ACA Alternatives for my Company Healthcare

Jason Stolz CLTC, CRPC
ACA Alternatives for My Company Healthcare is a search phrase that often appears when an employer feels stuck. A traditional ACA-compliant fully insured group health plan may have worked for a few years, but eventually the renewal cycle begins to feel like a treadmill: premiums increase, options narrow, plan changes are forced, and the business gets very little clarity on what is actually driving costs. When that happens, employers usually are not trying to get rid of group benefits. They are trying to keep group benefits, while changing the way the plan is funded and managed so the company has more control over the future.
The most effective ACA alternatives for my company healthcare are usually not “alternatives” in the sense of replacing group coverage with something weaker. They are alternatives in the sense of changing the underlying structure from a fully insured model into a model that shares risk differently, separates administrative costs from claims costs, and gives the employer more transparency. In practice, that typically means evaluating self-funded group health plans, partially self-funded options, and level-funded arrangements that can preserve group benefits while improving predictability and long-term sustainability.
At Diversified Insurance Brokers, we help employers nationwide evaluate whether a self-funded or partially self-funded group health strategy is a better fit than a fully insured ACA group plan. The value is not only in the premium comparison. The value is in understanding where healthcare dollars are being spent, whether the company is paying for worst-case scenarios that never occur, and whether changing the funding approach can create a more stable and controllable long-term outcome.
Employers often reach this decision point after consecutive years of large renewal increases, after a carrier exits the market, or after plan options become so limited that employee satisfaction suffers. In other cases, the company is simply growing and wants a healthcare strategy that can scale. Regardless of the trigger, the conversation usually begins the same way: the company wants to know what alternatives exist that still maintain legitimate group health coverage and do not turn healthcare into a constant annual crisis.
This page walks through how self-funded and level-funded group health plans work, why they are commonly viewed as practical ACA alternatives for employers, how risk is controlled using stop-loss insurance, what types of companies tend to benefit most, and how to think about the decision as a long-term strategy rather than a one-year premium reaction.
Explore ACA Alternatives for Company Healthcare
If renewals are rising and options are shrinking, compare fully insured plans against self-funded and level-funded group strategies.
Why Employers Look Beyond Fully Insured ACA Group Health Plans
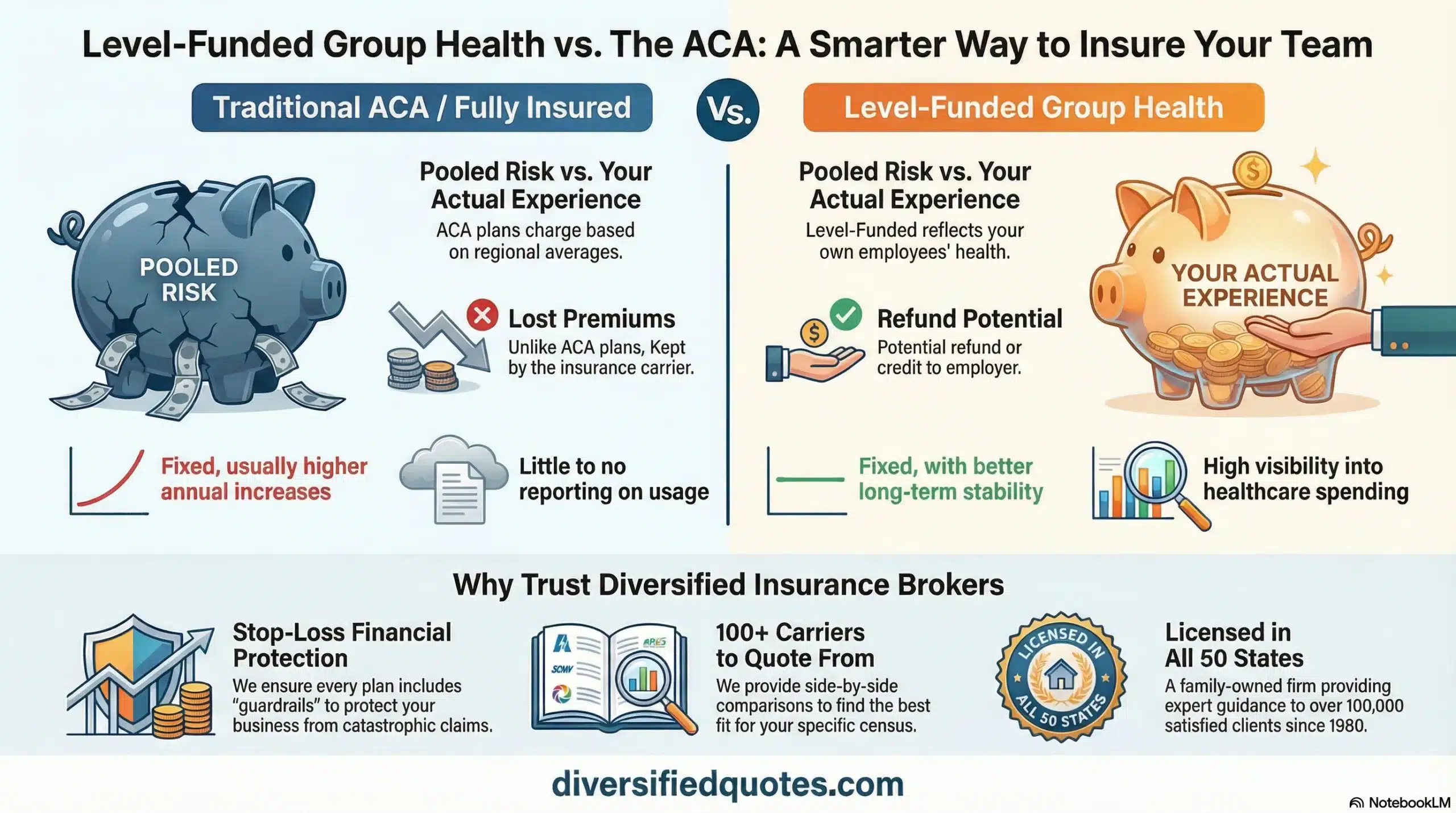
Fully insured ACA group health plans are designed to be simple. The employer pays a fixed premium to the insurance carrier, the carrier assumes claim risk, and the employer receives a packaged solution that includes administration, network access, and compliance support. That simplicity has value. The tradeoff is that the employer is paying for a “bundle” that includes claims risk pricing, carrier profit margins, and administrative costs inside one monthly number, with limited insight into how that number is built.
Over time, many employers begin to feel that the bundle is working against them. Premium increases arrive at renewal, and the reasoning often feels vague. Even businesses with stable employee populations and low utilization may see significant increases because the carrier is pricing not only for that company’s experience, but also for larger risk pool trends, regional medical inflation, and carrier margin needs. When employees ask why the plan changed or why payroll deductions went up, the employer frequently does not have a satisfying explanation.
Another issue is flexibility. Fully insured small group markets can be thin in certain regions, which means plan design options may be limited. The employer might have to choose between a high deductible plan that employees dislike or a richer plan that is financially unsustainable. As the company grows, that problem compounds. Employers end up making decisions that are reactive, not strategic, because they are operating inside an annual renewal system that does not reward long-term thinking.
This is why many businesses begin searching for ACA alternatives for my company healthcare. They are looking for a way to keep group benefits intact, while changing how costs are funded, how risk is managed, and how much transparency the employer can gain.
What “ACA Alternatives” Actually Means in Employer Group Coverage
There is a lot of confusion around the phrase “ACA alternatives.” Some people assume it means dropping group coverage or moving employees onto individual policies. For many employers, that is not the goal at all. When employers talk about ACA alternatives for company healthcare, what they usually mean is finding a group strategy that follows required protections while improving control and cost management.
Self-funded and level-funded group plans are still group health plans. They still involve a legitimate employer group structure, and they still involve the employer providing healthcare benefits as part of compensation strategy. The difference is not in whether coverage exists. The difference is in how the plan is funded, how claims are paid, and how risk is shared between the employer and insurance protection layers.
For a practical foundation on how these structures work, review what is self-funded group health insurance. That page breaks down the mechanics in a way that helps employers understand the core difference between paying a carrier premium and funding claims more directly.
How Self-Funded Group Health Works as an Employer Strategy
In a self-funded group health plan, the employer pays employee claims as they occur rather than paying a fixed “all-in” premium to an insurance carrier. The plan still uses a network, still uses an administrator, and still uses contractual plan documents. The employer is essentially funding the healthcare costs directly, while outsourcing administration and limiting catastrophic risk through stop-loss protection.
This structure creates a different kind of transparency. Instead of the employer paying a bundled premium, the employer can see how much of its spend goes toward actual claims versus administrative costs. Over time, that insight can allow the employer to make better decisions about plan design, vendor selection, and cost-control strategy. It also can reduce the feeling of helplessness that many employers experience in fully insured renewals.
Self-funding is not a fit for every business. It requires more strategic planning, more attention to compliance support, and a willingness to evaluate claims trends over time. However, when structured correctly, it can create a framework that rewards favorable utilization rather than pricing every company as if worst-case utilization is inevitable.
Partially Self-Funded and Level-Funded Group Plans
Many employers prefer a stepping-stone approach rather than moving directly into a pure self-funded model. That is where partially self-funded and level-funded plans become popular. These structures preserve many of the advantages of self-funding, while keeping monthly costs more predictable.
In a level-funded plan, the employer pays a fixed monthly amount, but that amount is typically broken into components. Part of the payment is administrative cost. Part is stop-loss cost. Part is claims funding. Claims are paid from a dedicated account. If claims run lower than expected, the employer may receive a refund, a credit, or a renewal adjustment depending on the plan design. That potential benefit is why level funding is often positioned as a practical ACA alternative for employers who want cost control without unpredictable swings.
Employers considering level funding often want to understand whether a refund is realistic and how it is calculated. For that, review can small groups get health insurance refunds. While outcomes are never guaranteed, understanding how these models treat surplus can help the employer set realistic expectations.
How Stop-Loss Insurance Protects the Employer
Stop-loss insurance is the protection layer that makes self-funded and partially self-funded group plans viable for most employers. Without stop-loss, the employer could be exposed to catastrophic claims. With stop-loss, the employer’s exposure is capped within known ranges.
There are typically two forms of stop-loss protection. Individual stop-loss limits exposure from a single high-cost claim. Aggregate stop-loss caps total claims for the plan year. When coordinated correctly, these protections stabilize the financial risk profile while allowing the employer to benefit from favorable claims experience.
Stop-loss is not just a checkbox. The details matter. Deductible levels, contract terms, renewal provisions, and coverage definitions influence both cost and protection. Employers exploring this path should understand stop-loss mechanics before transitioning away from fully insured coverage. To get a deeper explanation, review understanding stop-loss insurance in level funded plans.
Compare Fully Insured vs Level Funded for Your Company
See how your renewal options change when you separate claims costs, admin costs, and stop-loss protection into a structured strategy.
Which Employers Are Best Suited for Self-Funded or Level-Funded Plans
Employers often ask whether they need to be a certain size before self-funding becomes realistic. In practice, suitability depends less on size and more on stability, participation, and long-term goals. A company with consistent employment, strong participation, and leadership committed to managing healthcare as a strategy can often explore level funding earlier than expected. Some groups benefit most when the workforce is younger and healthier, but even mixed-risk groups can see value when plans are designed correctly and stop-loss is structured conservatively.
Employers often begin exploring ACA alternatives for company healthcare after repeated premium increases, after benefit dissatisfaction grows, or after plan options become limited. Another common trigger is growth. As payroll increases and headcount expands, the company wants a strategy that scales. In those situations, level funding can provide a path that offers cost predictability while creating potential upside if claims experience is favorable.
Employers evaluating whether group alternatives are feasible should also review eligibility thresholds. For reference, minimum employees for group health insurance provides context on when different carrier models become available and what participation requirements often look like.
Transparency and Claims Data Access
One of the biggest differences between fully insured and self-funded group plans is visibility. Fully insured plans often provide very limited insight into where healthcare dollars are actually going. Employers may receive broad summaries, but rarely receive actionable information that explains whether costs are driven by high utilization, pharmacy spend, specialty claims, or network dynamics.
Self-funded and partially self-funded structures typically provide more claims reporting. That reporting does not have to be overly complex, and privacy protections remain in place. The value is that the employer can identify patterns. If outpatient imaging is driving spend, the employer can explore plan design changes. If pharmacy costs are rising, the employer can explore formulary strategies or vendor options. If preventive care utilization is low, the employer can implement targeted education. The key is that decisions can be based on information rather than guesswork.
This is where self-funding begins to feel less like an insurance product and more like a cost management system. Employers shift from receiving a renewal “rate action” to having an ongoing framework for understanding and influencing healthcare trends.
Plan Design Flexibility Under Self-Funding
Employers who feel trapped by fully insured plan menus often find self-funded designs refreshing. Instead of selecting from a narrow set of carrier-defined options, employers can tailor deductibles, copays, coinsurance structures, network configurations, and wellness incentives to align with the company’s goals. This flexibility can allow the employer to maintain competitive benefits while still addressing cost containment.
Plan design flexibility is especially valuable when the employer wants to avoid blunt cost shifting. Many employers are willing to make employees more conscious of utilization, but they do not want to simply raise payroll deductions and hope for the best. With self-funding or level funding, plan design can be adjusted strategically so employees still feel supported while the employer improves long-term sustainability.
For employers who want to understand tradeoffs clearly, the page pros and cons of self funded group health is helpful for framing the decision around transparency, risk control, and plan flexibility.
Compliance Considerations
Self-funded group plans can require additional compliance attention. Employers must consider ERISA plan documentation, required notices, reporting obligations, and nondiscrimination rules. That sounds intimidating, but most of the work is handled by experienced third-party administrators and the advisors structuring the plan. The key is working with teams that build compliance into the plan design rather than treating it as an afterthought.
When compliance is done correctly, most employers find that the additional administration is manageable. In exchange, the employer gains transparency, flexibility, and long-term cost management leverage. For many businesses, that is a worthwhile trade.
Cost Control vs Cost Shifting
A common concern is that moving away from fully insured plans will cause costs to be pushed onto employees. In well-designed self-funded and partially self-funded plans, the goal is not cost shifting. The goal is cost control. That means aligning plan design with actual utilization, using data to identify drivers, and building a system that rewards favorable claims experience rather than pricing the employer for worst-case outcomes every year.
In many cases, employers can maintain competitive benefits while slowing the pace of increases. Even when employee contributions rise modestly, employees often perceive the plan as more valuable because network access and out-of-pocket structures may improve compared to narrow fully insured options.
Long-Term Strategy vs Annual Renewal Cycles
Fully insured group health tends to force an annual decision cycle. The company receives renewal numbers and must react. Self-funded and level-funded approaches allow the company to think long-term. Claims trends can be addressed proactively. Vendor performance can be evaluated. Plan design can be adjusted intentionally. Instead of being trapped in a yearly scramble, the company can build a multi-year strategy that improves predictability.
This long-term approach is often what employers mean when they ask for ACA alternatives for my company healthcare. They want control. They want clarity. They want a structure that makes costs understandable and manageable.
As employers evaluate these options, it can also help to frame the decision in the context of broader group planning. If you want a wider overview of employer coverage strategy, visit group medical insurance and how plan structures differ across funding models.
Review Your Renewal Before You Accept It
Before locking into another fully insured renewal, compare ACA group coverage against level-funded and self-funded strategies built for long-term stability.
Related Group Health Pages
Keep exploring employer health strategies, funding models, and eligibility questions.
Financial Protection Essentials
Chronic condition underwriting guidance, dental and vision options, financial firm reviews, and state-level consumer protections.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
What are the main ACA alternatives for group health insurance?
The primary ACA alternatives that still maintain a group health structure are self-funded group health plans, partially self-funded plans, and level-funded arrangements. These options change how claims are paid and managed while preserving employer-sponsored coverage.
Are self-funded group health plans ACA compliant?
Yes. Self-funded group health plans must still follow many ACA rules, including coverage requirements and employee protections. Employers comparing structures often review differences between traditional fully insured plans and small employer group health insurance options before deciding.
What is the difference between fully insured and partially self-funded plans?
Fully insured plans charge fixed premiums that include claims risk and carrier profit. Partially self-funded plans separate claims funding from administration and use stop-loss insurance to limit employer risk. Businesses exploring flexibility may also consider 2-person group health insurance options when evaluating eligibility.
How does stop-loss insurance protect my company?
Stop-loss insurance caps your financial exposure by limiting the cost of individual high claims and total annual claims, making self-funded plans more predictable for employers. Understanding how carriers manage reserves—outlined in resources like how insurance companies use premium dollars—can also clarify how risk is structured.
What size company is best suited for self-funded group health?
While larger employers commonly self-fund, many small and mid-sized companies can also benefit, especially when employee health is stable and participation levels are strong. Employers transitioning from ACA-rated coverage often start by reviewing short-term health insurance cost comparisons to understand structural pricing differences.
Can self-funded group health plans lower costs?
They can, especially for employers with favorable claims experience. Self-funding improves transparency and allows employers to avoid paying for unused risk margins built into fully insured plans. Comparing administrative structures to traditional group health brokerage models can highlight potential efficiencies.
Is self-funded group health riskier for employers?
Self-funded plans involve more responsibility, but stop-loss coverage and proper plan design significantly reduce financial risk compared to paying fixed premiums year after year. Employers weighing risk tolerance often compare this approach against fully insured vs. self-funded plan structures.
Do self-funded plans still offer employee choice and coverage flexibility?
Yes. Self-funded and partially self-funded plans often provide more flexibility in plan design, provider networks, and cost-sharing options than traditional ACA-rated fully insured plans. Many employers also integrate wellness initiatives or specialty programs to improve long-term claims outcomes.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers, is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient.
