Group Health Insurance for 90 Employees
Group Health Insurance for 90 Employees

Jason Stolz CLTC, CRPC
Group health insurance for 90 employees represents a critical transition point where healthcare strategy directly affects operating margins, employee retention, and long-term scalability. At this size, insurance carriers rely far less on generalized small-group pricing and far more on your organization’s actual claims behavior — which means the decisions your team makes about plan design, funding structure, network selection, and pharmacy strategy have a direct and measurable impact on what you pay and what you receive at renewal. Employers at 90 employees who continue using off-the-shelf fully insured plans frequently see rising premiums with limited explanation and no meaningful path to influence outcomes.
For companies with 90 employees, scale becomes a genuine strategic advantage when it is used deliberately. Claims volume is typically sufficient to support more advanced funding arrangements, enable more accurate pricing based on your group’s actual experience, and create stronger leverage in renewal negotiations. When structured correctly, group health insurance at this level can reduce waste, improve cost predictability, and reward good claims performance without sacrificing benefit quality or forcing disruptive changes on the employee population that affect morale and retention.
At Diversified Insurance Brokers, we help organizations with approximately 90 employees redesign group health insurance around transparency, cost accountability, and long-term financial control. The objective is to treat healthcare as the significant financial system it has become — so leadership can manage costs proactively and strategically rather than reacting to each year’s renewal as an unpredictable external event.
Group Health Review for 90 Employees
We’ll analyze your current plan, renewal exposure, and claims efficiency to identify cost-saving opportunities specific to your organization’s size and profile.
Request a Group Health ReviewWhy Group Health at 90 Employees Requires a Strategic Approach
Group health insurance at 90 employees is no longer driven primarily by broad risk pooling with other employers of similar size. Underwriters typically have enough data from a group this size to identify utilization trends, chronic condition prevalence, specialty pharmacy exposure, and recurring cost drivers with meaningful clarity. In practice, this means your plan structure matters more — because your organization’s own claims behavior has a direct and substantial influence on both current-year pricing and future renewal outcomes. You are no longer invisible in the underwriting process.
Employers who rely solely on fully insured plans often pay premiums that include built-in conservatism — carrier risk margins, administrative loading, and limited visibility into where costs are actually coming from. Over time, this structure can cause healthcare spending to grow faster than actual underlying claims performance, particularly when the plan contains hidden inefficiencies: a network that does not align with where employees actually receive care, unmanaged specialty pharmacy exposure, or plan design features that inadvertently route employees toward higher-cost sites of care for services that could be obtained at significantly lower cost in other settings.
Understanding how group medical insurance is priced at different employer sizes helps clarify why proactive plan design becomes essential rather than optional at 90 employees. Healthcare costs at this scale are large enough to materially affect operating margins, predictable enough to be analyzed and managed with available data, and concentrated enough that one or two well-targeted plan design decisions can produce meaningful improvements in long-term cost trajectory.
What Changes at 90 Employees From an Underwriting Perspective
At smaller group sizes, carriers rely heavily on broad market pricing assumptions because the group lacks sufficient statistical credibility — meaning the group’s own claims history is not reliably predictive of future utilization. At 90 employees, credibility meaningfully improves. Your group typically produces enough claims volume that utilization patterns become statistically visible, which creates an advantage when the plan is structured efficiently and claims performance is favorable — because favorable experience can now be reflected in pricing rather than being absorbed into a broad pool.
Credibility also works in the other direction. If specialty pharmacy is trending upward, if emergency room utilization is higher than expected, or if network misalignment is routing employees into higher-cost hospital systems for services available at lower-cost outpatient facilities, those patterns will contribute more directly to renewal pressure than they would in a smaller group. The employer that manages well at 90 employees is the employer who has established the governance infrastructure to identify and respond to those patterns throughout the plan year rather than discovering them at renewal when options are limited.
This requires treating healthcare as a governed financial system. That means selecting a funding structure that matches the organization’s goals for transparency and cost accountability, building a plan design that aligns employee incentives with appropriate utilization behavior, and using ongoing reporting to make smaller, targeted improvements throughout the year — rather than making large, disruptive changes at renewal under time pressure without adequate data to guide the decisions.
Group Health Insurance Options Available at 90 Employees
Organizations with 90 employees typically qualify for multiple funding structures, and the differences between them — in terms of cost transparency, employer financial exposure, and long-term premium predictability — are substantial. Fully insured plans remain available but are rarely the most cost-effective option when leadership wants meaningful transparency, improved renewal stability, and the ability to benefit financially from good claims performance. Understanding the realistic options at this size — and which structures are best suited to different organizational goals, risk tolerances, and administrative capacities — is the foundation of a strategic benefits approach.
Level-funded and partially self-funded plans are widely accessible at 90 employees and increasingly represent the mainstream approach for mid-market employers who want better alignment between actual claims performance and premium cost. These models create a more direct connection between what the organization pays and what the plan actually spends, while using stop-loss insurance to protect against individual large claims and aggregate annual cost volatility. Our resource on minimum employees for group health insurance explains which structures are realistically available at different group sizes and how participation and contribution requirements work across funding models.
Fully Insured Plans: Where the Model Can Become Inefficient at This Size
Fully insured plans offer genuine simplicity — the employer pays a fixed monthly premium, the carrier administers claims, and the renewal arrives each year as a single consolidated number. For organizations that prioritize minimal governance complexity and maximum risk transfer to the carrier, fully insured coverage continues to have a place. The challenge is that the premium structure includes built-in carrier conservatism — risk load, margin, and limited transparency into actual claims activity — that creates a persistent cost inefficiency for employers whose claims experience is favorable.
At 90 employees, many employers find themselves trapped in a renewal cycle they cannot meaningfully influence: premiums increase annually, explanations from the carrier are vague or unavailable, and the realistic response options are limited to increasing employee contributions, raising deductibles, or switching carriers without addressing the underlying cost drivers. Without data and without a plan structure that connects premium to performance, the root causes of cost increases remain invisible and unaddressed. Fully insured plans may still be appropriate when an employer’s known claims profile makes alternative funding less attractive from an underwriting perspective, when leadership specifically wants to minimize administrative involvement, or when organizational circumstances create a strong preference for fixed monthly costs regardless of claims performance. But for most 90-employee organizations with reasonably stable claims history, alternative funding structures provide a more advantageous long-term cost trajectory.
Level-Funded Group Health Insurance for 90 Employees
Level-funded group health insurance is often the most accessible entry point into alternative funding for employers at 90 employees who want better cost alignment without a significant shift in how they manage or budget for healthcare. The structure provides predictable monthly payments — making it familiar and manageable for finance teams — while creating a direct pathway for the employer to benefit from favorable claims performance in ways that fully insured plans do not allow.
In most level-funded designs, the fixed monthly payment includes three components: an estimated claims fund that is drawn against as claims are paid, administrative fees that cover plan management and reporting, and stop-loss premium that provides protection against large individual claims and aggregate annual cost overruns. From a cash flow and budgeting perspective, the monthly commitment resembles a fully insured premium — but the underlying structure is fundamentally different because the employer’s payment is directly connected to what the plan is actually spending.
At year-end, if claims are lower than the estimated fund amount, unused claim dollars may be refunded to the employer under the terms of the specific plan design. This creates a direct financial incentive for efficient claims management that fully insured plans simply do not provide — and over a multi-year period, that incentive compounds into a meaningful structural cost advantage for employers whose plans perform well. Level-funded plans also tend to produce more stable renewals over time because pricing is anchored more closely to the employer’s actual claims experience than to broad market trend factors, which reduces the “random walk” feel of fully insured renewal cycles.
Partially Self-Funded Plans and the Value of Cost Transparency
Partially self-funded group health plans are increasingly common at 90 employees because they combine meaningful financial protection — through stop-loss insurance that caps individual and aggregate exposure — with a significantly higher level of transparency into where healthcare dollars are actually being spent. Instead of paying fixed premiums that bundle claims, administration, and risk margin into a single opaque number, employers pay claims as they occur within a capped maximum and receive detailed reporting on utilization, cost drivers, and plan performance.
That transparency is the primary strategic advantage of partial self-funding at this size. When leadership can see where spend is concentrated — whether in specialty pharmacy, high-cost facility charges, emergency room utilization, or specific chronic condition management — they can apply targeted interventions that actually address the drivers of cost rather than reacting to aggregate premium increases without understanding their source. For organizations new to this approach, our resource on what self-funded group health insurance is explains how the structure works, and the pros and cons of self-funded group health helps evaluate whether the model aligns with the organization’s goals and administrative capacity.
Partial self-funding at 90 employees is not about taking on unlimited financial risk. Stop-loss insurance creates a defined maximum exposure for both individual large claimants and total annual costs, providing financial certainty within a structure that also provides cost transparency and performance accountability. The employer knows the worst-case financial boundary for the year, and everything within that boundary is managed with real data rather than estimated through broad market assumptions.
Stop-Loss Strategy: Controlling Risk While Maintaining Accountability
Stop-loss insurance is the mechanism that makes alternative funding practically viable for employers who want cost transparency and performance accountability without accepting unlimited financial exposure. At 90 employees, the right stop-loss structure is a critical design decision — not an afterthought — because it determines the financial boundaries within which the employer operates and the level of stability leadership can confidently communicate to finance and ownership.
Stop-loss protection typically addresses two distinct risk categories. Specific or individual stop-loss caps the employer’s exposure for any single claimant’s claims in a plan year — once a covered individual’s paid claims exceed the specific deductible, the stop-loss carrier reimburses claims above that threshold. Aggregate stop-loss caps total plan-year spending across all claimants as a percentage of expected claims — providing a ceiling on total financial exposure when multiple high-cost events occur simultaneously. Together, these two layers create a defined financial maximum that allows the employer to commit to alternative funding with confidence rather than uncertainty.
At Diversified Insurance Brokers, stop-loss strategy is evaluated alongside plan design and funding structure as an integrated system. The right specific deductible and aggregate attachment point depend on the employer’s budget tolerance, enrollment stability, risk appetite, and what level of year-to-year variability is acceptable in exchange for the transparency and long-term cost efficiency that alternative funding provides. There is no universal answer — the right stop-loss structure is the one that fits the organization’s specific financial profile and governance objectives.
Reducing Group Health Insurance Costs Without Cutting Benefits
At 90 employees, sustainable long-term cost reduction almost never comes from reducing benefit levels or shifting large additional costs to employees through higher deductibles. Benefit cuts can materially harm recruitment and retention in competitive labor markets, reduce employee morale in ways that affect productivity and engagement, and create downstream costs when employees defer necessary care and present with more serious and more expensive conditions later. Mid-market employers who achieve consistent, sustainable cost improvement typically do so by improving the efficiency of the healthcare system they are funding — not by making the benefit less valuable to employees.
The primary levers for meaningful cost improvement at 90 employees are network alignment, pharmacy strategy, and plan design that influences utilization behavior. Network fit determines the unit costs the plan pays for equivalent services — two plans with identical benefit structures can produce dramatically different claim costs simply because their underlying network contracts negotiate different rates with the same providers. Pharmacy management, particularly for specialty and high-cost medications, can be one of the most impactful levers available, especially as specialty drug utilization becomes an increasingly significant component of overall plan spend. Plan design can reduce waste by shaping how employees access care — encouraging primary care and urgent care for appropriate situations while discouraging avoidable emergency room visits and unnecessary high-cost facility settings.
Network Strategy: Reducing Unit Cost Without Disrupting the Employee Experience
Two benefit plans can appear essentially identical from an employee perspective — same deductible, same copayment structure, same covered services — while producing materially different financial outcomes for the employer because the underlying network contracts negotiate different unit prices for equivalent services. Network strategy at 90 employees should be deliberate and based on where employees actually live and where they actually receive care, not simply selected because a network is familiar or because it appeared in the prior carrier’s presentation.
Network strategy also shapes site-of-care behavior in ways that significantly affect total plan spend. When employees routinely receive diagnostic services, outpatient procedures, or routine specialist care in hospital outpatient settings — because the plan design does not distinguish between settings or because the network doesn’t create differential incentives — the plan pays hospital facility charges for services that could be obtained at equivalent quality in lower-cost outpatient settings. A deliberate network and site-of-care strategy reduces that unnecessary spend while keeping access straightforward and the employee experience unchanged.
Employers who address network fit strategically often find that they can improve cost efficiency meaningfully without cutting any benefit and without creating the employee frustration that typically accompanies benefit reductions. The savings come from the system — from paying the right price to the right provider in the right setting — rather than from shifting costs onto the employee population.
Pharmacy Strategy: The Most Concentrated Cost Driver in Mid-Market Plans
Pharmacy — particularly specialty pharmacy — is frequently the most concentrated and most rapidly growing cost driver in mid-market employer health plans, and it requires explicit strategic attention at 90 employees rather than being treated as a background element of the benefit structure. Specialty medications can represent a disproportionate share of total plan spend even when only a small percentage of enrolled members use them, because individual specialty drug costs can reach tens or hundreds of thousands of dollars annually per member for some conditions. When specialty drug trends are unmanaged, they can create renewal pressure that dwarfs any savings from other plan design improvements.
Effective pharmacy strategy at this size addresses formulary design, specialty drug management processes, generic utilization incentives, mail order programs, and coordination with pharmacy benefit management structures to ensure the plan is paying net competitive prices for medications across all tiers. The goal is not to restrict clinically necessary medications — employees need appropriate pharmaceutical care, and restricting access creates its own downstream costs and retention risks — but to ensure that medications are being obtained through the most cost-efficient channels, at the most competitive net prices, with appropriate management of specialty utilization to avoid unnecessary trend.
Plan Design Alignment: Reducing Waste Without Shifting Financial Pain to Employees
The most effective plan designs at 90 employees reduce waste by shaping utilization behavior — encouraging clinically appropriate care choices — rather than simply shifting costs to employees through higher deductibles and out-of-pocket maximums. Raising the deductible is a commonly used short-term cost reduction strategy, but it rarely produces sustainable improvement because it does not change the underlying utilization patterns that drive cost. It transfers financial risk from the plan to the employee, which can reduce claims temporarily as employees defer care, but that deferral often produces higher-cost events later when conditions progress.
Plan designs that work at 90 employees typically make primary care accessible and affordable so employees use it regularly rather than defaulting to emergency rooms for non-urgent situations. They support preventive care actively so chronic conditions are identified and managed earlier when management is less expensive. They create clear and reasonable cost differentials between high-value care settings and low-value settings so employees have a genuine financial incentive to choose appropriately — not a prohibitive barrier to any care. And they make care navigation simple enough that employees can make good decisions without requiring significant research or system navigation expertise that most people do not have.
Refund Opportunities and Renewal Stability Through Performance Alignment
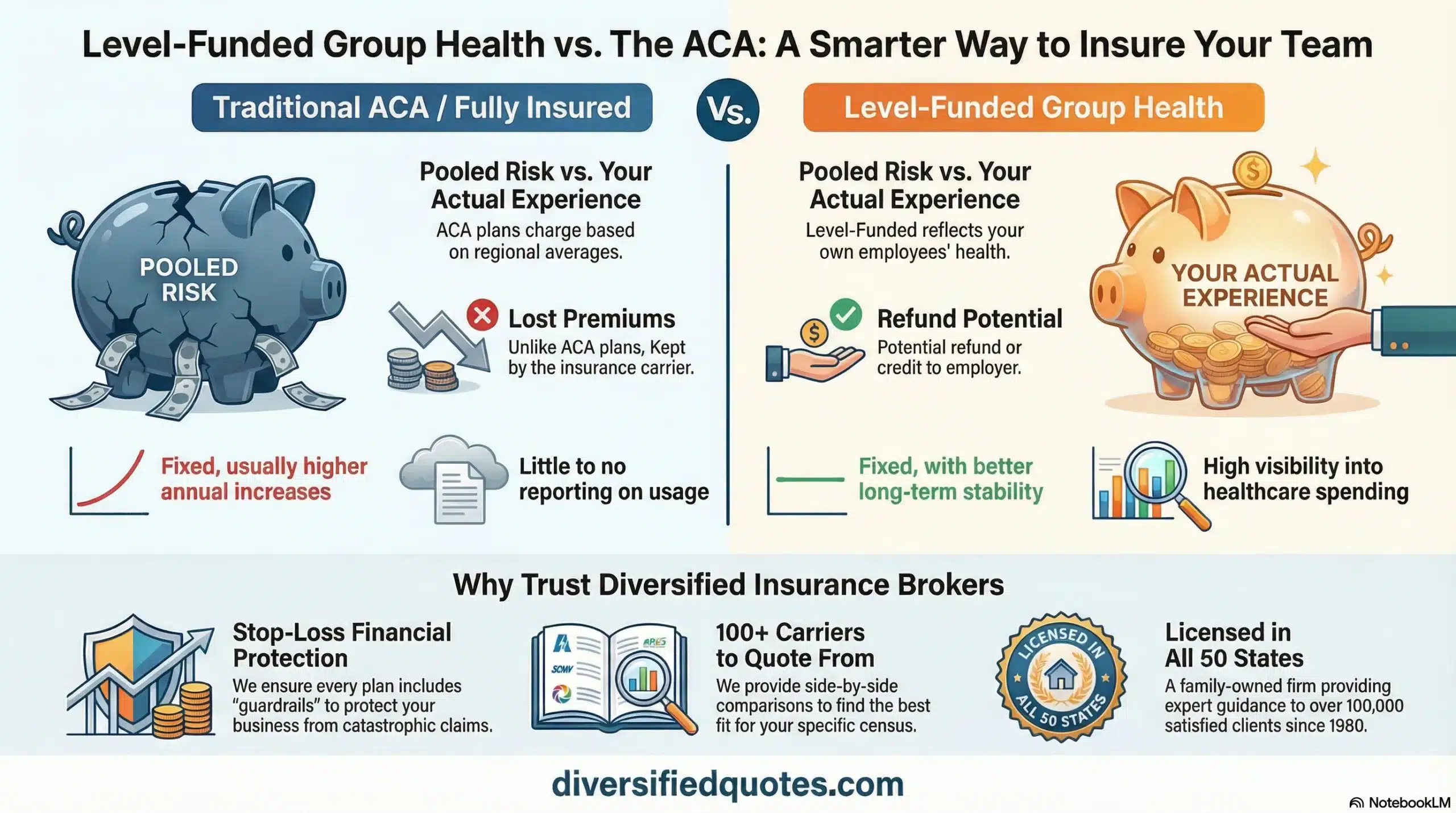
One of the most meaningful structural advantages of alternative funding models over fully insured plans at 90 employees is the alignment between claims performance and what the employer actually pays. Fully insured plans provide no financial reward for favorable claims experience — even in a year where the plan performs significantly below the carrier’s projected claims budget, the employer receives no refund and typically does not receive a favorable renewal as a direct result of that performance. The carrier retains the financial benefit of favorable experience.
Level-funded and self-funded structures change this dynamic fundamentally. When claims are lower than projected, unused claim dollars may be returned to the employer or credited toward future plan costs. When claims performance is consistently favorable over multiple years, renewal pricing reflects that history more directly than fully insured pricing structures typically allow. Over a three to five-year horizon, that alignment produces meaningfully better budgeting predictability and creates a direct financial return on investments in plan design improvement, network optimization, and pharmacy management that would not be captured under a fully insured structure.
Claims Reporting and Governance: Turning Data Into Actionable Decisions
At 90 employees, claims reporting is one of the most valuable differentiators between alternative funding models and traditional fully insured plans — but only when the reporting is structured to support decisions rather than to produce data for its own sake. The goal of reporting at this size is not to generate comprehensive statistical summaries. It is to answer the practical questions that leadership needs to make better plan decisions throughout the year: Are cost increases driven by medical or pharmacy? Are a small number of high-cost claimants driving a disproportionate share of total spend? Is emergency room utilization elevated relative to benchmarks? Are site-of-care patterns routing employees into unnecessarily expensive settings? Are specific chronic conditions being actively managed or progressively escalating?
When those questions have clear answers supported by reliable data, employers can make targeted, incremental improvements throughout the plan year — intervening where cost is actually concentrated rather than making broad, disruptive changes that affect the entire plan at renewal. This governance model — continuous monitoring, targeted intervention, and incremental improvement — is typically what separates employers who feel genuinely in control of their healthcare costs from those who feel perpetually reactive to external factors they cannot influence.
Planning Beyond 90 Employees
The group health strategy chosen and implemented at 90 employees significantly influences how smoothly and cost-effectively an organization scales into larger group categories. Employers who establish transparent, data-driven funding structures and effective plan governance at this size typically experience less disruption and fewer compounding cost problems as they grow — because the infrastructure for managing healthcare costs efficiently is already in place. Those who delay strategic investment in plan design and governance often find that inefficiencies compound as the group grows larger, costs become harder to correct, and the options available for improvement narrow as claims history becomes more entrenched.
At 90 employees, the combination of sufficient scale to implement more sophisticated strategies and manageable size to execute the transition without excessive disruption creates a genuine “sweet spot” for strategic plan redesign. If your current plan feels like a black box — renewals arrive without clear explanations, costs rise without obvious levers for improvement, and leadership feels like a price-taker rather than a decision-maker — this is precisely the size and the moment where a strategic review can create clarity, stability, and a substantially better long-term cost trajectory.
Compare Group Health Options for 90 Employees
Compare fully insured, level-funded, and partially self-funded plans side by side based on your organization’s cost profile and goals.
Compare Funding OptionsStabilize Renewals for a 90-Employee Plan
We’ll identify the biggest cost drivers in your current plan and show practical ways to improve predictability without cutting benefits or disrupting the employee experience.
Request a Group Health ReviewFinancial Protection Essentials
Medicare updates, retirement rollover strategies, group coverage planning, and dental insurance comparison resources.
Related Pages
Explore additional group health resources for small employers and growing teams.
Talk With an Advisor Today
Choose how you’d like to connect—call or message us, then book a time that works for you.
Schedule here:
calendly.com/jason-dibcompanies/diversified-quotes
Licensed in all 50 states • Fiduciary, family-owned since 1980
FAQ: Group Health Insurance for 90 Employees
Yes — employers with 90 employees typically qualify for a full range of group health insurance funding structures, including fully insured plans, level-funded designs, and partially self-funded arrangements with stop-loss protection. At 90 employees, the group is large enough to qualify for most mid-market plan structures that are not available to smaller groups, and small enough that the implementation and governance transition remains manageable. Availability of specific plan designs depends on participation requirements, contribution levels, and the group’s claims history and demographic profile, but most organizations at this size have multiple viable funding options to compare.
Refunds are possible under level-funded plan designs, where unused claim dollars — the portion of the monthly payment allocated to claims funding that was not spent on actual claims — may be returned to the employer at the end of the plan year, subject to the specific plan’s terms and stop-loss recovery provisions. Under partially self-funded arrangements, employers benefit directly from favorable claims performance by paying lower total claims costs during the year, which produces a similar financial outcome to a refund through reduced expenditure rather than a year-end check. Fully insured plans do not provide refunds or financial rewards for favorable claims experience — the carrier retains the benefit of any favorable deviation from projected claims under a fully insured structure. The potential for refunds and direct financial alignment with claims performance is one of the primary reasons mid-market employers explore alternative funding at 90 employees.
Partial self-funding at 90 employees carries manageable, defined, and quantifiable financial risk when structured correctly with appropriate stop-loss insurance — it is not the same as unlimited self-insurance with uncapped financial exposure. Stop-loss insurance provides two layers of financial protection: specific or individual stop-loss caps the employer’s financial exposure for any single claimant’s claims within the plan year, so catastrophically expensive individual cases are shared with the stop-loss carrier above the specific deductible threshold. Aggregate stop-loss caps total annual claims spending across all members, providing a ceiling on the employer’s total financial exposure for the plan year even if multiple high-cost events occur simultaneously. When both layers are appropriately sized to the employer’s budget tolerance and financial profile, the organization knows its worst-case annual healthcare cost boundary in advance — making self-funding a defined and manageable financial commitment rather than an open-ended risk. The financial risk of partial self-funding is typically more predictable and more transparent than the hidden inefficiencies embedded in fully insured premiums that never return value to the employer regardless of claims performance.
Most group health plan implementations at 90 employees can be completed within four to eight weeks from carrier selection to coverage effective date, assuming underwriting, enrollment, and administrative setup proceed on schedule. The timeline has several components: underwriting review of the application and any required claims experience data, carrier approval and plan documentation, employee enrollment and benefit communication, ID card and coverage document distribution, and administrative system setup for payroll deduction and billing. More complex plan structures — particularly self-funded arrangements that involve stop-loss carrier selection, third-party administrator setup, and network contracting — may require additional time. Organizations that want to transition between plan years on a specific anniversary date should begin the review and selection process at least 60 to 90 days before the intended effective date to allow sufficient time for a thorough evaluation, underwriting, and implementation without time pressure.
Yes — plans built around transparency, data-driven governance, and alternative funding structures scale more effectively as employee count increases than plans built around fully insured simplicity without underlying cost management infrastructure. As the employer grows from 90 to 100, 150, or 250 employees, the claims credibility of the group increases, the available funding options expand, and the potential benefit of good claims governance compounds. Organizations that establish effective reporting, clear cost accountability, and appropriate funding structures at 90 employees typically find that their healthcare cost management improves — rather than deteriorating — as they scale, because the infrastructure is already in place. Those that delay this investment often find that scaling amplifies inefficiencies rather than resolving them, because cost patterns become more entrenched and harder to correct at larger sizes without significant disruption.
Both level-funded and partially self-funded plans involve the employer bearing some claims risk rather than transferring all risk to an insurance carrier, and both use stop-loss insurance to limit that risk — but they differ in structure, transparency, and administrative complexity. Level-funded plans provide a fixed monthly payment similar to a fully insured premium, but the payment is broken into claims funding, administrative fees, and stop-loss premium components that are more transparent than a fully insured all-in premium. Claims are typically administered by the carrier or a designated administrator under a more standardized structure, and reporting is usually simpler than fully self-funded arrangements. Partially self-funded plans typically involve more flexibility in plan design, more detailed and customizable reporting, more direct employer control over specific plan provisions, and often a broader menu of third-party vendor options for pharmacy, care management, and utilization management. Self-funded plans generally provide more granular data and more customization but require more active governance and administrative engagement than level-funded designs. Both are significant improvements over fully insured plans in terms of cost alignment and transparency at 90 employees.
Pharmacy cost management at 90 employees involves several interconnected strategies that address both routine prescription costs and the specialty drug spending that often drives the most significant cost trend in mid-market plans. At the formulary level, effective pharmacy management involves tiering that directs members toward lower-cost therapeutically equivalent options where available, while ensuring that clinically necessary medications remain accessible without creating barriers to appropriate care. Specialty pharmacy management addresses the small number of extremely high-cost medications — biologics, oncology drugs, specialty infusions — that can individually consume a significant share of the plan’s total pharmaceutical budget. For specialty medications, strategies include ensuring drugs are obtained through the most cost-efficient channels, that appropriate clinical criteria for coverage are applied, and that the plan is paying competitive net prices after manufacturer rebates and other cost offsets. Generic substitution programs, mail order for maintenance medications, and coordination with the pharmacy benefit manager are the foundational tools, while specialty drug management requires more intensive clinical and financial oversight that is typically only accessible through alternative funding structures with appropriate vendor relationships.
Participation requirements for group health insurance at 90 employees vary by plan type, funding structure, and the carrier or administrator selected. Fully insured plans typically require that a minimum percentage of eligible employees — commonly 50 to 75 percent of those without coverage through another group plan — participate in the employer’s plan. Level-funded and self-funded arrangements often have more flexible participation thresholds than fully insured plans, particularly when the employer’s contribution level is competitive and the plan design is attractive to employees across different utilization profiles. Participation matters for several interconnected reasons: adequate participation distributes risk across a broader population rather than concentrating it among higher-utilization employees who are most motivated to enroll; broader participation improves statistical credibility for underwriting and renewal purposes; and strong participation typically creates a more favorable claims environment because healthier employees participate alongside those who regularly use the plan. Employer contribution strategy directly influences participation — higher employer contributions increase enrollment, broaden the risk pool, and generally improve plan performance and renewal stability over time.
Evaluating current plan performance at 90 employees requires access to claims data at a level of detail that fully insured plans often do not provide — which is itself a signal about the plan’s structure. Strong performance evaluation compares total plan cost per member against industry benchmarks for comparable employer populations, separates medical and pharmacy cost trends to identify where increases are concentrated, evaluates site-of-care patterns to identify whether employees are accessing care in cost-efficient settings, assesses emergency room utilization against expectations given the employee population and available alternatives, and examines specialty pharmacy spend relative to benchmarks. It also involves comparing the current renewal’s actuarial basis against the actual claims experience to determine whether the carrier is pricing based on your group’s actual performance or on conservative assumptions that do not reflect your claims history. If you cannot access the data needed to answer these questions from your current plan structure, that gap itself is meaningful evidence that a more transparent funding model would provide better information for strategic decision-making.
Preparing effectively for a group health plan review at 90 employees involves gathering several key pieces of information that allow for a meaningful strategic assessment rather than a simple premium comparison. Current plan documentation — the summary plan description, carrier benefit summaries, and the most recent renewal communication — provides the baseline benefit structure and cost information. Claims experience data for the most recent 24 to 36 months, if available from the current carrier, enables analysis of utilization trends, cost drivers, and comparison against benchmarks. Current employer and employee contribution levels help assess whether the contribution strategy is optimally structured for participation and retention. Employee census data — ages, dependent coverage elections, and ZIP code distribution — supports network analysis and underwriting assessment. Information about any known upcoming high-cost medical situations allows stop-loss strategy to be appropriately designed. With this information assembled, a strategic review can identify specific opportunities for improvement across funding structure, plan design, network strategy, and pharmacy management — rather than simply comparing premiums without understanding the underlying cost dynamics.
About the Author:
Jason Stolz, CLTC, CRPC, DIA, CAA and Chief Underwriter at Diversified Insurance Brokers (NPN 20471358), is a senior insurance and retirement professional with more than 25 years of real-world experience helping individuals, families, and business owners protect their income, assets, and long-term financial stability. As a long-time partner of the nationally licensed independent agency Diversified Insurance Brokers, Jason provides trusted guidance across multiple specialties—including fixed and indexed annuities, long-term care planning, personal and business disability insurance, life insurance solutions, Group Health, and short-term health coverage. Diversified Insurance Brokers maintains active contracts with over 100 highly rated insurance carriers, ensuring clients have access to a broad and competitive marketplace.
His practical, education-first approach has earned recognition in publications such as VoyageATL, highlighting his commitment to financial clarity and client-focused planning. Drawing on deep product knowledge and years of hands-on field experience, Jason helps clients evaluate carriers, compare strategies, and build retirement and protection plans that are both secure and cost-efficient. Visitors who want to explore current annuity rates and compare options across multiple insurers can also use this annuity quote and comparison tool.
Explore More Group Health Insurance Options: Browse our complete guide to Group Health Insurance by Company Size — covering plans for 2, 10, 20, 50, 100, 250, 500, 750 & 1,000+ employees from 100+ carriers.
