume Medicare covers long-term care is language. Terms like “skilled nursing facility,” “home health,” and “nursing home” sound similar, but they mean very different things in Medicare rules. Medicare’s help is tied to medical necessity and measurable improvement. Long-term care, on the other hand, is often about ongoing supervision and hands-on help that may last for months or years. When families plan around the wrong assumption, they usually discover the gap at the worst possible moment—during a hospital discharge or an urgent care transition.
A practical way to avoid confusion is to separate two questions: “Does the person need medical rehab?” and “Does the person need daily help?” Medicare is built around the first. Long-term care planning is built around the second.
Skilled Nursing vs. Custodial Care: The Key Medicare Divider
Medicare’s nursing facility coverage is not triggered by the need for supervision or daily assistance. It is triggered by the need for skilled services that require licensed medical staff—such as IV therapy, complex wound care, certain injections, or intensive physical, occupational, or speech therapy. Even then, the skilled services must be medically necessary and provided on a schedule consistent with Medicare requirements.
Custodial care is different. Custodial care is support with ADLs and basic supervision for safety. Someone may be mentally sharp but physically limited. Someone else may be physically capable but unable to manage medications, cooking, or safety due to cognitive decline. In both situations, families often need consistent help. That is the type of care Medicare generally does not pay for, even when it happens inside a nursing home.
Does Medicare Pay for a Nursing Home After a Hospital Stay?
Medicare can pay for a limited skilled nursing facility stay after hospitalization, but it must follow a specific path. In general, Medicare expects a qualifying inpatient hospital admission and then a timely admission to a Medicare-certified facility for skilled care related to the hospital condition. The goal is rehabilitation and stabilization—not long-term residency.
Even when everything is done correctly, families often encounter a “cliff” moment: Medicare pays while skilled therapy is active, then stops once the person plateaus or no longer needs daily skilled services. The person may still need help getting dressed, walking safely, or using the bathroom—but Medicare can still stop coverage because those needs are custodial.
If you are navigating a discharge, it helps to ask the facility a direct question: “What is the skilled service being provided, and what will change the moment that service is no longer medically necessary?” That one question often clarifies whether you are in a short-term rehab situation or entering a long-term custodial situation that needs a separate funding plan.
Medicare Advantage and Long-Term Care: Helpful, But Not the Same
Some Medicare Advantage plans include limited in-home support benefits or care coordination that can be valuable—especially for members dealing with chronic conditions. Those extras can reduce friction in the system and sometimes provide a modest amount of help. But they are not designed to fund ongoing custodial long-term care in the way a long-term care policy is. In other words, Medicare Advantage may make the medical side of the journey smoother, but it is not a true solution for multi-year custodial care needs.
That’s why many households treat Medicare as the foundation for medical coverage, then build a separate plan for extended care. If your goal is to protect retirement assets, it’s important to avoid confusing “helpful benefits” with “long-term funding.” The funding question is the one that impacts lifestyle choices, independence, and whether a spouse can remain financially secure.
How Long-Term Care Insurance Fills the Gap
Long-term care insurance is built to pay for the services Medicare excludes—home care, assisted living, memory care, adult day care, and nursing facilities. It preserves choice and independence by letting you decide where care happens. Instead of forcing a care decision based on finances, the right policy creates options: more time at home, more flexibility in facility selection, and less pressure on family caregivers.
Some households prefer hybrid life insurance with LTC benefits, which can accelerate the death benefit for care and still leave a benefit to heirs if care isn’t needed. If you’re coordinating income and care planning, it can also help to monitor current annuity rates and designs that integrate income with care funding.
At Diversified Insurance Brokers, we help families compare these designs in plain language. The “best” approach is the one that matches your goals: maximum leverage for care, maximum flexibility, predictable premiums, or a plan that protects heirs if you never need care. The right fit often depends on whether you want ongoing premiums, a single-premium repositioning strategy, or a life policy that doubles as a care funding tool.
Medicare vs. Long-Term Care Insurance: A Clear Comparison
- Medicare: Short-term skilled care after a hospital stay; limited duration with continued medical necessity.
- Medicare Advantage: May include limited in-home support or care coordination; not a substitute for custodial long-term care.
- LTC Insurance: Ongoing help with ADLs, memory care, assisted living, and nursing home care—regardless of hospital history.
The “Medicare Gap” in Real Life: What Families Actually Face
Most long-term care situations don’t begin with a dramatic event. They begin with small, persistent changes: falls risk, medication mismanagement, memory issues, limited mobility, or the inability to handle basic household tasks. Families often step in quietly at first, helping with groceries or rides to appointments. Over time, that support can expand into daily care demands that are hard to sustain—especially if adult children live out of state or spouses have their own health issues.
When the care needs become consistent, the cost becomes real. Home care can be the most flexible option, but it can still be expensive if many hours per week are needed. Assisted living can provide supervision and help with daily routines, but it is typically private pay. Memory care can be higher-cost and can last longer than many families anticipate. Nursing home care is usually the most expensive setting, and it often becomes relevant when care needs become complex or safety becomes unmanageable at home.
The earlier a household addresses the gap, the more control they keep. Planning early isn’t about assuming the worst—it’s about preserving choices, protecting a healthy spouse, and reducing the chance that a family has to make a rushed decision under pressure.
Planning Windows & Smart Couple Designs
Most people explore coverage between ages 50–65, when premiums and underwriting are more favorable. Waiting until health changes can limit options or remove certain designs from the table. For couples, a shared-benefit rider lets either spouse tap a combined pool—adding flexibility without over-insuring each person. This is especially useful because one spouse may never need care while the other could need care for an extended period.
Many states also offer LTC Partnership reciprocity, which can protect assets from Medicaid spend-down if policy benefits are exhausted. Partnership design is not right for everyone, but for certain households it can be a meaningful “backstop” strategy that reduces the fear of a total spend-down scenario.
In a planning conversation, we often translate these features into practical questions: How long would you want care funded? Where would you prefer it to happen? How much risk are you comfortable self-insuring? And what impact would a multi-year care bill have on the surviving spouse’s lifestyle?
Integrating Annuities & Care Benefits
Some retirees pair LTC coverage with an annuity that includes long-term care benefits. These designs can grow safely and then multiply values for qualified care, helping bridge cash-flow gaps while keeping funds available if care isn’t needed. For households that dislike the idea of “use it or lose it,” these strategies can feel more comfortable because there is generally still an account value component.
When these strategies fit, they can help solve two problems at once: protecting principal while living, and creating a larger pool available for care if needed. They can also simplify budgeting because the care benefits are often designed as a defined pool or a defined monthly benefit for a period of time, depending on the structure.
Why Relying on Medicaid Should Be a Last Resort
Medicaid will pay for long-term care only after strict financial eligibility is met, which often means spending down assets and accepting reduced choice of facilities. In many cases, the facility decision becomes limited to what is available and what accepts Medicaid, not what is ideal for location or quality of life. A private policy preserves options and control for you and your family.
Just as important, Medicaid planning often becomes stressful because it is reactive. Families may make rushed financial decisions in the middle of a crisis. Proactive planning doesn’t mean you will never use Medicaid—it means you don’t have to plan your life around Medicaid as the default option.
Next Steps: Build a Personalized Strategy
The first step is to understand your risks and local care costs, then choose a design that balances protection and affordability. We’ll compare traditional LTC, hybrid long-term care, and annuity-based approaches—plus show how benefits coordinate with Medicare and other income sources.
Need Help Understanding Your Medicare Coverage?
We’ll explain how hospital stays, skilled nursing rules, and plan structure impact your out-of-pocket exposure—then help you coordinate the long-term care plan around it.
See Your LTC Options & Estimated Costs
Side-by-side quotes from top carriers, tailored to your age, health, and goals.
Questions? 800-533-5969
Key Takeaways
- Medicare covers short-term skilled care—not custodial care or assisted living.
- Long-term care insurance funds extended care at home, in assisted living, memory care, or nursing facilities.
- Hybrids and annuity-based riders add flexibility if care is never needed.
- Most people apply between ages 50–65 for better pricing and approval odds.
- Couples can boost efficiency with shared benefits and consider Partnership protection.
Related Pages
Explore these resources to go deeper on Medicare limitations and long-term care planning strategies.
Financial Protection Essentials
Chronic condition underwriting, burial insurance solutions, legal funding guidance, and specialized life insurance structures.
Questions now? Call 800-533-5969
FAQs: Does Medicare Cover Long Term Care?
Does Medicare pay for long-term care?
No. Medicare only covers short-term skilled nursing care after a hospital stay, not custodial or ongoing long-term care.
What’s the difference between skilled and custodial care?
Skilled care involves licensed medical professionals providing therapy or treatment. Custodial care includes help with daily living activities like eating or dressing.
Does Medicare Advantage include long-term care?
Most Medicare Advantage plans do not include long-term care benefits beyond limited skilled services. You’ll still need private long-term care insurance for full coverage.
When should I buy long-term care insurance?
Most people purchase coverage between ages 50 and 65, when premiums are affordable and health qualifications are easier to meet.
Can I get long-term care coverage if I have pre-existing conditions?
Yes, in many cases. Hybrid or annuity-based policies often offer easier medical approval than traditional plans.
Does Medicaid pay for long-term care?
Yes, but only after you spend down your assets to qualify. Private long-term care insurance helps preserve your savings and independence.
About the Author:
Tonia Pettitt, CMIP©, is a seasoned Medicare specialist with more than 40 years of hands-on experience guiding individuals and families through the complexities of Medicare planning. As a senior advisor with the nationally licensed independent agency Diversified Insurance Brokers, Tonia provides clear, dependable guidance across all areas of Medicare—including Medicare Advantage, Medicare Supplement (Medigap), and Part D prescription coverage. Leveraging active contracts with dozens of highly rated insurance carriers, she helps clients compare options objectively and secure the most suitable coverage for their health and budget.
Known for her patient, education-first approach, Tonia has built a reputation as a trusted resource for retirees seeking reliable, unbiased Medicare support. With four decades of experience across evolving Medicare laws, carrier changes, and plan structures, she brings unmatched insight to every client conversation—ensuring clients feel confident, protected, and fully prepared for each stage of their retirement healthcare journey.
