How Much Health Insurance Does My Business Need

Jason Stolz CLTC, CRPC
One of the most common questions business owners ask is, “How much health insurance does my business need?” The answer is not a fixed dollar amount, because the “right” amount of coverage depends on your workforce, your budget, your hiring goals, and the risk your company can comfortably absorb. In other words, when you ask how much health insurance does my business need, you’re really asking how to build a plan that protects employees from major medical costs while keeping the business stable and competitive.
Group coverage should be viewed as a strategy, not just an expense. For some organizations, the goal is hiring leverage and retention. For others, it’s long-term cost control and renewal stability. For larger employers, it can become a managed financial system where plan structure, data transparency, and governance matter as much as carrier selection. You can see how plan strategies change at scale by reviewing group health insurance for over 1,000 employees.
At Diversified Insurance Brokers, we help employers determine how much health insurance their business needs based on real-world inputs: employee demographics, expected utilization, participation, contribution strategy, compliance requirements, and the level of benefits you want to offer as part of total compensation. Whether you have a micro team or a growing organization, the goal is the same: meaningful protection without overspending on features that won’t improve outcomes.
How Much Health Insurance Does My Business Need?
Get a clear recommendation on coverage level, contribution strategy, and plan structure—based on your company size, budget, and goals.
Why “How Much” Means More Than Monthly Premiums
It’s normal to start with premiums, because premiums are the most visible cost. But premiums are only one piece of what determines how much health insurance your business needs. The true cost of coverage includes the plan’s deductible and out-of-pocket exposure, how much the employer contributes, how employees share costs, and how predictable the plan remains at renewal.
Two plans can have similar premiums and deliver completely different real-world outcomes. A lower-premium plan with very high out-of-pocket costs can lead to delayed care and dissatisfaction, especially for employees who actually use healthcare. A richer plan can improve satisfaction but may restrict cash flow or reduce flexibility elsewhere in compensation. The right amount of coverage typically sits in the middle: strong catastrophic protection, reasonable access to care, and a design that employees can actually use without financial shock.
Another reason “how much” is more than premiums is that most employers do not want to rebuild their plan every year. Your coverage level should be sustainable. A plan that looks affordable today but triggers steep renewal increases later can cost more over a three- to five-year window than a plan built for stability from day one.
A Practical Baseline for “Enough” Coverage
When business owners ask how much health insurance does my business need, a helpful starting point is defining what “enough” means. In most cases, “enough” means your plan protects employees from catastrophic medical costs and provides practical access to care for the services they use most often—primary care, urgent care, prescriptions, labs, and common specialists.
From an employer perspective, “enough” also means your plan supports workforce stability. If the plan is so lean that employees can’t afford to use it, the benefit loses value. If the plan is so rich that it competes with payroll or growth investment, it becomes a long-term financial strain. “Enough” is the plan that your business can maintain confidently through normal cost increases while still being competitive in your market.
If you want to understand the building blocks behind employer coverage, the overview page on group medical insurance helps clarify how plan pricing, risk pooling, and structure impact what you actually pay over time.
How Company Size Changes the Right Coverage Level
Company size influences what you can access and what tends to work best. Smaller teams often prioritize affordability and simplicity, especially if budgets are tight and administrative time is limited. As groups grow, more plan options become available, and the employer typically gains leverage to negotiate structures that create better long-term stability.
If your company is on the smaller end, you may be deciding between one strong plan versus offering multiple plan choices. Some small employers choose a single plan because it’s easier to manage and communicates “this is our plan.” Others offer two options—a lower-cost plan and a richer plan—so employees can choose based on utilization and family needs. If you want a baseline view for smaller organizations, explore small business group health insurance.
As your group grows, the “right amount” of coverage becomes less about picking a single plan and more about designing a structure that remains stable at renewal. That can mean stronger plan governance, better reporting, and exploring funding models that reward favorable experience rather than treating every renewal as a reset. The larger you are, the more important structure becomes compared to premium shopping alone.
Workforce Demographics and Utilization Patterns
Employee demographics can quickly change what “enough” looks like. A younger workforce may prefer lower premiums and a higher deductible—especially if most employees are healthy, rarely use healthcare, and mostly want protection against large unexpected events. In that environment, an HSA-compatible plan can feel valuable because it blends lower premiums with a long-term savings tool.
An older workforce or a workforce with more families often values predictability and lower out-of-pocket exposure. Employees who regularly use prescriptions, labs, specialists, or ongoing care are more sensitive to deductibles, coinsurance, and pharmacy design. For these groups, a plan that is “too lean” can increase dissatisfaction even if premiums look attractive.
Industry also matters. Physically demanding roles often have higher utilization due to strains, injuries, and follow-up care that isn’t always work-comp related. Office-based roles may have different utilization patterns that emphasize preventive care, mental health access, and prescription coverage. When you align plan design with utilization reality, you reduce waste and increase perceived value.
Employer Contributions and Participation Requirements
Another major variable in how much health insurance your business needs is how much you plan to contribute as an employer. Most group plans include minimum contribution guidelines, and your contribution strategy affects both participation and perceived benefit strength. A plan can look “thin” or “strong” depending on what the employee actually pays per paycheck.
Many employers focus on employee-only contributions first, then decide whether and how to support dependents. Dependent support can significantly change total cost, but it can also be a powerful retention lever—especially in industries where family coverage is a deciding factor for staying with an employer.
Participation requirements matter too. Carriers often expect a minimum percentage of eligible employees to enroll, although valid waivers (coverage through a spouse, another employer plan, or certain other sources) can reduce the required enrollment threshold. If you’re evaluating whether your group meets basic eligibility standards, see minimum employees for group health insurance for a clear starting framework.
Choosing the Right Plan Structure
For many employers, “how much” coverage you need is directly tied to the structure you choose. Some structures prioritize predictability. Others prioritize long-term savings and transparency. A plan that fits your company today may not fit as you grow, which is why structure should be reviewed proactively rather than only at renewal time.
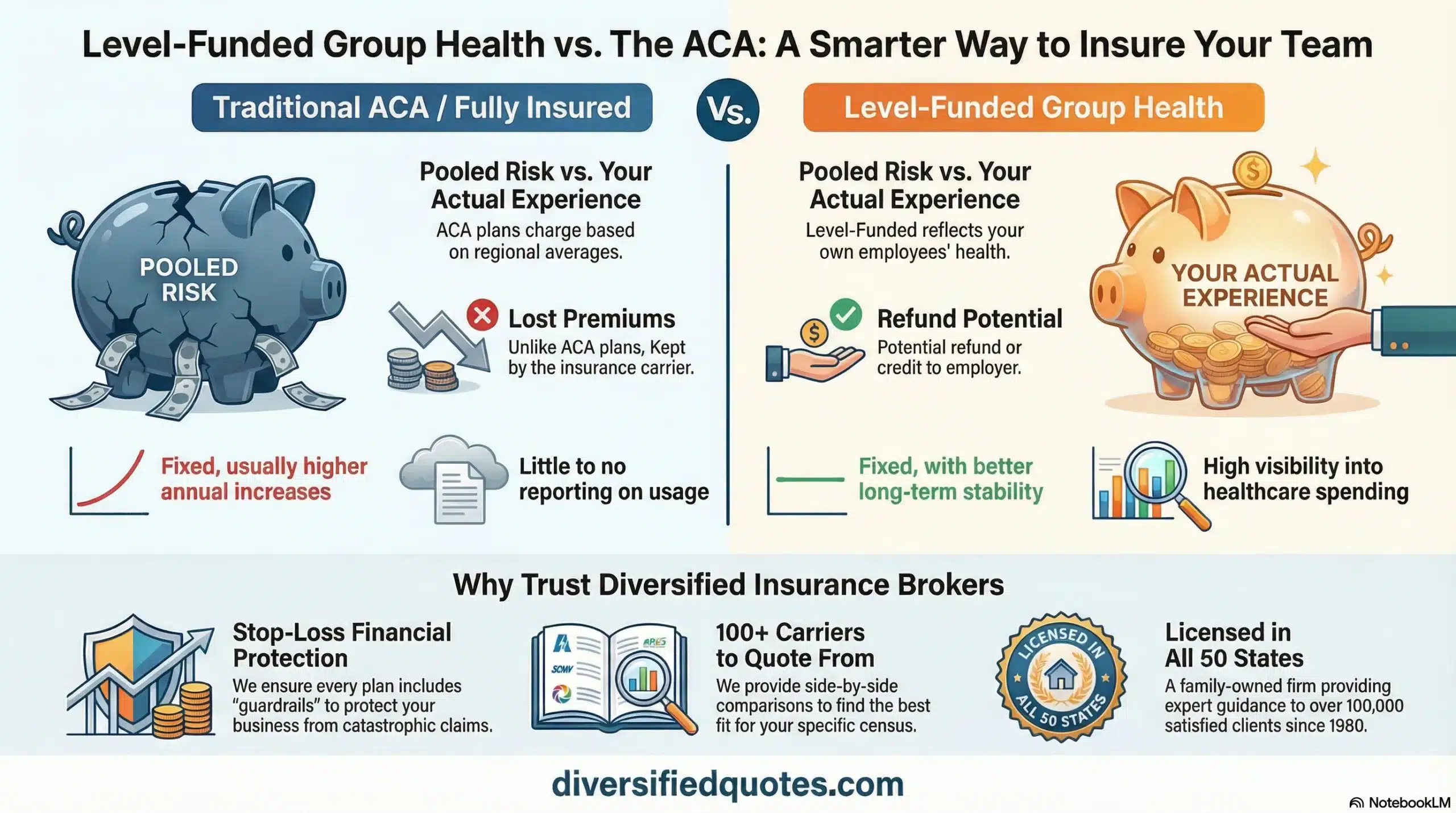
Traditional fully insured plans can be a good fit for businesses that want simple administration and predictable monthly billing. The tradeoff is that you typically have less transparency into what drives cost increases, and the plan can become reactive—especially if renewal increases outpace revenue growth.
Many employers explore level-funded or partially self-funded designs when they want better cost control without taking on unlimited risk. These structures can improve transparency, align costs more closely with your group’s experience, and create more levers to manage long-term trend. If you want the foundation behind these models, start with what is self-funded group health insurance.
Structure is also about risk tolerance. Some companies prefer a model where the carrier absorbs more risk. Others prefer a model where they retain some risk in exchange for transparency and potential savings. The “right” answer depends on your cash flow stability, workforce predictability, and tolerance for variance.
Plan Design: Deductibles, Networks, and Employee Experience
Coverage level isn’t just the plan name or the premium. It’s how employees experience the plan. Network access is one of the biggest drivers of satisfaction. A plan that looks affordable can create frustration if employees lose access to preferred doctors, hospitals, or local systems. In many cases, a slightly higher-cost plan with better access produces better retention and less disruption.
Deductibles and cost sharing should match your employee population. If most employees rarely use healthcare, a higher deductible plan paired with employer contributions to an HSA can be a strong strategy. If employees regularly use services, the plan should reduce “bill shock” for common care and prescriptions. The best designs avoid extremes: not so lean that nobody can use it, and not so rich that it strains the business unnecessarily.
Finally, consider the practical tools that help employees navigate the plan. Telehealth access, clear pharmacy design, and straightforward urgent care benefits can increase plan value without dramatically increasing cost. A plan that employees understand and use properly often performs better than a plan that is richer on paper but confusing in practice.
Layering Benefits to Strengthen Protection Without Overspending
Many employers assume the only way to improve benefits is to buy a richer medical plan. In reality, one of the most effective ways to increase protection without overspending is to layer supplemental benefits strategically. These benefits can fill common gaps—especially for high-deductible medical plans—without forcing medical premiums dramatically higher.
For example, some employers add hospital indemnity coverage to provide cash benefits when employees face inpatient stays. Others add accident insurance for unexpected injuries, which can be particularly relevant in physically demanding industries. Some also evaluate critical illness coverage to help employees manage the financial impact of major diagnoses.
This layered approach often improves employee perception and financial protection while letting the business keep the core medical plan in a sustainable range. It can also help employers maintain recruitment competitiveness even when medical premiums rise market-wide.
Compliance Factors That Influence What You “Need”
Compliance requirements can influence the minimum level of structure you need, especially as you grow. Employer size determines which rules apply, including certain ACA-related requirements and reporting obligations. Even smaller employers must follow carrier rules on eligibility, enrollment timing, and participation. Poor setup can cause coverage disruptions, disputes, or administrative issues that become expensive to fix later.
Because the rules and best practices can be complex, many employers work with an independent insurance broker who can help align plan design with eligibility rules and long-term strategy. The objective is not to add complexity. The objective is to build a plan that works, stays in force, and can evolve as the business changes.
Health Insurance as Part of Total Compensation
Health insurance should be evaluated as part of total compensation, not in isolation. Employees typically weigh pay, flexibility, culture, and benefits together. In competitive hiring markets, group health coverage is one of the first benefits candidates ask about, and the quality of the plan can influence the level of wage pressure you experience.
Businesses that under-insure may save money in the short term but face higher turnover and recruiting challenges. Businesses that over-insure may reduce flexibility in other areas—like wages, bonuses, training, or retirement benefits. The goal is to offer a plan that feels meaningful, fits your hiring market, and remains sustainable as the company grows.
If you’re building a longer-term benefits strategy, your plan should be designed to scale. That means the decision you make today should not lock you into a model that becomes unstable or uncompetitive within one or two renewal cycles.
Get a Group Health Insurance Review
We’ll help you determine how much coverage your business really needs—and build a plan that balances employee protection with cost control.
How Diversified Insurance Brokers Helps Employers Decide What’s “Enough”
When employers ask how much health insurance does my business need, our first step is clarifying the outcome you want: recruiting leverage, retention stability, cost predictability, better networks, or a structure that supports long-term control. Then we compare plan options through that lens, including contribution strategy, participation stability, and the pros and cons of different funding models.
We also help employers avoid the common renewal trap: reacting to rate increases by cutting benefits or shifting costs to employees without fixing the underlying structure. In many cases, better results come from a smarter plan design and a clearer long-term strategy—so you’re not rebuilding every year.
Financial Protection Essentials
Executive coverage strategies, senior care planning, inherited IRA education, and advanced retirement income concepts.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
Frequently Asked Questions
How much should a small business pay for group health insurance?
Most small businesses focus on a monthly budget per employee, then choose plan designs that fit. The “right” amount depends on employer contribution strategy, employee demographics, and whether you want a richer plan for recruiting or a leaner plan for cost control.
Do I need to pay 100% of my employees’ premiums?
No. Most group plans only require the employer to pay a minimum percentage toward employee-only coverage. Many employers choose to contribute more than the minimum to improve participation, retention, and overall plan stability.
What’s more important: lower premiums or lower out-of-pocket costs?
It depends on how your team uses healthcare. Lower premiums often mean higher deductibles and higher out-of-pocket costs. A balanced plan aims to keep both the employer budget and employee experience sustainable, especially during years with higher medical utilization.
How do I choose the right deductible for my business plan?
Start by looking at affordability for employees. If the deductible is too high relative to wages and savings, the plan may feel unusable. Many employers pair higher deductibles with strategies like HSA-compatible plans or supplemental benefits to reduce “surprise” costs.
How many employees do I need to qualify for group health insurance?
Eligibility depends on the type of group and the carrier’s rules. Some plans allow very small groups, while others have participation and contribution requirements. If your business is small, plan options can vary by state and carrier guidelines.
What is the biggest mistake employers make when choosing group health insurance?
The most common mistake is choosing a plan based only on the lowest premium without considering deductibles, network access, prescription coverage, and how employees actually use care. That approach often leads to dissatisfaction and higher turnover.
Can my business offer more than one health plan option?
Yes. Many employers offer two options—often a lower-premium plan and a richer plan—so employees can choose based on their needs. The best structure depends on your size, administrative capacity, and participation requirements.
How does a self-funded or level-funded plan change what my business “needs”?
Alternative funding models can shift how costs are managed by separating predictable fixed costs from variable claim risk. For some groups, these options improve long-term cost control, but they require careful plan design and claims-risk awareness.
Should I include dental and vision, or focus on medical only?
Medical coverage is usually the priority, but dental and vision can improve perceived value at relatively low cost. Many employers add them to strengthen the benefits package without significantly increasing medical premiums.
How often should I review my business health insurance coverage?
At least annually—before renewal. It’s also smart to review coverage after hiring growth, budget changes, major claims years, or when employees report access issues with networks or prescription coverage.
About the Author:
Jason Stolz, CLTC, CRPC and Chief Underwriter at Diversified Insurance Brokers (NPN 20471358), is a senior insurance and retirement professional with more than two decades of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, Group Health, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient. Visitors who want to explore current annuity rates and compare options across multiple insurers can also use this annuity quote and comparison tool.
